No cracking under pressure

Patients who need dental implants but have thin gums or are allergic to titanium may benefit from a new, stronger ceramic dental implant approved by the U.S. Food and Drug Administration in January.
While there have been other ceramic dental implants in the past, these did not always hold up to the bite pressure needed for normal use, said Stefanie Seitz, D.D.S., assistant professor of comprehensive dentistry. The new ceramic implants, now available through UT Dentistry, have shown comparable strength to titanium, the standard material used for dental implants.
“This is somewhat of a niche product for patients who have special circumstances,” Dr. Seitz said. “By their nature, titanium implants can compromise aesthetics by showing gray through the gum tissue. This ceramic implant is ivory in color, thereby mimicking the natural color of teeth, making it more aesthetic. The ceramic implants are also helpful for patients who are allergic to titanium or, for whatever reason, do not want to have metal in
their bodies.”
New imaging technology is used to plan and place both ceramic and titanium implants in a way that results in precise placement, less pain for the patient and faster healing.
The technology calls for dentists to perform a digital scan of the teeth instead of using a thick, pasty dental material to get an impression of the mouth. The digital data are put into a 3-D implant planning software program to determine the exact location, appropriate depth and angle for the implant. The program provides coordinates for the manufacturer to make a 3-D resin “guide,” or template, to place the implant. A hole in the template for the implant guides the dental surgeon for exact placement.
The ceramic implant is placed with a protective cap to allow for the three- to four-month healing phase before the tooth can be used for chewing.
Ceramic implants can be used for single implants or groups of teeth. Although the ceramic implant is available to all implant patients, the cost is higher than titanium implants, Dr. Seitz said.
Viva Fiesta!
 It’s called the Party with a Purpose, the two-week long Fiesta San Antonio festival that began 125 years ago as a remembrance of the heroes of the Alamo and the Battle of San Jacinto.
It’s called the Party with a Purpose, the two-week long Fiesta San Antonio festival that began 125 years ago as a remembrance of the heroes of the Alamo and the Battle of San Jacinto.
For the first time in many years, the Health Science Center joined in the festivities by sponsoring a float during the Texas Cavaliers River Parade, themed “River of Champions,” on the San Antonio River downtown. The university’s float, titled “Champions of the Cure,” honored Dot Delarosa, a lung transplant survivor, and 14-year-old Raven Labrador, a patient with acute lymphoblastic leukemia.
Others on the float included Health Science Center President William L. Henrich, M.D., MACP, and his wife, Mary; Presidential Ambassador Scholars Award recipients; and the band Morning, led by dentistry faculty member Bud Luecke III, D.D.S., M.S.D.
The money raised through the parade is donated to children’s charities in the San Antonio area through the Texas Cavaliers Charitable Foundation.

A gift of hope

A $1 million gift from Ed and Linda Whitacre will support the pilot cancer therapeutic clinical trials program at the Cancer Therapy & Research Center (CTRC) as well as fund an education and awareness campaign to highlight the clinical trials and expertise available to patients battling cancer.
Increasing the number of clinical trials for cancer patients in San Antonio and South Texas, and raising awareness among patients and physicians of new innovative therapies are among the central goals in the CTRC’s strategic plan.
Ian M. Thompson Jr., M.D., director of the CTRC, said the gift is critically important for the CTRC to ensure delivery of the cancer center’s responsibilities to patients in San Antonio and South Texas as the region’s only National Cancer Institute-designated cancer center.
“We are deeply grateful to Linda and Ed Whitacre for their generosity in helping us provide the most advanced new therapies for our patients and ensuring that every single patient in San Antonio and South Texas is aware of these unique opportunities,” he said. “Their gift will accelerate the development of new cancer cures through the work of our extensive teams of scientists and physicians, the same ones who treat our patients every single day at the CTRC.”
Appointments and awards
 A paper published by Sunil K. Ahuja, M.D., was ranked as one of the top 20 scientific advances made by National Institute of Allergy and Infectious Diseases-funded researchers in 2015. The paper demonstrates the immune-health benefits of early HIV treatment.
A paper published by Sunil K. Ahuja, M.D., was ranked as one of the top 20 scientific advances made by National Institute of Allergy and Infectious Diseases-funded researchers in 2015. The paper demonstrates the immune-health benefits of early HIV treatment.
 Janie Canty-Mitchell, Ph.D., has been named chair of the Healthcare Diversity Council board of directors. Dr. Canty-Mitchell serves as professor and chair of the Department of Family and Community Health Systems and interim chair of the Department of Health Restoration and Care Systems Management in the School of Nursing.
Janie Canty-Mitchell, Ph.D., has been named chair of the Healthcare Diversity Council board of directors. Dr. Canty-Mitchell serves as professor and chair of the Department of Family and Community Health Systems and interim chair of the Department of Health Restoration and Care Systems Management in the School of Nursing.
 Deborah L. Conway, M.D., has been appointed interim chair of the Department of Obstetrics and Gynecology. She currently is associate dean for curriculum in the Office of Undergraduate Medical Education. Dr. Conway is a Fellow of the American College of Obstetrics & Gynecology and is board certified in obstetrics and gynecology and maternal-fetal medicine. Her clinical and research area of focus is diabetes in pregnancy.
Deborah L. Conway, M.D., has been appointed interim chair of the Department of Obstetrics and Gynecology. She currently is associate dean for curriculum in the Office of Undergraduate Medical Education. Dr. Conway is a Fellow of the American College of Obstetrics & Gynecology and is board certified in obstetrics and gynecology and maternal-fetal medicine. Her clinical and research area of focus is diabetes in pregnancy.
 Edward Ellis, D.D.S., received the first American Association of Oral and Maxillofacial Surgeons Clinical Research Award for Fellows and Members. The award recognizes leaders in the specialty who are researching new and innovative diagnostic and therapeutic interventions that will advance clinical practice.
Edward Ellis, D.D.S., received the first American Association of Oral and Maxillofacial Surgeons Clinical Research Award for Fellows and Members. The award recognizes leaders in the specialty who are researching new and innovative diagnostic and therapeutic interventions that will advance clinical practice.
 Luci K. Leykum, M.D., professor of medicine, was named chief of the newly created Division of General and Hospital Medicine. Dr. Leykum was associate dean for clinical affairs since 2010, and has been division chief of hospital medicine since 2008. In her new position, she will work with the 60 faculty from the combined divisions to support and build on their educational, clinical and research endeavors.
Luci K. Leykum, M.D., professor of medicine, was named chief of the newly created Division of General and Hospital Medicine. Dr. Leykum was associate dean for clinical affairs since 2010, and has been division chief of hospital medicine since 2008. In her new position, she will work with the 60 faculty from the combined divisions to support and build on their educational, clinical and research endeavors.
 Craig Manifold, D.O., clinical assistant professor in the Department of Emergency Medicine, received the Michael Copass Leadership Award from the Major Metropolitan Medical Directors for his efforts in leading emergency management services nationwide.
Craig Manifold, D.O., clinical assistant professor in the Department of Emergency Medicine, received the Michael Copass Leadership Award from the Major Metropolitan Medical Directors for his efforts in leading emergency management services nationwide.
 Michael Mills, D.M.D., M.S., received the American Academy of Periodontology Outstanding Periodontal Educator Award. Dr. Mills is a clinical associate professor with teaching responsibilities in the postdoctoral division of the Department of Periodontics in the School of Dentistry.
Michael Mills, D.M.D., M.S., received the American Academy of Periodontology Outstanding Periodontal Educator Award. Dr. Mills is a clinical associate professor with teaching responsibilities in the postdoctoral division of the Department of Periodontics in the School of Dentistry.
 Basil A. Pruitt Jr., M.D., FACS, a clinical professor and burn surgeon, received the Lifetime Achievement Award from AMSUS, the Society of Federal Health Professionals.
Basil A. Pruitt Jr., M.D., FACS, a clinical professor and burn surgeon, received the Lifetime Achievement Award from AMSUS, the Society of Federal Health Professionals.
 W. Brian Reeves, M.D., was named chair of the Department of Medicine in the Long School of Medicine. Dr. Reeves is a former professor and vice chair of medicine and chief of the Division of Nephrology at Penn State College of Medicine.
W. Brian Reeves, M.D., was named chair of the Department of Medicine in the Long School of Medicine. Dr. Reeves is a former professor and vice chair of medicine and chief of the Division of Nephrology at Penn State College of Medicine.
 David Senn, D.D.S., clinical assistant professor of comprehensive dentistry, was named president of the American Society of Forensic Odontology. Dr. Senn is the director of the Center for Education and Research in Forensics, director of postdoctoral fellowship in forensic odontology, director of the Southwest Symposium on Forensic Dentistry, and chief forensic odontologist for the Bexar County Medical Examiner’s Office.
David Senn, D.D.S., clinical assistant professor of comprehensive dentistry, was named president of the American Society of Forensic Odontology. Dr. Senn is the director of the Center for Education and Research in Forensics, director of postdoctoral fellowship in forensic odontology, director of the Southwest Symposium on Forensic Dentistry, and chief forensic odontologist for the Bexar County Medical Examiner’s Office.
 David Weiss, Ph.D., was named a University of Texas System Chancellor’s Health Fellow in Graduate Education. The program was established in 2004 to recognize high-impact work at individual health institutions that are aligned with the overarching mission of the UT System and have potential for broad societal impact on health care education and research.
David Weiss, Ph.D., was named a University of Texas System Chancellor’s Health Fellow in Graduate Education. The program was established in 2004 to recognize high-impact work at individual health institutions that are aligned with the overarching mission of the UT System and have potential for broad societal impact on health care education and research.
Endovascular Experts

V. Seenu Reddy, M.D., M.B.A.
- Assistant professor
- Director of thoracic aortic surgery
- Associate director of the thoracic residency program
- Director of emerging technology in the division of thoracic surgery
Maureen Sheehan, M.D.
- Assistant professor in the division of vascular surgery
Boulos Toursarkissian, M.D.
- Associate professor
- Chief of the division of vascular surgery
All about the Aorta
 The aorta is the body’s largest artery. Shaped like a candy cane and about the diameter of a garden hose, the aorta extends from the heart down through the chest and abdomen, where it divides into a vessel that carries blood to the abdominal organs and legs.
The aorta is the body’s largest artery. Shaped like a candy cane and about the diameter of a garden hose, the aorta extends from the heart down through the chest and abdomen, where it divides into a vessel that carries blood to the abdominal organs and legs.
Aneurysms
Aneurysms can develop anywhere in the aorta. An aortic aneurysm is an abnormal bulge in the wall of the aorta. Up to 25 percent of aortic aneurysms are thoracic.
Diagnosis
 An aortic aneurysm may be detected during an evaluation of a patient’s history or during a physical exam. Many are found during routine medical tests such as chest X-rays, CT scans and ultrasounds.
An aortic aneurysm may be detected during an evaluation of a patient’s history or during a physical exam. Many are found during routine medical tests such as chest X-rays, CT scans and ultrasounds.
Treatment
Treating an aortic aneurysm depends on its size, type and location in the body as well as a patient’s overall health. If an aneurysm is large enough to demand surgery, or tests reveal that the aneurysm is quickly enlarging or leaking, immediate surgery may be recommended. If an aneurysm is small and asymptomatic, physicians may decide to take a "watch-and-wait" approach.
Patients who undergo the endovascular procedure benefit from decreased postoperative pain, a shorter recovery period and a reduced chance of complications. Because the technique is relatively new, patients require long-term surveillance.
ENDOVASCULAR vs. OPEN
- ICU stay: 1-3 days vs. 3-5 days
- Hospital stay: 3-5 days vs. 7-13 days
- Rate of complications: 5% vs. 20%
Figures are average and vary according to patient.
Gift of life
"To know even one life has breathed easier because you
have lived, this is to have succeeded."
- Ralph Waldo Emerson
Larysa Sholom was 16 when she arrived in the United States from the Ukraine as an exchange student. With great trepidation but courage, she left her family behind to pursue an education and expand her horizons. Years later, her love for the U.S. often brought her back to visit. But in 2008, while vacationing in San Antonio, a debilitating disease kept her from returning to her homeland.
At 21 years old, Sholom was diagnosed with Lymphangioleiomyomatosis, a rare lung disease that left her gasping for air. The disease, which affects mostly women, is characterized by the overgrowth of abnormal cells that destroy lung tissue. The cause of the disease is not yet understood and no cure exists. Sholom expected she had only one year to live.
With a fighting spirit, Sholom continued to pursue her dreams in America and landed a job as a supply and trading associate at NuStar Energy LP in San Antonio, one of the largest asphalt refiners and marketers in the U.S. and the second largest independent liquids terminal operator in the nation.
When NuStar Board Chairman Bill Greehey, who is fiercely loyal to his community and employees, learned of Sholom’s plight, he quickly referred her to the UT Health Science Center and the physicians of UT Health San Antonio. Greehey, a longtime and deeply generous supporter of the Health Science Center, said he was confident UT Medicine physicians could help her. NuStar’s CEO, Curt Anastasio, agreed and helped facilitate the referral.

"We are fortunate to have the UT Health Science Center in our community as it is recognized as one of the top health science centers in the nation," Greehey said. "The lifesaving and life-changing work they do for the citizens of San Antonio and South Texas is unmatched. They are saving the lives of people like Larysa every day through the groundbreaking research they conduct, the cutting-edge procedures they perform, and the special care they deliver."
Lifesaving lung transplant
On May 3, 2011, UT Medicine physician Scott B. Johnson, M.D., and his team, in a six-hour operation, performed a double-lung transplant on Sholom. Dr. Johnson is associate professor, head of the Division of General Thoracic Surgery and surgical director of the Lung Transplant Program of The University Transplant Center, a partnership of University Health System and the UT Health Science Center. Today Sholom is recovering and looking forward to fulfilling the dreams she brought with her to the U.S.

"It’s a nice thing that there’s a future. It wasn’t there before," Sholom said. "Now there are so many possibilities. I am happy and healthy and I’m extremely grateful for that. This is the gift of life."
Patients share their stories at President’s Gala
Sholom was one of two patients featured in a video presentation at the UT Health Science Center’s fifth annual President’s Gala held at the Grand Hyatt Hotel on Sept. 17. The other was Dave Ashwin, husband of Kathy Ashwin, director of the H-E-B Tournament of Champions. Ashwin was diagnosed with Stage 3 lung cancer. Jay Pal, M.D., Ph.D., a UT Health San Antonio surgeon and assistant professor of cardiothoracic surgery, performed his operation. Ashwin received follow-up treatment at the Cancer Therapy & Research Center (CTRC) at the UT Health Science Center.
"The Health Science Center has given me life," Ashwin said. "I have hope. I’m playing golf. I’m taking trips. I’m feeling wonderful. Golly, it’s just so good!"
Their stories of survival were heard by more than 1,300 community and academic leaders who attended the gala. Among the guests was Charles Butt, chairman and CEO of the H-E-B Grocery Company, a longtime member of the Health Science Center’s Development Board, and the gala’s honoree.
$500,000 establishes Charles Butt and H-E-B Excellence Fund
William L. Henrich, M.D., MACP, UT Health Science Center president, took to the stage. "These miracles would not be possible without education, without science and without the intrepid human spirit." Then he made a major announcement - the gala raised more than $500,000 to establish the Charles Butt and H-E-B Excellence Fund for the Future of Health.
Dr. Henrich saluted Charles Butt for his humility and commitment to enhancing his community.
"Where would we be without the enormous contributions of time, talent and resources given by Charles and the H-E-B partners across our state? Each one of us has benefited in some way from their generosity," he said.
Craig Boyan, president and chief operating officer of H-E-B, addressed the audience. "Education and health care are two of the major needs in the state and they are our top two priorities. This is why we are working with the Health Science Center to turn the tide in Texas and why we have donated $15 million to the Health Science Center. Dr. Henrich, we are proud of what you and your colleagues at the Health Science Center are doing. On behalf of our 76,000 employees, Charles Butt and our senior leadership team, we want you to know how much we appreciate what you are doing for the state of Texas."
The Charles Butt and H-E-B Excellence Fund for the Future of Health will support all aspects of the university’s programs and missions of education, research, clinical care and community service. It will focus on recruiting and retaining the best and brightest students and faculty and on the translation of scientific discoveries into new therapies to treat patients and benefit the community.
Health Science Center establishes Center for Public Health Preparedness and Biomedical Research
The Health Science Center has taken another proactive step in combating bioterrorism while calming public fears. The institution launched the new Center for Public Health Preparedness and Biomedical Research (CPHPBR). The CPHPBR will educate the public and train local health care providers in bioterrorism prevention and treatment. It will also facilitate research for vaccines against bioterrorist agents.
"This center will work with metro and regional health authorities to prepare exercise scenarios and provide training opportunities for emergency responders, including physicians, nurses and emergency medical services personnel," said Harold L. Timboe, M.D. "We also will provide presentations for the general public. We need to be ready for any eventuality, especially where it involves applying our health expertise."
Dr. Timboe is the associate vice president for administration at the Health Science Center and the founding director of the CPHPBR.
"Dr. Timboe is an excellent choice because of his medical and public health background and his distinguished military career, which culminated in commands at Brooke Army Medical Center and Walter Reed Army Medical Center," said Francisco G. Cigarroa, M.D., president. "This center will be uniquely tailored to the strengths of the Health Science Center, which offers many experts and programs of great value to the community and throughout South Texas in these challenging times."
Chuck Rodriguez, Ph.D., assistant vice president for university relations, will serve as the deputy director for the center.
When the doctor becomes the patient
What goes through the mind of a cancer doctor who learns he has cancer?

Ian M. Thompson Jr., M.D., director of the Cancer Therapy & Research Center, wasn’t as worried as was his wife, Donna, about the odd spot on his right ear.
She asked him to have it checked out; he was in no rush.
In reality, he didn’t have to go too far. Three floors down from his office in the CTRC, Sandra Osswald, M.D., oversees the Dermatology Clinic. Donna Thompson eventually convinced her husband to visit Dr. Osswald, who biopsied the spot. It wasn’t long before the cancer center director was told the news: He had cancer.
He was sent to Vineet Mishra, M.D., director of Mohs Surgery and Procedural Dermatology. Mohs is micrographic surgery that allows physicians to remove a tumor while leaving the surrounding healthy tissue unharmed. Dr. Mishra is one of nearly 1,200 fellowship-trained Mohs surgeons in the U.S.
“It was an early evolving melanoma,” Dr. Mishra said, “and it turned out to be more extensive than initially thought.”
Skin cancer is the most common type of cancer in the U.S., with more than 2 million Americans diagnosed each year. While melanoma isn’t as common, accounting for only 2 percent of all skin cancers, it is the most deadly. There will be an estimated 73,870 new cases of melanoma diagnosed this year, and nearly 10,000 people are expected to die in 2015 from the cancer, according to the American Cancer Society.
“Here in South Texas, we’re sitting in a hotbed of skin cancer,” Dr. Mishra said. “There is a misconception that skin cancer only affects certain races. In fact, it affects people of all races, all ages and both genders. It’s a major cause of concern.”
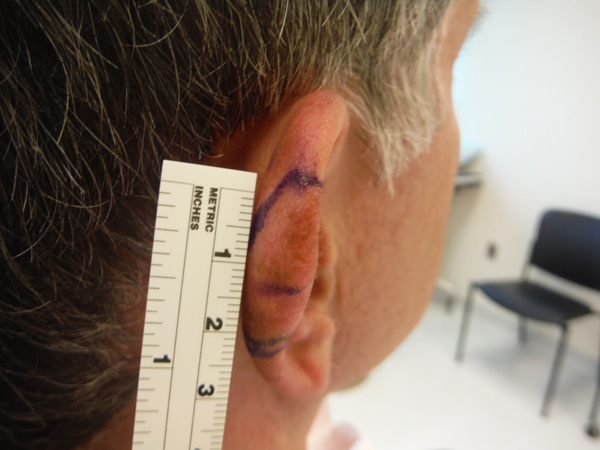
In skin cancer, a small lesion can conceal a dangerous mass with roots underneath.
Dr. Mishra compared the potential threat to that of an iceberg.
“What sank the Titanic was that which was beneath the surface,” he said.
In Dr. Thompson’s case, the lesion was especially serious because of its depth and location.
“Melanoma on the head and neck is a cause for concern,” Dr. Mishra said. “Given the routes of vascular and lymphatic drainage, it can spread to other vital structures and organs.”
“Why me?” is a question that some patients ask when faced with a frightening diagnosis, but Dr. Thompson brushed that off.
“Physicians deal with data,” said Dr. Thompson, who attended the U.S. Military Academy before earning his M.D. at Tulane University. “I can remember as a college student sitting up on the top of the gymnasium at West Point sunbathing on weekends, so there’s no ‘Why me?’ there.”
 Besides, he said, while there are clear risk factors—environmental, behavioral and genetic—a certain amount of cancer is simply bad luck. There’s no point in grappling with the past.
Besides, he said, while there are clear risk factors—environmental, behavioral and genetic—a certain amount of cancer is simply bad luck. There’s no point in grappling with the past.
The question of “What if?” is a little different.
“I spend my life with the privilege of dealing with cancer patients,” he said. “You begin to understand that what you really have is today.”
And “today” can be filled with a slew of critical decisions: What is the best treatment? Will reconstructive surgery follow?
Dr. Mishra reviewed the options with Dr. Thompson: Mohs surgery, radiation, or wide local excision. Dr. Thompson chose Mohs surgery.
With Mohs surgery, skin cancer is removed in layers. After each layer is removed, it is examined under a microscope. The process continues until healthy tissue around the cancer, or a clear margin, is reached.
“Dr. Thompson’s first layer was positive [for cancer],” Dr. Mishra said. “That’s a concern because the vast majority of patients are clear on the first layer after taking the recommended margin—which means his tumor was larger than anticipated.”
After Dr. Mishra took the second layer, the margin was clear. It was time for reconstruction surgery.
They took skin from his clavicle and sewed it on to the top of Dr. Thompson’s ear. It was challenging, Dr. Mishra said, because the cartilage has little blood supply, and a robust blood supply is needed to nourish the graft.
They fenestrated the cartilage, poking several small openings into it to allow what blood it could produce to reach the surface.
“Then we stitched the graft in place and applied a bulky dressing on it,” he said. “It looked massive, but we needed to maintain firm pressure over it or else the graft would not survive.”
After three weeks, the graft was pink and healthy.
The most important take-away from the experience of being a cancer patient, Dr. Thompson said, is simple: “Do not put your health on hold.
“The second thing is that there’s an old saying—the definition of an expert is someone from out of town. That is simply not true. We have the very best cancer care in the world right here.”
Evidence links lymphomas to flawed metabolism

School of Medicine researchers have found a direct link between disrupted metabolism and a common and often fatal type of lymphoma.
“The link between metabolism and cancer has been proposed or inferred to exist for a long time, but what is more scarce is evidence for a direct connection—genetic mutations in metabolic enzymes,” said senior author Ricardo C.T. Aguiar, M.D., Ph.D. He is a professor of medicine in the Division of Hematology and Medical Oncology and a faculty scientist with the Cancer Therapy & Research Center and the South Texas Veterans Health Care System, Audie L. Murphy Division. “We have discovered a metabolic imbalance that is oncogenic or pro-cancer.”
The team, which included members of the departments of medicine and biochemistry, investigators from the UT Southwestern Medical Center at Dallas and a group of collaborators from Austria, found that the gene that codes the enzyme D2-hydroxyglutarate dehydrogenase (D2HGDH) is mutated in a subset of cancers called diffuse large B-cell lymphomas. The mutated lymphoma cell displays a deficiency of a metabolite called alpha-ketoglutarate (α-KG), which is needed in steady levels for cells to be healthy.
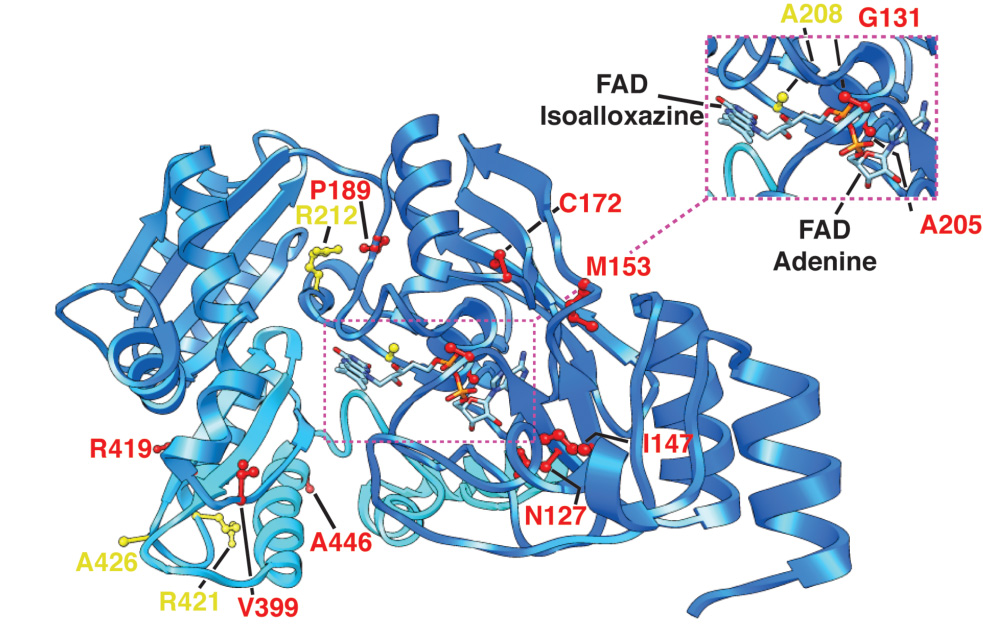 “When the levels of α-KG are abnormally low, another class of enzymes called dioxygenases don’t function properly, resulting in a host of additional disturbances,” Dr. Aguiar said.
“When the levels of α-KG are abnormally low, another class of enzymes called dioxygenases don’t function properly, resulting in a host of additional disturbances,” Dr. Aguiar said.
The metabolite has been recently identified as a critical regulator of aging and stem cell maintenance, he said.
“The implications of our findings are broad and not limited to cancer biology,” he said.
The finding was announced in Nature Communications.