What goes through the mind of a cancer doctor who learns he has cancer?

Ian M. Thompson Jr., M.D., director of the Cancer Therapy & Research Center, wasn’t as worried as was his wife, Donna, about the odd spot on his right ear.
She asked him to have it checked out; he was in no rush.
In reality, he didn’t have to go too far. Three floors down from his office in the CTRC, Sandra Osswald, M.D., oversees the Dermatology Clinic. Donna Thompson eventually convinced her husband to visit Dr. Osswald, who biopsied the spot. It wasn’t long before the cancer center director was told the news: He had cancer.
He was sent to Vineet Mishra, M.D., director of Mohs Surgery and Procedural Dermatology. Mohs is micrographic surgery that allows physicians to remove a tumor while leaving the surrounding healthy tissue unharmed. Dr. Mishra is one of nearly 1,200 fellowship-trained Mohs surgeons in the U.S.
“It was an early evolving melanoma,” Dr. Mishra said, “and it turned out to be more extensive than initially thought.”
Skin cancer is the most common type of cancer in the U.S., with more than 2 million Americans diagnosed each year. While melanoma isn’t as common, accounting for only 2 percent of all skin cancers, it is the most deadly. There will be an estimated 73,870 new cases of melanoma diagnosed this year, and nearly 10,000 people are expected to die in 2015 from the cancer, according to the American Cancer Society.
“Here in South Texas, we’re sitting in a hotbed of skin cancer,” Dr. Mishra said. “There is a misconception that skin cancer only affects certain races. In fact, it affects people of all races, all ages and both genders. It’s a major cause of concern.”
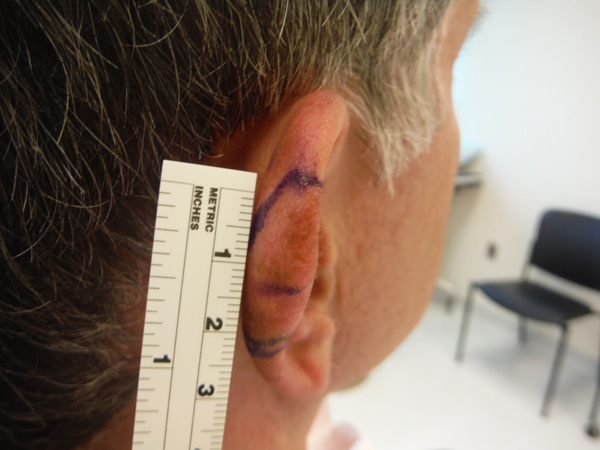
In skin cancer, a small lesion can conceal a dangerous mass with roots underneath.
Dr. Mishra compared the potential threat to that of an iceberg.
“What sank the Titanic was that which was beneath the surface,” he said.
In Dr. Thompson’s case, the lesion was especially serious because of its depth and location.
“Melanoma on the head and neck is a cause for concern,” Dr. Mishra said. “Given the routes of vascular and lymphatic drainage, it can spread to other vital structures and organs.”
“Why me?” is a question that some patients ask when faced with a frightening diagnosis, but Dr. Thompson brushed that off.
“Physicians deal with data,” said Dr. Thompson, who attended the U.S. Military Academy before earning his M.D. at Tulane University. “I can remember as a college student sitting up on the top of the gymnasium at West Point sunbathing on weekends, so there’s no ‘Why me?’ there.”
 Besides, he said, while there are clear risk factors—environmental, behavioral and genetic—a certain amount of cancer is simply bad luck. There’s no point in grappling with the past.
Besides, he said, while there are clear risk factors—environmental, behavioral and genetic—a certain amount of cancer is simply bad luck. There’s no point in grappling with the past.
The question of “What if?” is a little different.
“I spend my life with the privilege of dealing with cancer patients,” he said. “You begin to understand that what you really have is today.”
And “today” can be filled with a slew of critical decisions: What is the best treatment? Will reconstructive surgery follow?
Dr. Mishra reviewed the options with Dr. Thompson: Mohs surgery, radiation, or wide local excision. Dr. Thompson chose Mohs surgery.
With Mohs surgery, skin cancer is removed in layers. After each layer is removed, it is examined under a microscope. The process continues until healthy tissue around the cancer, or a clear margin, is reached.
“Dr. Thompson’s first layer was positive [for cancer],” Dr. Mishra said. “That’s a concern because the vast majority of patients are clear on the first layer after taking the recommended margin—which means his tumor was larger than anticipated.”
After Dr. Mishra took the second layer, the margin was clear. It was time for reconstruction surgery.
They took skin from his clavicle and sewed it on to the top of Dr. Thompson’s ear. It was challenging, Dr. Mishra said, because the cartilage has little blood supply, and a robust blood supply is needed to nourish the graft.
They fenestrated the cartilage, poking several small openings into it to allow what blood it could produce to reach the surface.
“Then we stitched the graft in place and applied a bulky dressing on it,” he said. “It looked massive, but we needed to maintain firm pressure over it or else the graft would not survive.”
After three weeks, the graft was pink and healthy.
The most important take-away from the experience of being a cancer patient, Dr. Thompson said, is simple: “Do not put your health on hold.
“The second thing is that there’s an old saying—the definition of an expert is someone from out of town. That is simply not true. We have the very best cancer care in the world right here.”
