New building for breakthrough discovery


Oct. 13 marked the dedication of the UT Health Science Center’s South Texas Research Facility (STRF), a $150 million center of discovery, scientific collaboration and translational medicine.
One of the largest and most energy-efficient research buildings ever erected in Texas, the three-story $150 million South Texas Research Facility is approximately the length of three football fields."Today we open the doors to a future of discoveries in the neurosciences, cancer and healthy aging," said William L. Henrich, M.D., MACP, president of the UT Health Science Center. "I am confident that breakthroughs will occur in this building to make lives better."
Economically, the STRF brings a sizable benefit to San Antonio. It enables the Health Science Center to begin recruiting 15 to 20 new lab teams – more than 150 new jobs. "I fully expect the STRF to become one of our city’s great economic engines as well as a source of curative discoveries," Dr. Henrich said.
For more information about the STRF, visit research.uthscsa.edu/strf.

Naming opportunities in the STRF are available.
For information call 210-567-6395.
Naked mole rat DNA sequenced
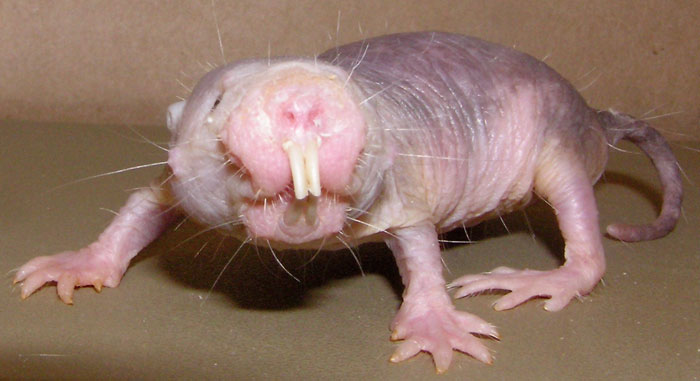
Scientists have sequenced the complete genome of the naked mole rat, a pivotal step to understanding the animal’s extraordinarily long life and good health. A colony of more than 2,000 naked mole rats at the UT Health Science Center contributed to the findings, published Oct. 12 in the journal Nature.
Arlan Richardson, Ph.D., director of the Sam and Ann Barshop Institute for Longevity and Aging Studies, said: "The data in this Nature paper are very important for aging research because they give us the first glimpse into how the naked mole rat lives 10 times longer than its distant cousins, the mouse and rat."
Rochelle Buffenstein, Ph.D., professor of physiology at the UT Health Science Center San Antonio, worked on the study with Thomas Park, Ph.D., of the University of Chicago; Vadim Gladyshev, Ph.D., of Harvard Medical School; the Beijing Genomics Institute; and other collaborators.
Vitamin E supplements increase risk of prostate cancer
 New results from a study of more than 35,000 men reveal that taking vitamin E supplements increases the risk of prostate cancer among healthy men by 17 percent.
New results from a study of more than 35,000 men reveal that taking vitamin E supplements increases the risk of prostate cancer among healthy men by 17 percent.
The results were published online Oct. 11 in the Journal of the American Medical Association. Ian M. Thompson Jr., M.D., director of the Cancer Therapy & Research Center (CTRC) at the UT Health Science Center, is one of the study’s authors.
"The impact of this study is profound," Dr. Thompson, said. "Over 200,000 men per year are diagnosed with prostate cancer. The fact that vitamin E increases this risk by almost 20 percent means there is a potential for a substantial reduction in the number of men diagnosed with prostate cancer – simply by a change in supplements."
Research that saves lives

Monumental research that makes lives better. STRF opens this fall.
A tiny wire-mesh scaffold that repairs clogged and damaged arteries near the heart. A rib made of titanium that allows children with deformed rib cages to breathe and grow normally. And a handheld port that infuses blood or medications into critically ill patients who might otherwise die waiting for traditional IV lines. All of these devices were developed by researchers at the UT Health Science Center and continue to benefit countless patients worldwide.
The UT Health Science Center has a track record of translational science success. As faculty physicians treat patients suffering from serious illnesses and trauma every day, they see, firsthand, the need for better treatments, new technology and advanced health care. Researchers and clinicians practice translational science, meaning they work together to transform lab findings into real remedies.
With the new South Texas Research Facility (STRF) scheduled to open this fall, the Health Science Center stands on the threshold of a new era in discovery and translational science. Designed by world-renowned New York City-based Rafael Viñoly Architects, the STRF is said to be the most unique building of its kind in South Texas. At three stories tall and more than 1,000 feet long, the STRF will add 190,000 gross square feet of new space to the Health Science Center campus, and will have the capacity to accommodate several hundred scientists and staff. Open lab, meeting and common areas within the building will promote teamwork and collaboration among scientists.
Lifesaving discovery
Cancer, healthy aging, neurosciences and regenerative medicine will be the focus of exploration at the STRF. Here, research will evolve into biomedical devices and therapies that university physicians, who literally work in clinics right across the street from the STRF, can use to immediately benefit patients.
With the new STRF, the Health Science Center’s tradition of excellence in translational science continues and will thrive, making lives better for generations to come.
One of the most prominent Health Science Center inventions is the Palmaz Stent®. In 1988 Julio Palmaz, M.D., a radiologist who is now the Ashbel Smith Professor at the Health Science Center, gained a patent on a tiny device he invented that would impact the world like no one had ever imagined. The Palmaz Stent, a tiny wire-mesh scaffold, is now used in 2 million patients worldwide annually to repair clogged arteries near the heart and elsewhere in the body.
This spring, the story of the stent came full circle at the Health Science ife and death for one of the university’s very own faculty luminaries.

From doctor to patient
As an associate professor in the Long School of Medicine at the UT Health Science Center and a practicing ob-gyn physician, Kristen Plastino, M.D., has delivered hundreds of babies. The University Hospital ob-gyn ward is like her second home where she spends countless hours congratulating new parents and supervising bright, enthusiastic residents who assist her in deliveries.
But on March 9 the tides turned. The doctor who is so accustomed to welcoming new life found herself in the ER, on the receiving end of treatment and fighting to elude her own death.
The day started out as any other. "Life was good," Dr. Plastino said. "Even the weather was perfect for my 10-year-old son’s baseball game that evening." When the game ended, Dr. Plastino and her son, Cole, walked to her car and began to load balls, bats and gloves. Suddenly, "My chest felt like it was being crushed," she said. Not knowing exactly what was happening, she quickly and cautiously began to drive home. Her husband, Hays, who had also attended the game, followed behind them in his car.
"Maybe it’s a panic attack," she thought to herself. But the pain pulsed violently and radiated down her left arm and up into her jaw. "By then, I suspected I was having a heart attack." The tall, thin, 41-year-old mother of four had never been hospitalized and was rarely sick. But Dr. Plastino’s instinct was right. She was experiencing a massive heart attack. "I was in shock," she said.
Clinging to life
When she arrived in the ER at University Hospital, Dr. Plastino was clinging to life. Surrounded by UT Health Science Center doctors and nurses, she was whisked away to the Cath Lab. Cardiologists determined her left anterior descending artery, the major vessel that supplies blood and oxygen to the front of the heart, had torn.
"She was literally 20 minutes away from death," said Hinan Ahmed, M.D., assistant professor of medicine/cardiology, who immediately inserted a balloon pump into her aorta to support her heart function. Then, with a balloon angioplasty, he opened up blood flow in the left anterior descending artery.
The next day, in a procedure that took less than one hour, Steven Bailey, M.D., positioned four Taxus® Paclitaxel eluting coronary stents in her artery. The devices keep the artery from tearing further, hold it open and distribute vital medication to her heart. Dr. Bailey is professor and chief of the Janey and Dolph Briscoe Division of Cardiology and the Janey Briscoe Distinguished University Chair in Cardiovascular Research at the Health Science Center.
The day after Mother’s Day, May 9, just five weeks after her ordeal, Dr. Plastino sat in her office on the fourth floor of the Long School of Medicine, courageously recalling her experience. But when she mentioned her four children, ages 3 to 10, her voice trembled and tears streamed down her cheeks. "Sometimes we think we’re in control of everything in our lives. But we’re not. Anything can happen. I thank God every day that our Health Science Center doctors were here to save me. I’m here another day for my children and my husband. Life is precious and I don’t take anything for granted."

Teamwork and technology
Dr. Plastino credits the knowledge and swift teamwork of her physicians and nurses along with the accessibility of advanced biomedical technology in San Antonio.
"I’m usually on the caregiving side of the fence," she said. "But as a patient, I witnessed, from a different perspective, a superb group of experienced and compassionate health care professionals at work. From the receptionist who answered questions in the ER, to the surgeons in the operating room, the process was seamless. I may not be alive if it weren’t for this kind of collaboration."
Dr. Plastino claims that one of the most amazing outcomes of her experience is the fact that four stents are helping to keep her alive. Stent technology was first developed at the UT Health Science Center San Antonio campus by Dr. Palmaz more than 20 years ago. "That’s the beauty of academic medicine and translational science," Dr. Plastino said. "Our doctors not only provide outstanding patient care, they accomplish the research that yields breakthroughs like the stent. These devices, these remedies save lives. I’m a living example."
Faculty physicians featured in this article, including Hinan Ahmed, M.D., Steven Bailey, M.D., Tyler Curiel, M.D., M.P.H., Francisco González-Scarano, M.D., Nicolas Musi, M.D., Kristen Plastino, M.D., Paula Shireman, M.D., and Sunil Sudarshan, M.D., practice with UT Health San Antonio, the clinical practice of the Long School of Medicine at The University of Texas Health Science Center at San Antonio. Some also serve at University Hospital and other health care partner institutions. University Hospital is a teaching hospital of the Long School of Medicine at the UT Health Science Center. For more information about UT Health San Antonio, visit UTHealthPhysicians.org.
$500,000 gift supports Anatomy Program
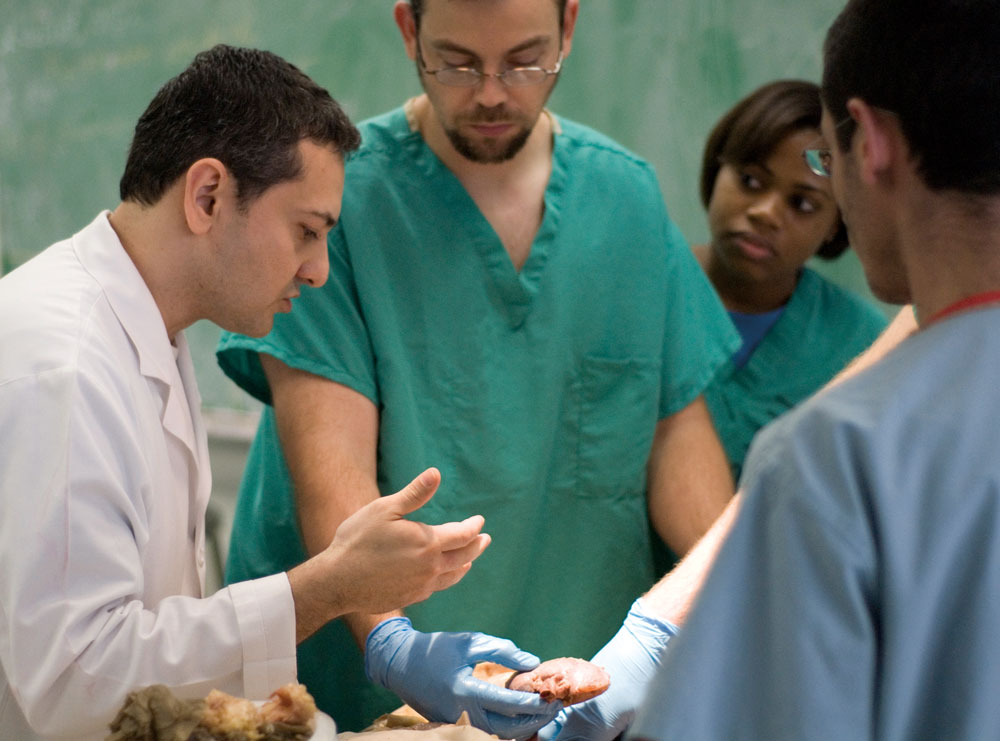
Ewing Halsell Foundation enhances Human Anatomy Program with $500,000 gift
Impacting patients and making lives better are the goals every student at the UT Health Science Center aspires to. That’s why students in all areas of study - medical, dental and health professions - begin their educational journey by meeting their very first patients in human anatomy laboratories on campus.
"Human anatomy introduces students to a different kind of patient," said Omid Rahimi, Ph.D., assistant professor in the Department of Cellular and Structural Biology, and director of the Human Anatomy Program at the Health Science Center.
"Before students work with living patients, they work with cadavers. These are the remains of once vibrant persons in the midst of life," Dr. Rahimi said. "These body donors are the preceptors for each student to confront disease, death and dying. They teach students to become skilled and compassionate health care professionals so they can care for their future patients. This is a unique experience that students can’t learn anywhere else; not from a textbook or any one model alone."
Thanks to a $500,000 gift from the Ewing Halsell Foundation, the students’ human anatomy learning experience at the Health Science Center will be enhanced by new state-of-the-art technology.
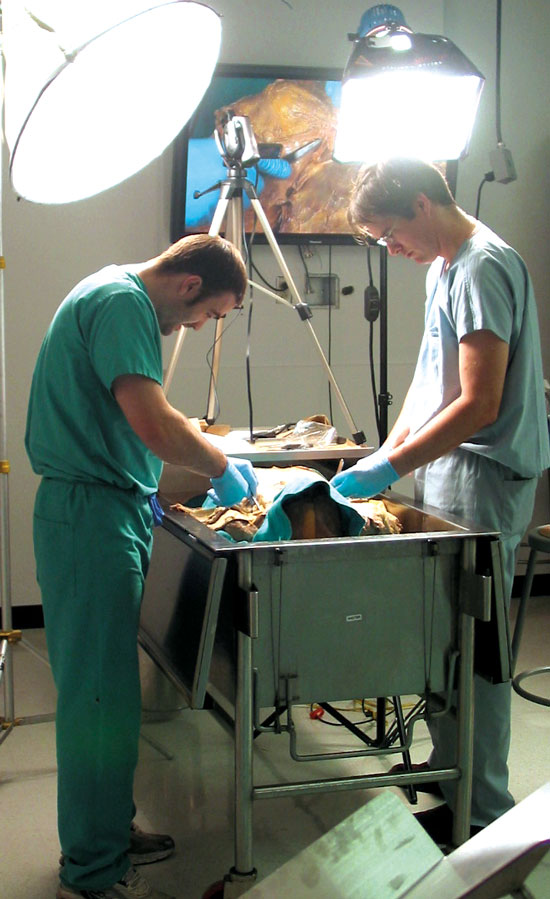
The gift is providing for 25 high-definition 58-inch plasma flat-screen monitors and ceiling-mount speakers. In addition, it also is funding a wireless microphone system, high-definition video cameras, including several hand-held models, a remote-controlled video camera mounted on a telescoping boom arm, as well as tank-side computer systems for the 57 cadaver tanks. All equipment will be networked throughout the four human anatomy laboratories located on the first floor of the Dental School. Installation of the plasma screens began this spring and is expected to be completed and ready for use by faculty and students this fall. Approximately 400 medical, dental, health professions and graduate students benefit from the Human Anatomy Program each year.
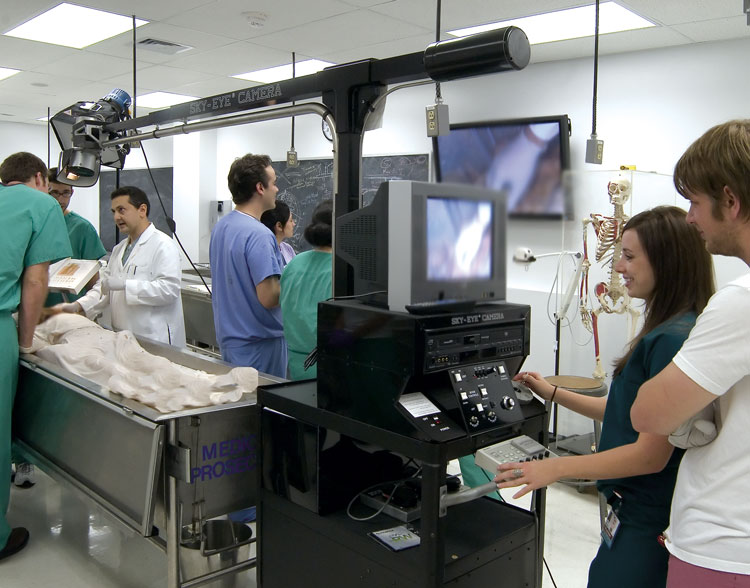
Christi A. Walter, Ph.D., professor and chair of the Department of Cellular and Structural Biology, conceived the vision a few years ago to update the labs with her colleagues, including Ron Philo, Ph.D., a retired faculty member and current adjunct associate professor who served as director of the Human Anatomy Program from 2003 to 2010.
"We are so grateful to the trustees of the Ewing Halsell Foundation for their generosity, foresight and dedicated support to the art and science of anatomy education," Dr. Walter said. "They truly understand the vast impact that anatomy education has on our students’ lives. By enhancing the students’ learning experience, their gift is helping us to better prepare students to care for thousands of patients in the future after they graduate and work in their field."
Dr. Rahimi added that in addition to improving the students’ learning experience, the new technology will also improve the anatomy faculty members’ teaching capabilities and reach.
"Today, we have a shortage of anatomy faculty," he said. "Many are retiring and the pipeline of graduate students who solely want to teach anatomy is thin. Faculty members today have to do more with less. Thanks to this gift, we will be able to help fill that void."
Dr. Rahimi explained how live dissections performed by students at one tank, for example, can be captured by video camera and broadcast to all four laboratories, classrooms or to off-campus sites simultaneously. "All of the bodies are different. So if one group of students discovers an important variation in a particular organ in one cadaver, they can share it in real time with all of their classmates and all of the laboratories," he said.
The tank-side computers will allow faculty and students to access the Internet or draw from existing human anatomy software, such as the digitized resources of head and neck vasculature and ocular movements developed by the Health Science Center’s own Frank J. Weaker, Ph.D., associate professor of cellular and structural biology.
"This new technology will allow every participant to be more engaged in academic medicine and practice and to work better together and communicate as teams," Dr. Rahimi said. "In addition to preparing the next generation of surgeons and other health care providers, I think it could reinvigorate a desire in some of our students to later teach anatomy as well."
Dr. Rahimi noted that on top of supporting students and faculty at the Health Science Center, the Ewing Halsell Foundation gift also pays tribute to the numerous individuals and families who donate their bodies or the bodies of a loved one to the university’s Human Anatomy Program.
"At the end of the day, it’s all about patients - past, present and future," Dr. Rahimi said. "The Ewing Halsell Foundation trustees have demonstrated their dedication to students and their deep respect for the silent patients who donate their bodies for the sake of science education and patients in the future. We are sincerely thankful."
Uncovering the roots of ‘at-risk’

Nearly everyone knows enough about their family’s health to fill out a patient history at the doctor’s office. Few think to go further. For those who do, taking a simple inventory of chronic conditions that crop up in a family tree can be powerful.
Take Susan Bell. The New Braunfels woman worked as a school nurse and taught nursing at the college level; yet, it never occurred to her to piece together a detailed family health history. When she finally did, she was surprised by patterns that emerged.
"It makes you sit up and take notice," said Bell, who will share this family portrait with her children and grandchildren. "I am now more aware of health issues in my extended family. That gives me an opportunity to make lifestyle changes, and I’ll be alert to symptoms."
With all eyes focused on the promise of genetic testing, the decidedly lower-tech strategy of recording which family member has what ailment is often overlooked. Yet, a thorough family health history is an effective tool that is easy to use and rarely costs more than a few minutes on the phone with far-flung relatives.
A medical anthropologist at the Long School of Medicine of The University of Texas Health Science Center at San Antonio has become an evangelist for family health histories, bringing them to the attention of people like Bell for the first time.
Nedal Arar, Ph.D., associate professor of medicine in the Division of Nephrology, began to appreciate how valuable family health histories can be – and how underused they are – while working on her own research, as well as on a study led by nephrologist Hanna Abboud, M.D. Both studies are funded by divisions of the National Institutes of Health and seek a genetic basis for diabetes and the kidney damage it causes.
As Dr. Arar spoke with patients in both studies, she was struck by how many knew diabetes clustered in their families but did not perceive themselves to be susceptible: "This underestimation of risk is very striking."
And it’s not harmless: Those who fail to recognize a threat to their health might miss chances to counteract it. An informed patient can adjust diet and exercise, quit smoking and stick to a health screening schedule.
Seeking to spread the word, Dr. Arar reached out to the South Central Texas Area Health Education Center (AHEC), which brings deep experience in community engagement. Together, they started GRACE: "Genomic-based Research Applications for Community Engagement."
The GRACE project encourages greater use of family health histories in the community. This pilot project is supported by the Institute for Integration of Medicine and Science (IIMS), which bridges research and clinical activities at the UT Health Science Center. IIMS is directed by Robert Clark, M.D., and funded through a Clinical and Translational Science Award (CTSA) from the National Institutes of Health.
The GRACE project began holding educational sessions this year – first on San Antonio’s West Side, followed by the one in New Braunfels. More are planned.
Each session begins with a video on the importance of family health histories. Afterward, participants use the "My Family Health Portrait" online tool from the U.S. Surgeon General (www.hhs.gov/familyhistory). Available in English and Spanish, the tool tracks health conditions through several generations.
"What we’ve found is that people want to be very precise," said AHEC Director Paula Winkler, M.Ed. "They will sit in front of the computer, and they’ll call their sister or their mom."
The inaugural session was hosted by the Edgewood Family Network, a nonprofit serving San Antonio’s West Side. The audience grew animated as family histories were assembled. "Once that door was open, and they started thinking about it: ‘Oh yeah, So-and-so died from this, and we’re pretty sure she had diabetes,’" said Alma Alvarado, co-founder of the organization.
Participants were encouraged to fill in blanks with relatives. "They had not, up until that point, really thought about asking," Alvarado said. "We said, ‘You should know because this affects your children.’"
Dr. Arar is measuring satisfaction with the Surgeon General’s tool and learning how people use the information. Many share it with relatives, but it’s also good to bring to a family physician.
And while family health histories are easier and cheaper than genetic testing, it’s not an either-or decision. In fact, family health histories can be used to pinpoint who would benefit most from DNA testing, saving money and eliminating unnecessary tests.
A downside to family health history information: It can be fleeting. A friend of Bell’s who attended the New Braunfels session realized that much of her family history was lost forever along with relatives who had died.
Bell had an idea for preserving it: "Maybe we should place it in the family Bible along with the family tree."
Sirinek establishes scholarship, chairs new faculty endowment campaign

"Do not follow where the path may lead. Go instead where there is no path and leave a trail."
–Ralph Waldo Emerson

Throughout the UT Health Science Center’s history, there have been many pioneers who have blazed the trail for the university’s current leaders and success. According to Kenneth R. Sirinek, M.D., Ph.D., one of the most influential of those leaders was J. Bradley Aust, M.D., Ph.D.
So in March 2010 when Dr. Sirinek was promoted to vice chairman for academic affairs and professional development in the Department of Surgery and named the J.B. Aust, M.D., Ph.D., Chair in Surgery, he promised himself he would go above and beyond to honor the memory of his late and great mentor, Dr. Aust, who passed away at the age of 83 that same year.
"I was part of the second generation of academic general surgeons recruited in 1979 by Dr. Aust to initiate and develop the research mission of the Health Science Center’s Department of Surgery, and to establish a national presence in academic surgery for this institution," Dr. Sirinek said. "Dr. Aust served as the ideal role model for young academic surgeons while creating a close-knit family atmosphere and collegiality among the faculty. He was one of the few consummate surgical academicians who excelled as a clinician, teacher, researcher and administrator."
Dr. Sirinek said he and his wife, Peggy, were well aware of the ever-increasing financial burdens placed on medical students, including a recent increase in tuition. In the past, they had supported their own undergraduate and graduate institutions. Being named to the Aust Chair served as a wake-up call to provide some financial support for the students at the Health Science Center.
In response to this, Dr. Sirinek and his wife donated $25,000 to establish the Dr. Ken and Peg Sirinek Endowed Scholarship in General Surgery at the Health Science Center. The endowment is the Department of Surgery’s first faculty-funded scholarship. Dr. Sirinek’s aim is to recognize the academic achievement of top students, encourage them to pursue a career in general surgery, and to provide them with financial relief at the same time.
"Through this endowment, I hope to keep Dr. Aust’s legacy alive and vibrant and to pass it on to the next generation of medical students, general surgery residents and my surgical colleagues," he said.
In addition to establishing this scholarship, Dr. Sirinek has agreed to a leadership role as chair of the newly organized School of Medicine Faculty Endowment Campaign. According to Francisco González-Scarano, M.D., dean of the Long School of Medicine and vice president for medical affairs, the goal of this effort will be to encourage and recruit faculty to financially support the Health Science Center and its students by establishing named scholarships in the Long School of Medicine.

J. Bradley Aust
1926 – 2010
Founding chair of the Department of Surgery
In 1965, F. Carter Pannill, M.D., who was dean of the UT Health Science Center’s School of Medicine at the time, gave J. Bradley Aust, M.D., M.S., Ph.D., a tour of a vast field, empty except for two tall silos, located on the outskirts of San Antonio. Then, he invited Dr. Aust to head a new Department of Surgery there. "The offer to help start a new medical school and develop the Department of Surgery was too good an opportunity to pass up," his colleagues said Dr. Aust later recounted. He became the founding chairman of the Department of Surgery in 1966.
For 30 years, he dedicated his time and talent to training more than 150 surgical residents and interns. "While building a highly productive department," his colleagues said, "he fostered an atmosphere of a true surgical family." He and his wife, Constance, were married for 60 years and had six children and 12 grandchildren. Dr. Aust died at the age of 83 on March 17, 2010.
For more information and to contribute to the Long School of Medicine Faculty Campaign, visit MakeLivesBetter.uthscsa.edu/medicine.
Kenneth R. Sirinek, M.D., Ph.D., is a practicing surgeon with UT Health San Antonio (UTHealthPhysicians.org), the clinical practice of the Long School of Medicine at The University of Texas Health Science Center at San Antonio.
$1 million from Audre and Bernard Rapoport supports cardiology division

This year, Dr. Lange’s efforts were buoyed by gifts totaling $1 million from Audre and Bernard Rapoport and The Bernard and Audre Rapoport Foundation. These funds will allow Dr. Lange to expand upon research and treatment programs in the Division of Cardiology over the next five years.
"I am honored and humbled by Mr. and Mrs. Rapoport’s generosity," Dr. Lange said. "Their commitment to the Health Science Center and interest in cardiology research and care will allow us to make further advancements in this area possible."
Dr. Lange is professor and executive vice chairman of the Department of Medicine, director of the Office of Educational Programs and holds the L. David Hillis, M.D., Endowed Chair in Medicine. He is a practicing physician with UT Health San Antonio, the clinical practice of the Long School of Medicine at the UT Health Science Center. Prior to joining the Health Science Center in 2008, Dr. Lange served as chief of clinical cardiology in the Department of Medicine at The Johns Hopkins Medical Institution.
Dr. Lange has published more than 200 journal articles and book chapters relating to three types of heart disease: ischemic, valvular and congenital heart disease in adults. Ischemic relates to reduced oxygen supply to the heart as a result of arteries blocked by cholesterol or plaques. Valvular relates to defects of the heart valves. Congenital heart disease results from defects of the heart’s structure and function that occur before birth.
"I am privileged to be able to serve my fellow faculty, students and patients in honor of Mr. and Mrs. Rapoport and their generosity," Dr. Lange said. "My goal is to build a world-class program that supports the vision of the Health Science Center’s mission of advancing medical research, education and clinical care through academic medicine."
Dr. Lange said he plans to use the funds to recruit accomplished new faculty and to retain senior faculty who will work together to develop novel therapies for heart disease. He also plans to invest in new state-of-the-art facilities and equipment as well as fellowship programs that will benefit outstanding junior researchers and students.
"Our Division of Cardiology is at the forefront of academic medicine through its multiple ongoing research programs, its access to the latest technology and its partnership with facilities such as University Hospital, Christus Santa Rosa Health System, and the Audie Murphy Division, South Texas Veterans Health Care System," Dr. Lange said. "These resources allow us to offer diagnostic, therapeutic and management services as well as invasive and noninvasive procedures for patients. In addition, our clinician scientists participate in the development of new cardiovascular drugs, in which our patients can benefit from through their participation in clinical trials. Because of Mr. and Mrs. Rapoport’s generosity, we will be able to expand in all of these areas."
Bernard Rapoport was born in San Antonio in 1917 to Russian, Jewish immigrants. Despite his humble upbringing, he worked his way through college during the Great Depression and graduated from The University of Texas at Austin with a degree in economics. He married Audre Newman in 1942 and began selling insurance. With a modest investment in 1951, Mr. Rapoport grew the American Income Life Insurance Company to a business worth more than $560 million.
Fueled by their desire to employ their success in promoting social justice, improving communities and helping the underserved, the Rapoports later established the Bernard and Audre Rapoport Foundation.
Since its inception in 1986, the Bernard and Audre Rapoport Foundation has dedicated more than $50 million in grants to many organizations and causes throughout the United States and Israel to cultivate emerging talents and promising models and to support education, arts and culture, health and human service, and civic participation.
In 1991 Bernard Rapoport was appointed to a six-year term on the Board of Regents of The University of Texas System where he served as chairman from 1993 to 1997.
$250,000 in gifts supports research to treat burn pain

More than 2 million people in the United States require treatment for burns each year. Thousands, including children, die or experience prolonged suffering. With more burned and injured servicemen and women returning home from the decade-long war in Afghanistan, the need for better treatments for burn pain is critical now more than ever.
Thanks to a $50,000 gift from the Elizabeth Huth Coates Charitable Foundation and a $200,000 gift from another local foundation, researchers at The University of Texas Health Science Center at San Antonio can move a step closer to developing new therapies that treat the cause of burn pain and not just its symptoms. The gifts will align top Health Science Center scientists with physicians and leaders at military partner institutions, including the Burn Center at Brooke Army Medical Center (BAMC) and the U.S. Army Institute of Surgical Research (ISR), toward this goal.
Kenneth Hargreaves, D.D.S., Ph.D., professor and chair of the Department of Endodontics in the Dental School at the Health Science Center, has led breakthrough discoveries in understanding the mechanisms of pain and how to more effectively treat it.
"Pain due to burns is a major problem since under-treatment is a risk factor for pain to become chronic," Dr. Hargreaves said. "Many available analgesics have either limited analgesia for burn pain or produce adverse side effects. "These gifts have greatly accelerated our research into the role of the endo-capsaicins in burn pain particularly in our military servicemen and women."
A substance similar to capsaicin, which gives chili peppers their heat, is generated at the site of pain in the human body. Dr. Hargreaves and his team discovered how to block these capsaicin-like molecules and created a new class of nonaddictive painkillers.
Capsaicin is an ingredient in hot chili peppers that causes pain by activating a receptor called transient potential vanilloid 1 (TRPV1). Researchers used cells from laboratory mice that were heated in a water bath at temperatures greater than 43 degrees Celsius. The degree of heat used was significant because the human body normally begins to feel discomfort and pain at 43 degrees Celsius and higher, Dr. Hargreaves noted.
"We found that in the cells heated at greater than 43 degrees Celsius, the pain neurons showed tremendous activity in the mice with TRPV1," Dr. Hargreaves said. He indicated that this novel phenomenon was taking place because the cells, in response to the heat, began to create their own natural endogenous capsaicins, which researchers later identified as a series of compounds or fatty acids called oxidized linoleic acid metabolites (OLAMs).
Linoleic acid is one of the most abundant fatty acids in the human body. Under conditions such as inflammation, low blood pressure and some other illnesses, linoleic acid is rapidly oxidized to form biologically active metabolites.
The findings have led Dr. Hargreaves’ team to develop two newclasses of analgesics using drugs that either block the synthesis of OLAMs or antibodies that inactivate them. Dr. Hargreaves noted that the drugs could eventually come in the form of a topical agent, or a pill or liquid that could be ingested, or in the form of an injection. All approaches have the potential to block pain at its source, unlike opioid narcotics that travel to the brain and affect the central nervous system.
"The data shows that these drugs inhibit pain neurons in vitro and produce analgesia in animal models of inflammation." Dr. Hargreaves said. "The question now is to determine if these new drugs are effective in treating burn pain. Thanks to these new gifts, we will be able to look at moving to the next level by collaborating with BAMC and the ISR for human clinical trials that could have immediate relevance for treating wounded warriors suffering from burn pain."
$500,000 to support Phase I clinical drug programs
An anonymous cash gift of $500,000 will help fund the lifesaving research conducted at the CTRC’s Institute for Drug Development through its Phase I clinical research program. Phase I studies offer hope for cancer patients through new investigational anticancer drugs or new combinations of novel therapies. This generous gift will support researchers who study the molecular characteristics of tumors and monitor how these relate to patients’ responses. It will also fund pharmacogenomic studies that show how genes affect a person’s response to drugs. In addition to funding a biorepository that collects tissues to facilitate studies to optimize personalized cancer therapies, this gift will provide support for novel clinical trials designed and conducted by CTRC clinicians, as well as translational studies to identify new drug targets and approaches for optimal cancer treatments.
The Cancer Therapy & Research Center (CTRC) at the UT Health Science Center San Antonio is one of the elite academic cancer centers in the country to be named a National Cancer Institute (NCI) Designated Cancer Center, and is one of only four in Texas.


