
The X-ray revealed a black void. What was once colonized by lively cells, tissue and nerves was vacant and still. The pulp tissue (nerves) inside 12-year-old Cody Nelson’s tooth was dead – the result of a biking accident. He’d been speeding down a hill when his tire hit a bump, sending the handlebars into his face.
“I touched my mouth and saw this white stuff. Then, I felt my front tooth and half of it was gone,” he said. He’d fractured his right permanent front tooth, a central incisor that assists in chewing and is one of the most visible in the mouth.
Accidents like Cody’s are common. The American Dental Association estimates that one-third of all dental injuries are related to sports or recreational activities. In addition, other sources indicate that more than 7.3 percent of U.S. children, by age 17, have lost at least one permanent tooth to decay.
Normally, a child might live with an injured or infected tooth. Even if a dentist rebuilds the missing portion of a chipped tooth, using a tooth-colored resin, the interior of the tooth’s root remains lifeless and vulnerable to infection. Root canal therapy would be the only option, but this treatment means that the root of the tooth will no longer develop, and will be at risk for further fractures for the remainder of the patient’s life.
Researchers in the Dental School at the UT Health Science Center at San Antonio are helping to solve the problem. For the first time ever in a clinical setting, researchers in the Department of Endodontics, have proven that stem cells, abundant in the soft tissue surrounding children’s teeth, can be used in an endodontic procedure to regenerate the teeth’s own tissue and cells.
Cody Nelson was one of 12 patients ages 7 to 16 who participated in the study led by Anibal Diogenes, D.D.S., M.S., Ph.D., assistant professor in the Department of Endodontics at the Health Science Center.
When a child loses a portion of tooth to a cavity, or as in Cody Nelson’s case, to an injury, inflammation and bacteria can be present. The first step in the Health Science Center study was to disinfect the tooth canal and administer antibiotics.
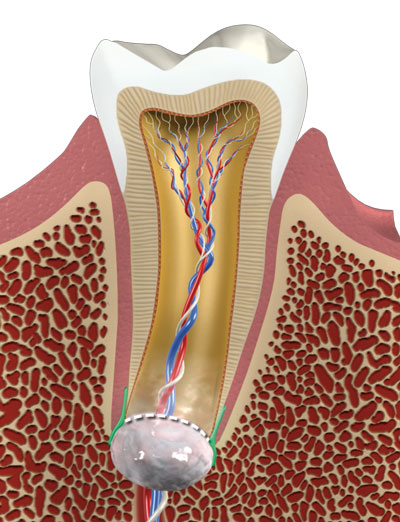
The grey-colored structure at the end of the tooth’s root is the apical papilla, which is present in developing permanent teeth and is the precursor tissue to the pulp of adult teeth. Unlike the pulp in adult teeth that may undergo necrosis due to infection, the apical papilla resists advanced infections.
Illustration by Sam Newman, Multimedia Services
Cody returned to the Dental Clinic in a month where clinician’s flushed and cleaned the tooth canal. After applying an anesthetic, dentists used a special technique to evoke bleeding in the apical papilla, which is the soft tissue surrounding the end of the root in developing permanent teeth. The apical papilla is the precursor tissue to the pulp of adult teeth. Unlike the pulp in adult teeth that may undergo necrosis due to infection, the apical papilla resists advanced infections. Thus, stem cells can be released from this structure and brought into the interior of a tooth to re-populate and restore the damaged tissue.
Standard blood samples were also drawn from each study participant.
“We needed to answer several questions,” Dr. Diogenes said. “If we caused blood cells from within the apical papilla to emerge, would they carry with them stem cells? And could those stem cells stimulate the regeneration of dead tissues in a tooth? We compared the blood samples from the teeth with the standard blood samples drawn from each patient.”
What they discovered was exciting. After one month of treatment, blood carried from the apical papilla into the tooth had a concentration of stem cells up to 700 times higher than in the systemic blood samples.
“We found that by causing bleeding in the apical papilla, we were able to release stem cells resulting in their delivery to the tooth canal. In addition, we demonstrated that the cells originated from the apical papilla and that they did not come from anywhere else in the body.”

Under high-powered magnification, stem cells (in green) can be seen among the cells (in blue) of the apical papilla and the blood vessels are seen in red. The apical papilla stem cells are capable of mediating the regeneration of tissue, and restore immune function to a necrotic tooth. Micrograph courtesy of Michael Henry, D.D.S., Ph.D., Department of Endodontics
Dr. Diogenes said the process provides the ideal environment for regeneration or restoring vitality to the tooth pulp. “All of the elements of bioengineering are present,” he said. “Bleeding is provoked, which brings the stem cells into the tooth canal. The blood clots, naturally forming a fibrin scaffold (a network of proteins that preserve living tissue). Platelets and the tooth structures provide the growth factors needed. Finally, the stem cells stimulate the regeneration of tissues, which are then supported by the scaffold and the growth factors.”
What was once dead tissue is brought back to life. More importantly, Dr. Diogenes said the tooth is immunocompetent, meaning it can defend itself from infection.
“The further development seen means a stronger reliable tooth that functions as an uninjured tooth,” Dr. Diogenes said. “The process takes several months, but positive vital responses have been seen in as little as six months.”
The study was funded by the American Association of Endodontists Foundation and by the Department of Endodontics at the UT Health Science Center and was published in the Journal of Endodontists. The American Dental Association is creating treatment codes for this new procedure that Dr. Diogenes hopes will become widely used in dental clinics across the country.
Co-investigators on the study from the Department of Endodontics at the Health Science Center were Kenneth Hargreaves, D.D.S., Ph.D., Michael Henry, D.D.S., Ph.D., and Tyler Lovelace, D.D.S.
Dr. Diogenes and his team are now studying the same process in adult patients.
“We are excited about these findings because not every child is a candidate for a root canal,” he said. “If an affected tooth is not fully formed, further development is not viable after conventional root canal therapy. During a root canal, dentists fill a tooth with an inert material. Therefore, the tooth can no longer develop,” Dr. Diogenes said. “Only regenerative endodontics can restore vitality in the tooth. Instead of having to live with tooth loss and limited therapy options, we may now be able to offer this minimally invasive procedure, which costs about one-quarter of root canal surgery.”
Kenneth Hargreaves, D.D.S., Ph.D., professor and chair of the Department of Endodontics at the Health Science Center, said Dr. Diogenes’ research represents translational science at its best.
“Anibal and his team are the first to demonstrate a clinical procedure that delivers a high concentration of mesenchymal stem cells into the root canals of disinfected teeth that literally regenerate tissue in actual patients.” Dr. Hargreaves said. “These findings provide a foundation that will be incredibly important in guiding the translation of tissue engineering from the bench to the chair side. He and his team are among the leaders in this effort.”
Laura Nelson, mother of study participant, Cody Nelson, said she was glad her son was among the first to benefit from this procedure.
“It’s amazing what the dentists at the Health Science Center’s Dental Clinic can do,” Mrs. Nelson said. “We are lucky this research and these specialists are here in San Antonio. Cody can chew gum and eat apples just like before. He recently got braces too.”
Cody said he thinks it’s “pretty cool,” especially since he’s back to being an active 12-year-old and doing what he loves to do best – riding his bike.
To become a patient in the UT Health Science Center Dental Clinic, call
210-567-3217 or visit www.dentalscreening.com.
