The health care equity equation

The university’s Wellness 360 patient care practice balances a self-sustaining clinical enterprise with expanded health care access for all
By Norma Rabago
In 2017, newly hired Cindy Sickora, DNP, RN, FAAN, UT Health San Antonio School of Nursing vice dean of practice and engagement, was tasked with converting a system of four clinics offering free care to a self sustaining clinic model while providing the same high level of care. Through months of analysis, Sickora discovered untapped sources of income but also a way to expand the clinic’s reach to low-income communities in need of quality health care.
“I worked with a consultant, and I told her I don’t know how to make a lot of money, but I do know how to be socially just,” she said.
Hard work and happenstance
The road to self-sustainability for Wellness 360, the patient care practice within the School of Nursing, has required hard work and happenstance. First, Sickora and her staff had to learn how to bill students and faculty for care.
A request to provide disaster relief in the wake of Hurricane Harvey in August 2017 led to a previously unplanned purchase of a mobile health unit.
Then, a call from Karen Schwab, PhD, APRN, CPNPPC, PMHS, asking for space to care for pediatric patients, led to an unexpected expansion of service.
“I was finishing my PhD at the nursing school and working at a private practice, but it was winding down, so I had to think long term,” Schwab said. “I had this panel of patients who were second generation; my patients were now having their own children. I knew Dr. Sickora might be open to pediatrics after hours, so I asked her, and she gave the green light.”
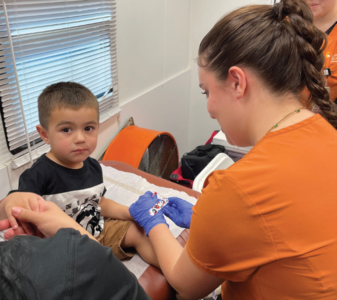
Schwab now serves as Wellness 360’s director of pediatric services. She said that, on average, the clinic sees 20 to 30 pediatric patients daily and recently saw an all-time high of 52 patients in one day. Those numbers will climb with the rollout of patient care hubs in the works, which are connected to a $4 million grant Schwab received last year to provide care to foster care children across 28 Texas counties.
More broadly, through partnerships with nonprofit organizations such as AVANCE, SJRC Texas and Respite Care of San Antonio, nurses provide well- and sick-child visits, preventative screenings, behavioral health services and telehealth for children living in underserved communities, foster care children and children with special needs. Nurses use the mobile health unit to travel to rural communities such as Uvalde, providing the same care.
“It’s critical to see the adversity that people face in accessing health care. When you get students in the community, they see the difficulty of accessing care, and it changes how they look at people,” Sickora said.
“It’s one thing to see someone in a hospital bed where you have control. It’s not the world of the patient; it’s your world as the provider. When you go out and see what people face, you have a whole different world view of why people are where they are.”
Student immersion
A major benefit of the clinic program is the real-world experience it provides for nursing students, especially in giving them exposure to caring for vulnerable populations.
That’s been true for Karina Herrera, a seventh-semester nursing student at UT Health San Antonio. Herrera’s interest in providing care for children started when she was a volunteer at the Dell Children’s Medical Center in Austin while pursuing her undergraduate degree in biology.
“When you think of hospitals, they have very plain white walls. The LED lighting is not very welcoming,” Herrera said. “I started volunteering at the children’s hospital, which was more colorful and optimistic. I liked that environment and fell in love with pediatrics.”
Today Herrera volunteers at the Wellness 360 pediatric clinic as part of the award-winning Pediatric Volunteer Team, a nursing student-led organization for students interested in treating children. Herrera is the incoming president. Through the school’s mobile health unit, Herrera and her fellow volunteers bring health care to underserved communities — communities that she knows well.
“I know what it’s like to have few clinics or providers available near you and wait a long time to see a physician,” she said. A Del Rio, Texas, native, Herrera remembers making the day-long trip to San Antonio with her mother and grandparents to see specialty doctors. She said bringing health care to patients in rural communities rather than requiring them to travel to San Antonio has been especially rewarding.
Campus expansion
For Sickora, both the expansion into rural communities such as Uvalde and growing care networks with new technologies such as telehealth will further add to the clinic’s success.
In 2020, The University of Texas at San Antonio and the Alamo Colleges District established partnerships with the UT Health San Antonio’s School of Nursing to manage and staff clinics on their campuses, initially through telehealth and now also in person. These clinics opened in 2021, offering medical care ranging from minor illnesses to behavioral health.
In addition to treating students, services are available to staff and faculty. Students without health insurance pay $5 per visit.
“Regardless of ability to pay, we don’t send anyone away,” said Maria Saldiva, DNP, APRN, FNP-C, a family nurse practitioner.
As the clinic enjoys financial stability, and with an eye toward leveling the playing field of quality health care for all, the future of Wellness 360 looks bright, according to Sickora.
“I’m the ultimate optimist, and I think there is nothing we can’t do,” she said. “I think as long as we have the right people — which we absolutely do have the right people — we can do anything.”
Wellness 360 goes to school
Deaunte Watkins, a San Antonio College student, wasn’t feeling well.
“I was having trouble with my chest, and I wasn’t sleeping well,” he said. “At the time, I was unsure what to do.”
 Through a friend, Watkins heard about the campus Wellness 360 clinic’s affordable services for students through a partnership between the Alamo Colleges District and UT Health San Antonio’s School of Nursing to manage and staff clinics on campuses.
Through a friend, Watkins heard about the campus Wellness 360 clinic’s affordable services for students through a partnership between the Alamo Colleges District and UT Health San Antonio’s School of Nursing to manage and staff clinics on campuses.
After an appointment with Maria Saldiva, DNP, APRN, FNP-C, a family nurse practitioner, Watkins was diagnosed with high blood pressure.
“She was so welcoming. The whole staff made me feel comfortable,” he said.
On average, 10 to 15 patients are seen daily at San Antonio College, said Saldiva. Aliments range from respiratory infections to basic behavioral health services. A psychiatric nurse practitioner is available for students requiring additional behavioral health services in the Alamo Colleges District schools.
After Watkins’ diagnosis, Saldiva worked with him to implement a plan that included medication, exercise and healthier eating habits.
“I’ve lost more than 50 pounds,” said Watkins. “I’m happy and living a good life.”
Mobile health unit delivers vital services and experience
What do Paul Simon, Edie Brickell and the UT Health San Antonio mobile health unit have in common? Answer: $200,000.
After Hurricane Harvey decimated such coastal cities as Rockport, the Grammy-winning duo donated funds to UT Health San Antonio School of Nursing’s Cindy Sickora, DNP, RN, FAAN, vice dean of practice and engagement, to provide medical services to Rockport’s residents.
A veteran of disaster relief efforts, Sickora mobilized the school’s faculty and students to travel to the coastal city. Some of the donated funds were used to rent a fully equipped mobile health unit. With the remaining funds and additional dollars from the school, Sickora purchased the mobile unit to bring medical services to the San Antonio community and function as a teaching site for nursing students.
But to sustain the unit, Sickora needed a financial backer. In a meeting with health insurer Superior Health, Sickora pitched the idea of sponsorship to the company’s executives but felt it wasn’t going well.
“The executives were sitting in the meeting on their phones. [It appeared] they weren’t paying attention to us,” she said. “Low and behold, they were texting each other saying ‘$50,000? Let’s put our name on it.’”
With the annual sponsorship and sporting the Superior Health logo, the burnt-orange mobile health unit is driven across the city, providing services such as mandated physicals for high school students and well-child exams and vaccinations for disadvantaged children. Jane Smith, RN, mobile health coordinator and occupational health nurse, said the visits with families were particularly joyful.
“You are part of the solution in ensuring people have what they need to thrive,” she said.
Later, during the pandemic, Sickora leaned on her disaster response experience and included the unit in her strategy of providing COVID-19 tests and vaccines across the city. The unit was especially useful at job sites where workers lacked the time to stop by a clinic.
“It was minimal disruption for the jobsite. It was minimal disruption for the employees. But they were all vaccinated,” Smith said.
Smith said the future of the mobile unit includes expanding services to neighborhoods across the county with limited medical care and rural communities facing the same struggle. Along with helping to fill the medical care gap, the mobile health unit’s teaching component is equally invaluable to future RNs.
“By the time the students graduate, they are more confident in their abilities. When I graduated from nursing school, I had only given three shots, whereas our students have given close to a hundred,” Smith said.






