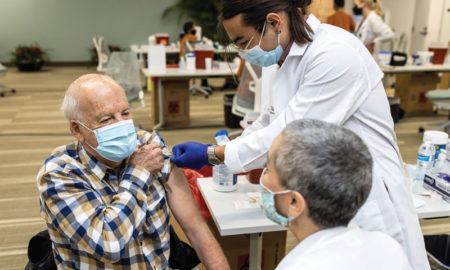
ICU Nurse Finds Career Later in Life as Pandemic Strikes

By Salwa Choucair
Just a month into her first job as a nurse in the Medical-Surgical Intensive Care Unit of Methodist Hospital, Brenda Backlund-Pearson, BSN Class of 2019, RN, began questioning her new career path which she had just spent two years studying to achieve and two decades finding.
At 47, Backlund-Pearson found herself starting her third career during the beginning of the COVID-19 pandemic.
“I wondered if I should quit and start over once the pandemic is over,” she says. “I am older, and my parents are older. All these thoughts were going through my mind. I was terrified. I thought, I don’t even know what I’m doing, and now the world is battling a new deadly virus.”
Instead of quitting, she worked three days a week, arriving early, staying late and spending her off time gardening and re-reading lessons from her School of Nursing professors at UT Health San Antonio to find out what she could about the new disease affecting her most critical patients.
With a strong desire to help people and make a difference in their lives, Backlund-Pearson turned to nursing as a career after studying cosmetology, journalism and education and after working in retail for years. She has always been able to read people and recognize when they need help. She chose ICU nursing because she noticed that ICU nurses seemed to use their intuition when it came to their patients, and her natural ability to assess people and situations would serve her well.
“Today, making a connection with a patient or the patient’s family, that human interaction, is my favorite part of the job,” she says.
Making that connection was more important than ever when COVID-19 patients took over the ICU.
“Unfortunately, in the ICU, we were watching the sickest of the sick slowly fade,” she says, “Not everyone passed away, but it was a much higher mortality rate. It was devastating as a new nurse to think I was just watching people die.”
Her manager wanted her to know that she was making a difference and suggested she begin following her patients when they were discharged from the ICU to another unit.
She continued to make that human connection as well, noticing when one of her patients was ready to give up, pulling up a chair next to her and holding her hand. She asked the patient’s daughter to cover a poster with photos of family members and proceeded to go over each picture with her patient. The patient’s spirits improved, and she told the patient, “Look at all these people who love you and care about you. You’ve got to fight for them. I know this is hard, and you want to give up, but you can’t give up.”
“Those are the moments when I feel like I made a difference,” says Backlund-Pearson, who followed that patient’s progress until she was discharged from the hospital. “That’s what I choose to focus on, because that one patient was one of 10, and nine didn’t make it.”
Since visitors are not allowed in the ICU COVID unit, Backlund-Pearson and her colleagues are the only contact patients and their families have with one another.
At the end of their lives, patients and their families rely on her to facilitate their goodbyes. Protected in personal protective equipment from head to toe and wearing a mask, she holds up an iPad so that loved ones can see each other one more time.
“I tell them that I am holding their loved one’s hand, and although I have tears myself, I hide them, because this isn’t about me. This is about them. You can hear the sadness and the mourning, but it is more sad because it is disconnected. Technology is amazing, but it is not the same as a physical hug or a physical touch, and I am thankful for my fellow nurses when I leave that situation. Sometimes it is a hand on the shoulder from another nurse, and other times it is an outright sob. Just three minutes and it is time to suck it up, get it together and go to the next patient.”
She does not know how many patients she has watched die from COVID-19.
“More than I can count,” she says, “and it changes you.”
Backlund-Pearson continues, however, to make that human connection with her patients, and while it took her some time to get here, she knows that with nursing, she has finally found her calling in life.
“I wish I had done this sooner, but I truly believe that 20 years from now, I can still be doing something impactful and beneficial even at 67. Nursing allows me to do that, and there will always be something rewarding in this field. The options are amazing.”