COVID-19 Grants Allow Nurse Researchers to Improve Care, Educate

By DAVID ENDERS
Vaccine researchers, drug developers, and epidemiologists have made well-deserved headlines this past year for critical research in fighting a global pandemic. But who is best positioned to do the equally important research into the actual lived experiences of COVID-19 clinicians, patients, their families and communities? For that, you are going to need a nurse researcher.
UT Health San Antonio School of Nursing researchers received several COVID-19 supplemental research grants to find better ways to deliver care.
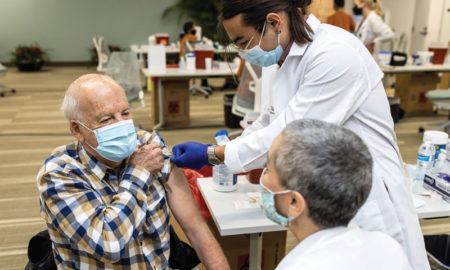
Professor Norma Martinez Rogers, PhD, RN, FAAN, was awarded $95,455 from the Health Resources & Services Administration (HRSA) to educate the community on COVID-19. The grant covered production of a bilingual video series designed to fill the gaps in COVID education for at-risk populations. Titles include: “The Advantages of Telehealth” (Lisa Alberts, DNP, APRN-BC, PMHNP-BC); “Advanced Care Planning: Why it Matters in the Days of COVID-19” (Kristen Overbaugh, PhD, RN); “Sleep Disorders of the Elderly Related to COVID-19” (Kylie Meyer, PhD); and “The Importance of Getting the Vaccine” (Amanda Villareal, PhD). The grant also provided for laptops to be used for telehealth at the Wellness 360 clinic and mobile unit, as well as relaxation headsets for stress relief, pulse oximeters, thermometers, remote blood pressure cuffs, and stethoscopes.
“The focus of this grant was not only to prevent COVID, but to make our senior citizens aware of the dangers,” Dr. Martinez Rogers says. “The Importance of Getting the Vaccine” is targeted at underserved populations more apt to view public health with a level of mistrust. “We specifically chose Dr. Villareal for that video because we wanted somebody not in the health care profession to ask them the question, ‘What do you need to hear about why you should take this vaccine?’ Dr. Villarreal has attended the grassroots churches in these areas and knows the population very well.”
The vaccine has become so politicized, she says. “One of the biggest challenges we faced was accessing the churches and trying to get them to accept that what we were saying needs to happen without it being a sermon.” Her team plans to distribute the videos through YouTube, partnering with health care systems, and the School of Nursing’s Wellness 360 mobile unit to reach rural communities.
The pandemic has laid bare health care disparities. “Telehealth is great if you have a laptop and internet service, but not so great if you don’t,” Dr. Martinez Rogers says. “And the people who are really poor don’t, and that’s when it becomes a problem. So there has to be other mechanisms we can use to reach the underserved. When you are wondering how to feed your kids their next meal, problems like COVID become a lower priority.”

Reaching at-risk communities often falls on the shoulders of the Community Health Worker (CHW). Janna Lesser, Phd, RN, FAAN, director of the South Texas Area Health Education Center (AHEC) Program, and her team used a $91,802 supplemental COVID-19 grant from HRSA to expand grassroots research projects in underserved communities. Using the Project ECHO model, they developed a new curriculum for CHWs. “We had the privilege of getting to do the groundwork in understanding what the CHW is doing and what makes sense for them in their communities,” says Dr. Lesser, professor and holder of The Anita Thigpen Perry Endowment for the Center for Community Based Health Promotion with Women and Children. “We’re kind of proud of that because it uses a community-based participatory action research model.”
Project ECHO employs telemedicine to assist rural providers using two-way engagement with specialists to help them manage care for complex patients. The new curriculum includes domains on COVID testing, vaccines, signs and symptoms, behavioral health, mental health, health disparities, and self-care—all highlighting the strengths in each community to help them take care of each other. “We also want to see how this COVID-19 Project ECHO impacts the mental health of CHWs in the field,” says Pamela Recto, PhD, RN, assistant professor.
A grant from the Institute for Integration of Medicine & Science, in partnership with the San Antonio Fatherhood Campaign, also allowed Dr. Recto to investigate the impact of the pandemic on young fathers. “Some of these young fathers are the primary providers for their family and the stress of not having a job or having their hours cut, along with the fear of getting COVID and bringing it home to their families, is a big problem,” she says.
 Jing Wang, PhD, MPH, RN, FAAN, vice dean for research Jing Wang, PhD, MPH, RN, FAAN, vice dean for research |
 Janna Lesser, PhD, RN, FAAN, director of South Texas AHEC Janna Lesser, PhD, RN, FAAN, director of South Texas AHEC |
 Pamela Recto, PhD, RN, assistant professor Pamela Recto, PhD, RN, assistant professor |
 Joe Zapata , Jr ., MSS, manager of Academic Programs for South Texas AHEC Joe Zapata , Jr ., MSS, manager of Academic Programs for South Texas AHEC |
Unfortunately, some people under extreme pressure will turn to opioids, and Joe Zapata, Jr., MSS, manager of Academic Programs for South Texas AHEC, conducted a qualitative study to explore the impact of South Texas AHEC’s Project ECHO Opioid Use Disorder Project for CHWs on the participating health workers. He also explored the impact of the pandemic on these CHWs practicing in South Texas communities. “The experience impacted me as well because I am in the process of becoming a CHW,” added Zapata.
Andrea Moreno-Vasquez, MPH, senior program coordinator for South Texas AHEC, completed a qualitative study to better understand the experience of life during the pandemic amongst women living on the westside of San Antonio. The predominance of participants were domestic workers. “These women all feel closed off, isolated, and they feel that domestic work is not really valued in this country, that it doesn’t deserve good pay, benefits, or formal work contracts,” says Moreno-Vasquez. Many were terminated immediately when the pandemic hit with no formal work contract or social safety net.
Families impacted by dementia already experience isolation and this has been exacerbated during the pandemic. Professor Carole White, PhD, RN, FAAN, director of the Caring for the Caregiver program, received a $102,805 supplemental COVID-19 grant from the Patient Centered Outcomes Research Institute (PCORI) to continue the development of the Stakeholder Alliance for Better Palliative Care for People with Dementia and their Caregivers, with an expanded focus on COVID-19 and dementia care. Some 16.1 million unpaid caregivers (mostly family members) in the U.S. take on the responsibility of caring for loved ones with dementia, and the pandemic has added to their stress.
Dr. White collaborated with an advisory council consisting of people living with dementia, family caregivers, and health and social care professionals to provide a sustainable and supportive community to share resources as well as set an agenda for the research that matters most to them.
“The hope is if we listen to the voices of stakeholders, we actually study what matters to them.” The results of a survey conducted with stakeholders identified the need for more support at the time of diagnosis. “Although we have effective interventions to support families,” Dr. White says, “these interventions are available to less than 3 percent of families. There is a pressing need to ensure that effective interventions are available in the community to support families impacted by dementia.
In discussing research priorities, the advisory council identified the need to look at how COVID-19 has affected dementia care. “I think what we’re doing in looking at the impact of COVID-19 on dementia care from multiple perspectives will provide a more complete picture of how COVID-19 has impacted dementia care,” Dr. White says.
The results of surveys conducted with 124 family caregivers indicate that over 60 percent report feeling isolated since the pandemic, and they report high levels of fear and anxiety related to the care of their family members with dementia, particularly if their family member is in an institution. Almost half of family caregivers state that their quality of life has decreased since COVID-19. Themes from focus groups conducted with family caregivers highlight their challenges to provide care and deal with losses during COVID-19.
“Family caregivers described how COVID-19 has forced them to think about having a ‘Plan B’ in place, ensuring that they have plans for their family member if something happened to them. Despite the struggles for families impacted by dementia during COVID-19, family caregivers have also been able to identify strategies that have helped them to cope, including technology innovations that have allowed them to continue to join support groups and also interact with family members,” she added.
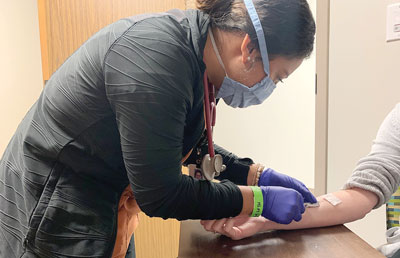
Telehealth has played a key role during pandemic lockdowns, but how do you make it better and more accessible to vulnerable populations? That was the focus of a $25,000 COVID Response Fund grant from the San Antonio Area Foundation, partnering with United Way. Jing Wang, PhD, MPH, RN, FAAN, vice dean for research, used the grant to provide free wearable and remote health monitoring devices (including pulse oximeters, fitness trackers, blood pressure monitors, glucose meters, and guided meditation headbands for stress) to 128 diagnosed COVID-19 patients as well as vulnerable seniors, people with chronic conditions, and their caregivers.
Dr. Wang, director of the Center on Smart and Connected Healthcare Technologies, says the center’s Connected Health Platform enables patients to connect directly to their clinicians to share meaningful device data.
“I think the demand for this is very large,” says Dr. Wang, holder of the Hugh Roy Cullen Professorship in Nursing. “We had a lot of people sign up in a very short period of time without much advertising. I definitely see a need to scale this larger. The beautiful part is we have already developed a system that can help the patient integrate all of these devices into one platform so they don’t have to use several apps to see their information, and they choose who they want to share it with.” One COVID patient remarked, “The blood pressure monitor helped a lot. My doctor wanted me to provide her updates, and now I can use the pulse oximeter daily to do that.”
Perhaps one silver lining to the pandemic, Dr. Wang says, is that people may be more willing to adopt smart and connected health technologies for easy access to care and enhanced quality of care.
“When you consider patient-generated information from home gives both the patient and the clinician a better picture of patient behaviors and needs, that is really the key for patient-centered care.” At the same time, she adds, there is no substitute for the hands-on approach. “The core of nursing is always the supportive care we provide to our patients. Technology is just a tool that nurses should learn and harness to provide the best possible and needed care to the underserved.”