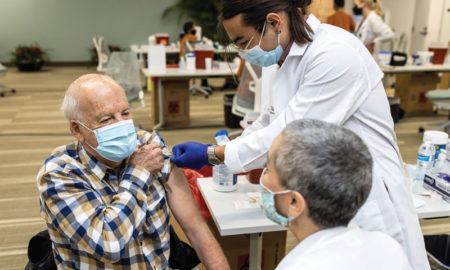
Caring for the Caregiver: Support, Resources Transition to Virtual Platform

By GINGER HALL CARNES
The COVID-19 pandemic intensified the isolation that typifies the stressful life of a caregiver for a person living with dementia. Responding to caregiver needs has produced unanticipated “silver linings” for caregivers and brought national attention to UT Health San Antonio’s Caring for the Caregiver program.
Established in 2016 by a team from the School of Nursing led by Carole White, PhD, RN, FAAN, founding director and the Nancy Smith Hurd Chair in Geriatric Nursing and Aging Studies, the robust Caring for the Caregiver program began by offering in-person activities to bring caregivers and persons living with dementia out of their homes. Since 2017, nearly 1,700 community members have attended at least one event with most attending multiple events over time.
When the pandemic hit in March 2020, a Skills Training Workshop that was a monthly five-hour event to teach practical caregiving skills ceased. Memory Cafés, events where caregivers and people living with dementia socialized and could be creative, also ceased. In-person engagement with caregivers ceased.
The program’s team quickly adjusted to create ways to reach caregivers and expand their programs to a virtual environment.
Sara Masoud, MPH, the program’s community outreach coordinator, said team members immediately began calling everyone in their database to find out how they were coping with the pandemic and determine what to do as a program, which resulted in the creation of the Caregiver Reassurance Program. Now 15 to 20 UT Health San Antonio nursing and occupational therapy students volunteer for six months to call caregivers. These students receive ongoing training and are certified as “Dementia Friends.” Every student is paired with a list of family caregivers who they call at least once a month over a six-month period. “They are the sunshine in someone’s day to focus on the positive, find out how they’re doing and what they’re looking forward to, and to refer them to resources they might need,” Masoud explained.
“It’s our dream to create a Care Navigation Program” because the program is mutually beneficial, Masoud said. Students learn as care professionals and the caregivers feel they have someone who will listen to their challenges and provide help.
They found other silver linings—including sharing their programs with others around the world—that would not have happened without Zoom. A Memory Café where caregivers and people living with dementia played Lotería (which is sometimes referred to as “Mexican bingo”) attracted 70 households from across the United States. They now partner with UT Rio Grande Valley to offer their Memory Café events in a bilingual format.
Dr. White and Masoud organized a symposium in March 2021 focused on the impact of COVID-19 on dementia care, funded by the national Patient-Centered Outcomes Research Institute (PCORI). Rather than spending funds to travel to San Antonio for the national conference, more than 200 people attended virtually.
During a national Zoom presentation to Dementia Friendly America, Education Specialist Jennifer Brackett, MS, shared best practices the UT Health Caring for the Caregiver program created as it migrated to virtual communication.
The change is prompting people to engage with each other virtually, not just listen to someone lecture on a screen. Memory Cafés, started in the 1990s in the Netherlands, lean toward creative activities involving music, dancing, games and the arts; new people can join anytime. The effort has prompted the local Alzheimer’s Association and senior living facilities to start cafés.
Kylie Meyer, PhD, a postdoctoral research fellow who joined the nursing faculty in June 2021, said people from across the country are “Googling” for support and landing on their website. Virtual programs allow caregivers across the country to attend UT Health social and education programs. “It creates a broad community nationally,” she said.
Brackett chairs the Dementia Friendly San Antonio (DFSA) Council. Begun pre-COVID with 250 at a Town Hall, citizens identified specific topics the city needed to address with first responders, universities, and other health care professionals on how to interact with persons living with dementia.
“The council is working to build an inclusive community where everyone touched by dementia is respected, engaged, and supported. DFSA is a communitywide grassroots initiative led by a community advisory board which has come together to address the pressing need for an inclusive community that supports families touched by dementia,” Brackett explained.
For example, when the person with dementia is present, they advise not asking the caregiver how the person is doing but speaking directly to the individual living with dementia to promote a culture of inclusivity. “We have a person with dementia on our Dementia Friendly Advisory Council because we need to hear both sides and be informed,” Brackett said.
The five-hour Skills Training Workshop transitioned into four shorter Learning Skills Together sessions via Zoom.
Dr. Meyer learned through satisfaction surveys that Zoom-delivered skills training is preferred by many families because they do not have to schedule someone else to keep an eye on their care partner. “Having it online provided a greater degree of flexibility so more people could attend,” she said.
The Caring for the Caregiver team also relayed caregivers’ concerns about leaving the house to see doctors or their grandchildren during the COVID-19 pandemic. Many caregivers lost support during the pandemic because no one was coming to homes and respite places closed.
Brackett provides educational support through the Essentials of Caregiving program with panel discussions on such crucial topics as understanding a diagnosis of dementia, learning to be a caregiver, and planning for future care. She also creates a monthly newsletter, which was weekly during the first eight months of the pandemic, that is available on the website.
The program’s Stakeholder Advisory Council has received additional funding from PCORI to explore how COVID-19 has impacted dementia care. This council has conducted focus groups and interviews with the caregivers, people living with dementia, and health and social work professionals to hear their perspectives on this topic.
The team keeps its robust website up to date at www.utcaregivers.org where they share tips to help get connected with others and registration links to their virtual programs. Caregivers can sign up for the newsletter and access a multitude of resources from internal and external sources. They have tips on how to relieve the feelings of isolation that plague caregivers, even without COVID restrictions.
Dr. Meyer noted that some family members solely consider themselves the “spouse” or “daughter” rather than calling themselves “caregivers.” “The term ‘caregiver’ is a key to open the door to resources,” she said. “We want to help all caregivers who are dedicating their lives to helping people living with dementia.”
All UT Health San Antonio Caring for the Caregiver services are free to family caregivers and are supported through donations and grant funding.

Glenn Biggs Institute for Alzheimer’s & Neurodegenerative Diseases
210-450-9960 • https://biggsinstitute.org
Provides a comprehensive network of clinical care for patients and their families with access to the most advanced treatments and clinical trials.
Alzheimer’s Association
1-800-272-3900 • www.alz.org/sanantonio
Provides a 24-hour helpline where you can speak with an expert.
Caregiver SOS (WellMed Charitable Foundation)
1-866-390-6491 • www.caregiversos.org
Provides education, information and support to family members and friends providing care to an older person.
National Alliance for Caregiving
https://www.caregiving.org
Provides additional resources to help family caregivers address and cope with the challenges of caring for a loved one.
National Institute on Aging
https://www.nia.nih.gov/health/caregiving