50 Years of Medicine: An Overview of the Past, Future

Reminiscing on School’s Creation While Looking to Dynamic Future
By Ginger Hall Carnes

As UT Health San Antonio’s Joe R. and Teresa Lozano Long School of Medicine celebrates its Golden Anniversary, some of the early faculty and students point to changes and successes that weren’t even imaginable when the doors opened in 1968.
When The University of Texas Medical School at San Antonio opened its doors to students on Sept. 3, 1968, “there was great excitement and enthusiasm,” recalled Marvin Forland, M.D., who was among the first faculty members and still works on campus today at the age of 85. Some students began their classes at UT Southwestern Medical School in Dallas or the UT Medical Branch at Galveston, seven transferred from outside the UT System, and others were first-year students, bringing the total enrollment to 105.
James L. Holly, M.D., who was in the 1973 graduating class, remembers cows grazing on the property. As Fred Olin, D.V.M., M.D., a San Antonio orthopaedic surgeon who also graduated in 1973, drives by campus today, he is “astounded at how much they covered up the land.” Dr. Olin remembers meeting on the first day of class in an auditorium, now named for his classmate, Dr. Holly.

Linda Johnson, Ph.D., gets goose bumps on her way into work when she comes over a hill on Floyd Curl Drive. A panorama of medical buildings comes into view. She compares it to “the dawning of creation. You can see the Medical Arts & Research Center, the Center for Oral Health Care & Research, the Mays Cancer Center, and many other medical buildings.”
The early days
When she started at the medical school as a lab associate in 1972, all of this was vacant land; she remembers just three buildings—the 440,000-square-foot UT Medical School at San Antonio, Bexar County Hospital (now University Hospital) which opened Nov. 9, 1968, and Methodist Hospital. “I would drive in to do experiments at night, and there would be deer on the lawn.”
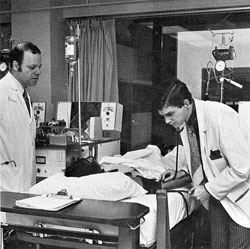
Dr. Forland credits the school’s second dean, F. Carter Pannill, M.D., with “siring a medical school” by planning the laboratories, overseeing the completion of the new structure, hiring department chairs, and making efforts to move into the community. During his tenure from 1965 until 1972, “Dr. Pannill was the person most influential in launching us,” Dr. Forland said.
Dr. Holly lauded the early faculty, describing Dr. Pannill as “a visionary of what this school could become.” He particularly named Drs. Pannill, Forland, Elliott Wesser and Jim Story. “These were brilliant men who could go anywhere. They weren’t there because they were at the end of their careers or this was where they were going to retire. They were there to build something, and they were engaged and excited about it. We students were thrilled too. It was a very exciting place to be.”
Dr. Story, founding head of the Division of Neurosurgery, was a faculty member in the Department of Neurosurgery at the University of Minnesota but saw developing a new medical school as a challenge, “and it proved to be. I’ve always been a little masochistic,” he said.
Dr. Johnson, professor of cell systems and anatomy, who has taught anatomy at the Long School of Medicine since 1978, said a story on the school’s 50th anniversary has to mention Carlos Pestana, M.D., Ph.D., who arrived in 1968, retired in 1997, and served as a professor of surgery and associate dean for academic affairs. “He was the main dean of curriculum and admissions when I started here,” Dr. Johnson said.

“To me, he was the person who set the whole pace for the medical school at the beginning—which students got in, what the curriculum would be. He was one of the main creative forces behind the curriculum, and people idolized him,” said Dr. Johnson. The Pestana Lecture Hall is named in the physician’s honor, and alumni established a scholarship in his name.
Overcoming challenges
Equipment was a challenge, and faculty and staff used a variety of methods to get what they needed.
Dr. Forland was one of only a few nephrologists in San Antonio, and Bexar County Hospital had one lonely kidney dialysis machine. There was a Pat Neff Junior High School student using dialysis, and the doctors presented at a school assembly in 1971 to explain what the kidney patient was enduring. The children there decided to raise the funds. “So we got our second dialysis machine from these students collecting newspapers and aluminum cans, selling cakes, and washing cars,” he laughed.

“There was not enough money for capital equipment. We had an extreme need for a tax increase,” said Dr. Forland, who formed a Faculty Assembly Ad Hoc Committee on the Financial Needs of the Bexar County Hospital in 1980. The group identified potential sources of financial support, reached out to the community with appropriate information, and created a campaign to increase the tax rate that funded the Bexar County Hospital District. They pointed to obsolete equipment, a reduction in services for outpatients, and a reduction in the number of beds for surgical services. “A teaching hospital must be a quality hospital—not a luxury hospital—but a quality hospital,” Dr. Forland wrote in a letter to a local newspaper. Later that year, Bexar County Commissioners approved a maximum tax rate.
Dr. Story was part of that emphasis on equipment and spent 29 years at the medical school. “At the time, we had terrible, primitive imaging in our hospital. We didn’t have CAT scanning and MRI here. In the early days, residents would load patients in their vehicles to transport them to Methodist Hospital for CAT scans or MRI studies and then bring them back,” he said.
Faculty from neurosurgery and other specialties worked together to obtain CAT scans and MRI equipment. The Division of Neurosurgery and the Department of Psychiatry worked together on a committee, led by Dr. Robert Leon and Dr. Story, to lay the groundwork for bringing PET scanning to the institution.
“This was no small feat and included securing a cyclotron for production of radioisotopes used for imaging. This, of course, required substantial financial investment. It was achieved by grants from the Perot Foundation, the Department of Veterans Affairs and the Department of Defense,” Dr. Story said. “The committee also brought Dr. Peter Fox to the university to lead what is now known as the Research Imaging Institute.” The institute has developed an outstanding portfolio of interdisciplinary, collaborative grants and a large and growing network of collaborators on a worldwide basis.
Witnessing changes
The changes in the last 50 years are more than the physical plant.
“One of the striking innovations is the lack of textbooks,” said Dr. Forland. “In those early years, students paid other students to take notes and to type them up,” he said, smiling as he remembered.
Dr. Holly recalled, “The heart and soul of the medical school was the library. I lived in the library. We actually took a weekly one-hour lecture in library science to teach us the value of the library. All our communications were by landline, books and articles. We copied a lot of things and carried around a lot of books.”
The school’s curriculum recently underwent a major change, with the Class of 2016 completing four years of the new CIRCLE curriculum, according to Dr. Johnson. The curriculum is now systems-based, integrating basic science and clinical information. Team-based learning and self-directed learning are emphasized with fewer lectures and more clinical and patient exposure.

“We’re teaching medicine differently—it’s very clinically based,” said Dr. Johnson, a three-time Presidential Teaching Excellence Award recipient. “We want everything they have to learn to be information that they can really use—not just good to know for knowledge sake.”
Another huge change is an entirely online curriculum. Students pay a fee to access the content in their electronic textbooks. “We expect them to build on what we give them directly in class and lab by going to the textbook and other electronic sources,” Dr. Johnson added. And, if something is momentarily confusing, “they can look it up on their own and not be stopped in their learning,” she added.
The school’s anatomy program has always had a strong dissection basis. In the transition to the new curriculum, “We were able to reduce contact hours in lecture and lab and still maintain the integrity of a dissection-based anatomy experience,” Dr. Johnson said, adding, “The trend at some medical schools has been to minimize dissection or even do everything on computers. We find electronic resources to be an enrichment to what students learn in the laboratory. Students actually tell us that they chose our medical school because it still offers a rich dissection experience.”
Those dissection labs produced lifelong friendships because the four students work on the same donated body throughout their anatomy experience. “I still hear from my lab partners,” said Dr. Olin, who was a veterinarian who switched to medical training. He praised the medical education he received in San Antonio. “When we were in rotations at Bexar County Hospital, there were interns from other parts of the country. They knew enough, but they couldn’t do as much. In our medical training, we were taught how to draw blood, use a microscope to do a blood count, and to spread material to get a culture. We got not only a very good theoretical/academic education but a practical education.”
Technological advances
Another change is how students learn about patients while in the hospital room. “Access to information has changed remarkably,” Dr. Forland said. “You would drag yourself to the library or read your textbooks at home. Now students have access to all of medicine in an electronic device in the palm of their hands.”

Dr. Johnson still has 2-inch by 2-inch Kodachrome slides in slide carousels that she used in lectures when she began teaching. “It was very laborious. Whenever you wanted to make a new image, you had to make arrangements with photography to do it. It was cumbersome and the slides got yellow with age.” Years ago, she transitioned to PowerPoint. “I also remember lecturing from printed notes typed on a typewriter before the days of computers!”
Now technology has revolutionized learning in the laboratories. Omid Rahimi, Ph.D., director of the human anatomy program and associate professor of cell systems and anatomy, created a digital anatomy laboratory at the Academic Learning & Teaching Center; the lab has become an integral part of the new CIRCLE curriculum. The digital anatomy lab does not replace the traditional gross anatomy instruction but enhances the educational experience, he said.
Dr. Rahimi said the digital lab uses 3-D technology to digitally dissect a real patient’s data, which can include CT scans and MRI images of normal and diseased anatomy. Each student has access to a computer, and the labs feature multiple big screens on the walls. “We now have photography equipment in all the rooms,” he said. “If we find something interesting in a cadaver, we can put it on a screen and show it in all four rooms. It has been a magnificent improvement.”
Z. Dave Sharp, Ph.D., professor of molecular medicine and Zachry Distinguished Chair in Molecular Medicine, recalled growing a bunch of bacteria and isolating a particular restriction enzyme while doing post-doctoral work at Rice University. “Five or six years later, you could buy all those so you didn’t have to go through all that time-consuming work. Some of the older guys sneer at this. I call it kit biology; we buy a kit to do this. It saves time.” The computer programs that have been developed for research “are really amazing,” he added.
Dr. Johnson is philosophical about the changes. ”The best of anything is a hybrid of the old and the new. There are some things that are wonderful in the old; we should not eliminate them just because they’ve been used in the past. By the same token, there are a lot of improvements that can be made by incorporating new ways of doing things that are better.”

A hub for research
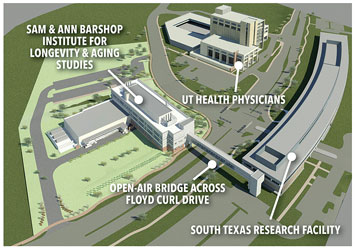
As the years continued and growth naturally occurred on the main campus, officials dreamed of an Institute of Biotechnology taking over more than 150 acres in far west San Antonio off Highway 211.
Dr. Sharp, who joined UT Health San Antonio in 1982, was among the first faculty who moved into the Hayden Head Building (which housed the Institute of Biotechnology) at the Texas Research Park in 1991. Eventually the building was full with more than 30 graduate students.

“There were 25 high-profile, high-impact science papers produced in the history of the university; 15 of them came from this building,” Dr. Sharp said proudly. The laboratories were the center of burgeoning research initiatives, such as DNA repair and tumor suppressor genes in their heyday in the early 2000s, Sharp said.
“I love this building. We’ve done so much great science in it,” the long-time scientist said as he gazed out the window of a building that is mostly empty today. As it became apparent that the institute needed the synergy that could be accomplished with medical professionals in closer proximity, plans are in place to move the occupants to the South Texas Medical Center.
Thanks to a generous donation in 2001 from Sam and Ann Barshop, the Barshop Institute for Longevity and Aging Studies was created. The institute’s facility in the Texas Research Park was dedicated in 2005; now that work will continue in a premier research center near the Greehey Campus off Floyd Curl Drive. “The Barshop Institute is world-renowned,” Dr. Sharp said, and his work has been aligned with the Barshop Institute with investigators like Drs. Randy Strong and James Nelson while they both were located at the Texas Research Park. This work will continue and expand when the researchers move in late 2019 to an extensive building closer to the Long School of Medicine.
Dr. Sharp’s and Dr. Strong’s ground-breaking work with anti-aging pharmacological interventions brought worldwide attention to the Texas Research Park because their study, performed with the National Institutes of Aging Intervention Testing Program, revealed that rapamycin could extend the lives of mice and possibly could slow the progression of some age-related diseases being studied by Barshop researchers.

Philanthropic support
Just as a 50-year marriage matures and adjusts to changes, its partners continue to make new connections and friends.
During its 50 years, the School of Medicine has created an alumni base and friends who provide the critical philanthropic element that keeps the institution moving into national prominence. Researchers and physicians need funds to continue their important work and to have the proper equipment and staff to care for patients.
At the top of that list for this institution are Joe R. Long and Teresa Lozano Long.
Both came from humble backgrounds and graduated from UT Austin. Teresa was the first Latina to receive a doctorate from the school. Joe earned a law degree and achieved great success in the banking industry. By 2017, they had donated more than $61 million to UT Health San Antonio, and their names were bestowed on UT Health San Antonio’s first school—the Joe R. and Teresa Lozano Long School of Medicine. The main campus also is named for this philanthropic couple.
“Philanthropy, clinical practice income and research grants are critical to maintaining the standards and quality of the institution. To obtain the stature that we’ve obtained has been based on the generosity of people like the Longs,” Dr. Forland said. “We are obviously tremendously grateful for that.”
Dr. Forland gave the example of the Center for Medical Humanities & Ethics, which he helped establish and has worked at since his 1999 retirement: “We receive approximately 25 percent of our budget from the state, and we have to raise the additional funds to exist.”
Dr. Holly and his wife have started endowments for enriching the students’ experience and expanding the outreach of the school and encourage their colleagues to do likewise. Dr. Holly and John Doran, M.D., FACP, are the two founding members of the school’s Aesculapian Laureate Society. The society recognizes alumni who have given more than $1 million to the medical school.
“There were men and women who devoted their lives to helping me prepare to be what I wanted to be—a doctor,” Dr. Holly said. “I felt an enormous debt of gratitude. That debt can only be repaid by me contributing to the future generations and participating in the school in any way I possibly can.”
Dr. Holly has 50 years of observation from a variety of platforms—as a student, alumnus and a benefactor. “It’s changed so dramatically,” he said. “It’s now a major health care system that’s approaching the top 10 in the nation as far as quality and research and all the other measures of excellence. It’s a remarkable evolution.”





