50 Years of Research: History of Trailblazers Taking Risks

Innovation, Dedication Mark First Five Decades of Discovery
By Susie Phillips Gonzalez

The history of research at the Joe R. and Teresa Lozano Long School of Medicine at UT Health San Antonio is one of innovation, according to Dean Robert Hromas, M.D., FACP. In the school’s early years, medical trailblazers took risks developing successful devices and medications.
Among them was the world’s first cardiac arterial stent invented and patented in the 1980s by Julio C. Palmaz, M.D., who revolutionized cardiology and peripheral vascular medicine. He was a longtime professor of radiology who was named an Ashbel Smith Professor in recognition of his pioneering work. The life-saving balloon stent has been listed as one of the “Ten Patents that Changed the World” by Intellectual Property Worldwide magazine, and Dr. Palmaz has been inducted into the National Inventors Hall of Fame.

Research—a companion pillar to academics and patient care at every medical school—is fundamental to finding answers to questions about disease, launching clinical trials, and, ultimately, developing medical treatments or procedures that prevent or cure diseases.
“Research is an indicator of the sophistication of a university,” said Andrea Giuffrida, Ph.D., vice president for research and professor of pharmacology. “It’s the yardstick we use to measure academic reputation. Our research is a sort of business card that we use to attract top scientists and students. We have gained the respect of the scientific community in multiple fields,” he added. The areas range from cancer, diabetes, neuroscience, aging and Alzheimer’s disease, post-traumatic stress disorder (PTSD), and population health.
Some of these highly regarded research advances include:
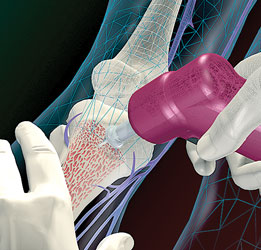
The EZ-IO® Intraosseous Vascular Access System allows quick access through the bone marrow cavity to infuse blood, medications, and fluids into critically ill patients who are having difficulty accepting traditional IV lines.
Developed by emergency room physician Larry Miller, M.D., CEO of VidaCare, for use in emergency and trauma environments, the device won the Wall Street Journal Technology Innovation Award in the gold category in 2008. The university provided research resources that helped him bring the device to market.
Jean Jiang, Ph.D., Ashbel Smith Professor and professor of biochemistry and structural biology, has developed antibodies that target a group of proteins called connexins to curtail the spread of breast cancer to bone and to aid in spinal cord research. She began this research in 1991. These proteins form channels in the cell, which play important roles in physiological and pathological processes in neuronal and skeletal tissues. Dr. Jiang, associate director of the Joint Biomedical Engineering Graduate Program of UT Health San Antonio and The University of Texas at San Antonio, is collaborating with researchers from UT Health Houston. In 2017, the group signed a licensing agreement with a pharmaceutical company in China to develop first-in-class therapies for spinal cord injury and breast cancer bone metastasis.

A discovery by co-inventors Bruno Doiron, Ph.D., and Ralph DeFronzo, M.D., increases the types of pancreatic cells that secrete insulin. This could result in a potential cure for Type 1 diabetes and may also allow Type 2 diabetics to stop insulin shots. Their therapy uses gene transfer to introduce selected genes into the pancreas. These genes become incorporated and cause digestive enzymes and other cell types to make insulin. The strategy cured diabetes in mice. Drs. Doiron and DeFronzo have the goal of starting human clinical trials in two years.
After a seven-year national study, Principal Investigator Ian M. Thompson Jr., M.D., and collaborators determined the drug finasteride, which was originally used to shrink noncancerous enlarged prostates, significantly reduces a man’s risk of developing prostate cancer. Dr. Thompson testified before the U.S. Food and Drug Administration committee on cancer drugs to support label change for the drug.
“Our history is out-of-the-box thinking,” said Dr. Hromas, adding that similar methods will be encouraged going forward. “We want to conduct innovative clinical trials for difficult diseases that no one has an answer for.”
In his area of cancer research, Dr. Hromas is leading the way with studies that “trick cancer cells into committing suicide.” It is what Dr. Hromas calls a novel approach that will soon see Phase 1 clinical trials in San Antonio at the Mays Cancer Center, the newly named home to UT Health San Antonio MD Anderson Cancer Center, where scientists are searching for new ways to treat cancer that go beyond the traditional options of surgery, chemotherapy and radiation.

One technique targets DNA pathways that could block cancer cells from replicating and even repair damage caused by chemotherapy and radiation. To enhance this field of study, one of the world’s foremost leaders in cancer research, biochemist Patrick Sung, D.Phil., will join the faculty from Yale University in January 2019, as the Robert A. Welch Distinguished Chair in Chemistry and professor of biochemistry and structural biology. Dr. Sung’s discoveries have increased the understanding of how DNA can repair damage induced by radiation, carcinogens and other causes. He is a leader in the mechanistic biochemistry of DNA repair and will serve as associate dean for research in the Long School of Medicine.
A third area of innovative cancer research involves discoveries by Tyler Curiel, M.D., M.P.H., professor and Daisy M. Skinner President’s Chair in Cancer Immunology Research, on immunology and its profound impact on cancer care and aging-related disorders. “He’s discovered a number of ways to stimulate the immune system to see a growing cancer like it is an infection,” Dr. Hromas said.
“The immune cells attack it and eat it.” Dr. Curiel, a physician-scientist, has been funded by the NIH and other entities since 1987. He is a leader of multiple collaborative grants, bringing together cancer researchers, aging experts and cancer clinical investigators for major national grants and awards.
Cancer research
The Cancer Therapy & Research Center, formerly a separate entity, has had a long relationship with the medical school since its founding in 1974. “We had an affiliation, and over time, it became a natural fit to become an integral part of the university and did so in 2007,” said Director Ruben A. Mesa, M.D., FACP.
In early 2018, UT Health launched its clinical affiliation with sister UT System institution, The University of Texas MD Anderson Cancer Center. A transformative $30 million gift from the Mays Family Foundation has resulted in the naming of the Mays Cancer Center, the newly named home to UT Health San Antonio MD Anderson Cancer Center.

One of four National Cancer Institute-Designated Cancer Centers in Texas and the only one in the region, the Cancer Center is recognized around the world, having recently received more than $40 million in external funding. Dr. Mesa notes that cancer research efforts are broad and involve cancers commonly found in the community such as liver cancer or obesity-related cancer.
More than 200 investigators are studying new cures for cancer through advances in medicines, cancer surgery and better radiation therapy. Researchers are seeking better prevention and screening techniques as well as answers for questions related to why the disease develops and how it progresses.
Drugs are continually being developed and trial tested. The Cancer Center has played a lead role in the development and testing of 20 drugs that have been approved by the FDA.
Another area where the Cancer Center has led in the fight against breast cancer is its role in founding and co-leading the largest breast cancer investigator meeting in the world. The 41st annual San Antonio Breast Cancer Symposium in December will bring almost 8,000 investigators from around the world to San Antonio. The five-day program covers clinical, translational and basic research and provides a forum for interaction, communication and education for a broad spectrum of researchers, health professionals and those with a special interest in breast cancer.
“The burden of cancer remains significant,” Dr. Mesa said. “As an NCI-Designated Cancer Center, we are specifically charged with decreasing the burden of cancer in South Texas. How we do that is an integral marriage between our efforts in research and practice.”

Health care for all
Amelie G. Ramirez, Dr.P.H., an internationally recognized cancer and chronic disease researcher and the founding director of the Institute for Health Promotion Research, knows how trends in her own backyard can exponentially expand outward to other communities.
Born and raised in Laredo, Dr. Ramirez saw firsthand how the inadequate health care for people along the Texas-Mexico border posed barriers to high-quality health care and battles with chronic disease. For the past three decades, she has devoted her career to trying to improve health by conducting research, promoting health, reaching out to the community, participating in speaking engagements, and training students to create a pipeline of researchers eager to promote health care for all. She seeks to promote health and a culture in which everyone has a fair and just opportunity to be as healthy as possible.
Dr. Ramirez and her team created Salud America!, a national program to share multimedia research and digital tools and stories to empower a national online network of more than 200,000 parents, community leaders, and health care providers, the majority of which are based in South Texas.
Evaluations have shown that exposure to Salud America! content is significantly linked to greater action by people to promote healthy system changes, such as creating shared use agreements for public use of school parks and trauma-informed care at schools.
Also the associate director of cancer prevention at the Cancer Center, Dr. Ramirez remains actively involved in research designed to improve health—such as finding that competent patient navigation reduces patients’ lag times to breast cancer diagnosis and treatment after an abnormal mammogram—while also searching for ways to encourage positive behavior changes in individuals and communities.
“We’re not just doing research for the purpose of doing research. We are doing research that engages the community in order to improve their health and help them make better health choices,” Dr. Ramirez said, adding that she works diligently to promote preventive cancer screenings and to reduce fear associated with having cancer through the explanation of treatment and follow-up care with the goal of sustaining a patient’s quality of life.
An aging battle

In the 1980s, researchers began to recognize that a patient’s quality of life was essential as part of the aging process. Edward J. Masoro, Ph.D., a pioneer in aging research and professor and chair emeritus of the Department of Cellular and Integrative Physiology, performed seminal work on the effect of calorie restriction on the longevity of rodents. In 1991, Dr. Masoro founded the university’s Aging Research and Education Center, which evolved into the Sam and Ann Barshop Institute for Longevity and Aging Studies when San Antonio philanthropists Sam and Ann Barshop made a transformative gift in 2001.
Nicolas Musi, M.D., director of the Barshop Institute, said researchers are dedicated to the study of the biology of aging. That way, they can better understand the molecular and cellular factors that control the aging process, which he explained is the single most important risk factor for many diseases, including cancer, osteoporosis, Alzheimer’s, and others. Through the emerging field of geroscience, Dr. Musi said Barshop scientists are studying the relationship of aging and the diseases of aging, looking for ways to promote a healthy aging process and prevent disease. In addition, Barshop researchers are searching for medications that target aging.
The most well-known discovery is the slowing of aging and the increasing of life span by Rapamycin, first tested in mice housed in the Texas Research Park lab of Z. Dave Sharp, Ph.D., who arrived at the Long School of Medicine in 1982.

Rapamycin, a naturally occurring bacterial product first isolated from soil taken from Easter Island, had long been federally approved to suppress organ rejection in transplant recipients. His proposal to extend the lifespan of mice almost failed to receive grant funding because reviewers thought the drug “would kill the mice.” Instead, Dr. Sharp’s research gained worldwide attention in 2009 when the findings were published in the prestigious Nature journal.
Verified by three separate experimental labs, Dr. Sharp and his team, which included the Barshop Institute’s Randy Strong, Ph.D., used dwarf mice that have an unusually long life span to determine that Rapamycin in an encapsulated form—known as eRapa—extended the lives of these mice. In July 2018, human trials began on men with low-grade prostate cancer. The drug also has the potential to slow the progression of some age-related diseases like Alzheimer’s and is being studied by Barshop researchers.
Dr. Musi also oversees grant programs funded by the National Institute on Aging, including the San Antonio Claude D. Pepper Older Americans Independence Center, launched in 2015 to investigate the aging process from the bench to the clinic, and the San Antonio Nathan Shock Center, founded 25 years ago to conduct transformative research on the biology of aging and serve as a springboard for advanced educational and training activities. In addition, Dr. Musi directs the San Antonio Geriatric Research, Education and Clinical Center, founded in 1987 to improve the life of older veterans through the advancement of research, education and clinical care in geriatrics.

Targeting Alzheimer’s
“We are very focused on understanding what it is about aging that creates pathways to disease, including Alzheimer’s disease,” Dr. Musi said. “In that regard, it is a natural marriage of scientists who are studying how the brain ages to see how it leads to Alzheimer’s. There are many interactions and collaborations with aging and Alzheimer’s research. These collaborations will get stronger and stronger as time goes by.”
That’s exactly the goal of Sudha Seshadri, M.D., FAAN, FANA, an eminent clinician, researcher and educator in the field of Alzheimer’s disease, who came to San Antonio in late 2017 as the founding director of the Glenn Biggs Institute for Alzheimer’s & Neurodegenerative Diseases.
Considered a superstar in the understanding of dementia, she is working closely with Barshop investigators toward the goal of slowing the progression of Alzheimer’s in older patients.
“Alzheimer’s is such a big expensive problem,” Dr. Seshadri said. “Nearly six million Americans have the disease as of today, and the cost to the country is nearly $300 billion. If we do nothing, it will cost three times as much by 2025. There’s no question we need to do research to find answers.”
Dr. Seshadri’s population research focuses on the genetics of Alzheimer’s as well as the lifestyle and vascular risk factors for dementia—work she began as the senior investigator for the Framingham Heart Study and brought to the Biggs Institute as the principal investigator for eight NIH grants.
She seeks to understand the entire spectrum of the disease of dementia by looking at the unique and specific aspects of a patient’s blood and brain. Dr. Seshadri plans to analyze various population subgroups and suggest different courses of treatment.
“Just as you don’t treat everyone with blood pressure or heart disease with the same approach, doctors must look at each individual Alzheimer’s patient. We know San Antonio has a high risk of diabetes and insulin resistance, and this is thought to be an important pathway to brain aging and dementia. Understanding that link better may be an important way to prevent and slow down the disease. We don’t have an option.”
While actively recruiting a team of physicians and clinicians, Dr. Seshadri said her vision for the Biggs Institute is to build a robust program that will be able to answer questions unique to the South Texas population while offering relevant research options to the rest of the country and the world. Ultimately, she wants to become one of the top 10 Alzheimer’s research centers in the country.
PTSD consortium

Like Dr. Seshadri, Alan Peterson, Ph.D., ABPP, also dreams of establishing a national center that would serve as a resource for research and clinical patient care to help military service members and veterans who are experiencing PTSD. If he is able to secure funding for the proposed National Center for Warrior Resiliency, Dr. Peterson and his team would continue their work to stem the public health crisis brought on by PTSD.
Retiring from the U.S. Air Force in 2005 after 21 years of active duty, including three deployments to war zones, Dr. Peterson is considered one of the nation’s foremost research leaders in the prevention, diagnosis, and treatment of combat-related PTSD and related conditions in active-duty military personnel and veterans.
As director of the STRONG STAR (South Texas Research Organizational Network Guiding Studies on Trauma and Resilience) Consortium and the Consortium to Alleviate PTSD, Dr. Peterson oversees more than 50 research projects funded by more than $150 million in peer-reviewed research grants with awards from the Department of Defense, Department of Veterans Affairs (VA), National Institutes of Health, and private sources. His more than 150 collaborators include researchers and clinicians with the military, VA and top universities and hospitals across the nation and even internationally.
“We are the only large group specifically researching combat-related PTSD,” said Dr. Peterson, also chief of behavioral medicine and the Aaron and Bobbie Elliott Krus Endowed Chair in Psychiatry at the medical school. “The key piece to what we do is to bring together as many of the top scientists across the country and partner with the military to evaluate the most effective treatment. This is an example of ‘team science.’ ”
During his military career, then-Lt. Col. Peterson realized he lacked sufficient treatment protocols when he encountered service members exposed to war trauma. When he retired from the Air Force, he accepted a faculty position with UT Health in 2005. From there, he began doing what he often did while active duty military, forming military-civilian partnerships to tackle pressing military-related behavioral health care needs—this time focused on the difficulty in treating combat-PTSD and related conditions. Dr. Peterson formed a coalition of investigators under the umbrella of STRONG STAR who were awarded their first consortium grant from the Department of Defense in 2008.
Among other efforts, the group’s work focused on the two leading civilian PTSD treatments—prolonged exposure and cognitive processing therapy—and evaluated them for the first time with active military. Other efforts then and since have worked to enhance these treatments to improve their efficacy with combat-PTSD and to develop and evaluate other highly promising treatment approaches. His goal and that of his many partners is to tailor treatments to the individual needs of each service member and combat veteran.
“We are dealing with someone’s mind, heart and emotion. What’s happened to one person has not happened to anyone else,” Dr. Peterson said. “We have to find what unlocks each person.”
New frontiers

For the last decade, personalized medicine has emerged in multiple medical disciplines, according to Dr. Giuffrida. The idea, he said, is for scientists to develop medications and devices that provide individualized treatments with lower costs to patients. Also gaining traction in the field of medical technology are wearable devices that go beyond step-tracking gadgets. Such wearables can collect health data that doctors can use to formulate improved and, in some cases, personalized care protocols.
Dr. Giuffrida says another hot research area involves prosthetics operated by a person’s own brain using a machine-brain interface. On the infrastructure side, Dr. Giuffrida said UT Health is creating a science accelerator that will provide educational programs and the business framework to help faculty become entrepreneurs and move ideas from the bench to the market.
“Working in research is exciting,” Dr. Giuffrida said. “It brings important value to our society. If you are a teacher, research can give you additional tools to be a better educator. If you are a student, you will learn multiple ‘transferable skills’: critical thinking, tenacity, self-control and ways to become more creative or cope with failure. Research is important whether you want to be a scientist or a health care professional. Those skills will be a valuable asset even if you want to work outside of the field of biomedicine.”
Over the past 50 years, scientists have made diverse discoveries in basic and clinical research at the medical school.
As Dr. Hromas explained, “Too many people still die of cancer, of diabetes, of Alzheimer’s disease, and other diseases. The only way to make and impact on those diseases is through research.” And, that is exactly what researchers at the Long School of Medicine are posed to do during the school’s second 50 years.






