The Future of Research – Myron Ignatius, Ph.D.

By Ginger Hall Carnes
There’s something fishy going on at the Greehey Children’s Cancer Research Institute (GCCRI)—a new zebrafish cancer model shipped all the way from Boston.
Myron Ignatius, Ph.D., assistant professor of molecular medicine, used the fish to research pediatric cancer during his postdoctoral training at Massachusetts General Hospital and Harvard Medical School. Although he joined UT Health San Antonio last October, he had to patiently wait until late spring this year to stock his aquariums in his new San Antonio lab. Boston can be cold even in April, making shipping impossible at 32 degrees.
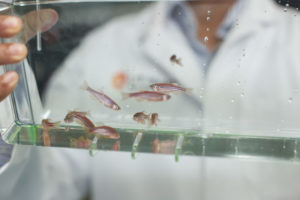
In addition, while you have to inject drugs into mice, fish swim in the water in which the drugs are dissolved, making drug screening easy.
Fish also are more economical, yet they complement well research in mice. “With each mating of a pair of fish, you’ll get between 100 to 200 embryos, pair that up with 100 breeding pairs every day and very quickly you can get thousands of animals for experiments. It’s a beautiful genetic model, because if you have numbers, you can follow what each gene is doing in a tumor.”
Dr. Ignatius decided the GCCRI was an ideal place for his research because it was created specifically to support research on childhood cancers. He wanted to work in a place where people care about fighting pediatric cancer.
Dr. Ignatius partnered with the GCCRI and UT Health San Antonio to secure a $2 million Texas recruitment award from the Cancer Prevention & Research Institute of Texas (CPRIT) to fund his research and his lab of approximately 40,000 fish.
He’s particularly thrilled to be working with Peter J. Houghton, Ph.D., who directs the GCCRI. “Dr. Houghton is a world expert in sarcomas,” Dr. Ignatius said. “He’s the one screening for drugs. It’s a unique opportunity to learn and collaborate.”
Cure rates in pediatric cancers are about 70 percent, but Dr. Ignatius is particularly focused on those children whose tumors relapse. “We know that all our treatments now are geared toward the primary tumor with radiation and chemotherapy,” he said. “But if the tumor comes back, there’s no treatment.”
Additionally, patients who survive pediatric cancer are dying in their 30s and 40s rather than having normal life spans, highlighting the need for researchers like Dr. Ignatius, who are at the cutting edge of research into future treatments.





