Scientists and patients battle an incurable disease

One morning in May 2006, multiple sclerosis launched its first assault on Antonia Santiago. And a clock began ticking.
Multiple sclerosis is a disabling disease of the central nervous system that affects nearly a million people in the U.S. MS interrupts the flow of information within the brain and between the brain and the body. Symptoms range from numbness and tingling to blindness and paralysis. The progress, severity and symptoms cannot be predicted.
Santiago woke to numbness and tingling in her left leg and foot. A strange burning sensation persisted for days.
“It took a full month to regain all the feeling, to be normal,” she said.
Brain imaging studies and a spinal tap confirmed Santiago’s MS. Although it was a cruel turn for the 20-year-old, she was fortunate to be diagnosed early. Some patients bounce from physician to physician for years with no answer, but Santiago began a weekly injectable therapy right away.
Her journey with MS was just beginning.
***
In 2018 in a laboratory at UT Health San Antonio, a genetic trick gave a young mouse the ability to walk normally. The mouse, bred to lack a gene involved in construction of nerves in the nervous system, had begun to exhibit features of MS disability such as a weakening of the legs and shuffling gait. At 10 months of age, though, the mouse scampered around like a healthy mouse, thanks to a gene rescue strategy.
The gene under study, beta IV-Spectrin, constructs part of the nervous system “highway” through which electrical impulses travel from the brain to muscles. This information highway is under attack in multiple sclerosis. Manzoor Bhat, Ph.D., Zachry Distinguished Chair in Neurosciences, and his team have shown that restoration of the defective gene is more effective if done in mice at 3 months of age rather than later when nerve damage has advanced.
Dr. Bhat believes there is a definite window of time to restore lost nerve function in MS.
***
Santiago’s first seven years with the disease were rough. Flulike side effects from the weekly injection left her in bed 1½ days a week. Thinking she would be better off without therapy, she began to skip doses. In July 2012, an MS flare-up landed her in the hospital.
“I had what seemed like an allergic reaction to an MS medication,” she said. “I broke out in hives at work. It became an exacerbation of the MS, which always starts with numbness.”
She was moved to a rehabilitation hospital that August.
“My walk wasn’t a normal walk; I felt like I was walking on coals,” she said. “And my speech was slowing down.”
Because of the burning feeling, she was afraid to touch anything. Her gait was unsteady, so the therapists gave her a walker and a fall-risk harness. They helped her walk three times a day to bring back sensation in her legs and feet.
“They got me back to walking without assistance,” she said.
Halloween 2012 was her 27th birthday. She spent it in the rehab hospital, and was finally cleared to go home that November.
***
Neurons, the core component of the nervous system, fire electrical impulses that are carried to other neurons and distant muscles. These impulses underlie a person’s cognition, sensory functions and ability to move. The neurons conduct information through axons, which are long, tree trunk-like structures insulated by a protective sheath called myelin. Healthy myelin enables the signals to travel quickly along the axons.
In MS, a person’s own immune system damages the myelin sheath. When the sheath is injured, the signals slow down dramatically, leading to the effects seen in the disease.
But myelin damage is not the end of the story in multiple sclerosis. Dr. Bhat’s team is studying mice that have a deficiency in axonal structures called the nodes of Ranvier. These nodes are gaps in the myelin sheath that function as gatekeepers and amplifiers of the electrical impulses. They, too, enable signals to travel quickly along the axonal highways.
The beta IV-Spectrin gene helps to form and maintain these structures. Mice that lack this gene form immature nodes that fall apart over time. The mice become immobile, and by 6 months of age are essentially paralyzed.
The disease is advancing; the clock is ticking.
***
Six years ago, in April 2013, a general neurologist referred Antonia Santiago to Rebecca Romero, M.D., director of the university’s Center for Comprehensive MS Care, a designation from the National Multiple Sclerosis Society. This recognition is presented to centers that offer an MS specialist and integrative, multidisciplinary treatment and care.
Santiago’s long-held wish was to go off injections and start oral therapy. Shortly after her first visit with Dr. Romero, she began taking one of three oral medications approved for MS.
The Center for Comprehensive MS Care offers the latest experimental medications to MS patients in clinical trials.
“The medicines we now have reduce MS progression by 50 percent,” Dr. Romero said. “In 1993 we had our first medication approved in MS, and now we have 14 available medications, and we continue to evolve.”
The future of MS treatment will be in neuro-repair, Dr. Romero said. “That’s the Holy Grail. How do we stimulate our own body to repair the damaged nerves, myelin and axons?”
Breaking down axonal disease into its core components, as Dr. Bhat’s lab is doing, will bring more possibilities into view.
“It’s really important research,” Dr. Romero said. “This is where new therapies will take off.”
***
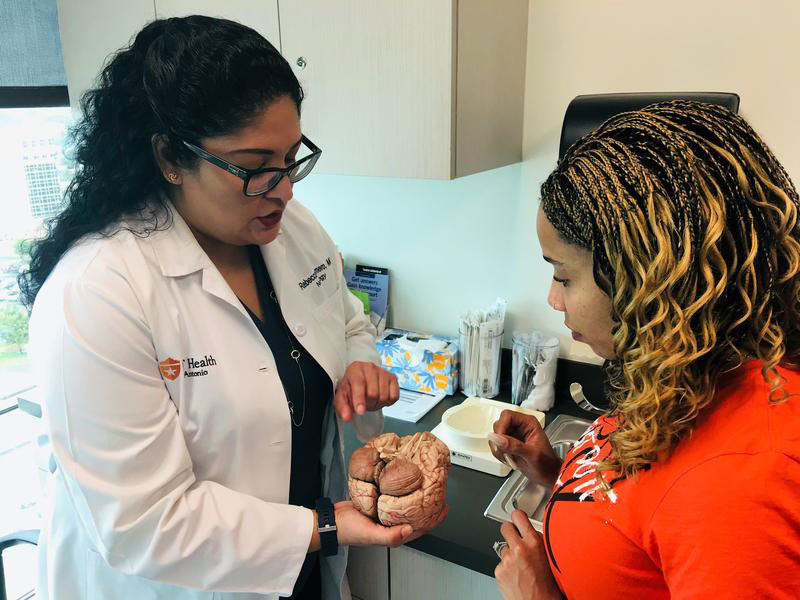
Since Santiago began seeing Dr. Romero, magnetic resonance imaging (MRI) studies of Santiago’s brain and spine have been stable. She’s had no further hospitalizations for MS flares. Numbness and tingling, however, are constant in the bottom of her feet.
Now 33, she travels around the nation talking to people about MS.
“One of the biggest obstacles to starting treatment is getting diagnosed,” she said. And as Dr. Bhat’s studies show, and outcomes of MS patients themselves reveal, time is critical.
Since the first medication for MS treatment was approved in 1993, “we now have two decades of data on patient outcomes,” Dr. Romero said. “And we know that patients who went on treatment lived longer. We also know that patients who started on medication with the first sign of MS did better long term than those who waited three to six months.”
Identifying a window of time to restore lost function in MS holds promise for future therapies, she said.
“Dr. Bhat recognized that there is a critical time and window in which nerve damage may be repaired. It’s not too far to extrapolate his findings to clinical trials we’ve seen,” Dr. Romero said.
Patients like Santiago live with the knowledge that their MS is progressing. Even in the midst of this, they harbor hope. Because if a mouse’s walking can be restored, there is promise for future MS patients.
“I just know where we were [with MS drugs] when I was diagnosed, and where we are today, and it’s exciting,” Santiago said. “I see a cure coming, maybe in my lifetime.”
To accomplish that, researchers like Dr. Bhat are racing the clock.
1 Comment
Add comment
You must be logged in to post a comment.

I have Peripheral neuropathy, is any chance the MS drugs might help improve nerve signal transmission?