By Will Sansom
Some children narrowly escape the horrors of drowning only to face a different kind of suffering: trapped inside their own bodies, awake but paralyzed, communicating by eye movements and sounds, unable to walk, speak or eat. Researchers at UT Health San Antonio identify it as “post-drowning locked-in syndrome.” New imaging studies reveal that cognitive and sensory networks are preserved in the brains of these children. The injury does not, as formerly believed, impact the entire brain, but is confined to a small area. The findings support parents’ conviction that their locked-in children are experiencing emotions, learning new ideas and developing personalities. The research also creates hope that someday the brain injury will be treatable.
Michael’s story
Sabine Summerville remembers the day as if it were yesterday. In a matter of minutes on an autumn afternoon, her son Michael’s life changed in a few feet of water.
Michael, the seventh of Sabine and Bill Summerville’s nine children, was 21 months old when he drowned in a swimming pool and was resuscitated in October 2008. Eleven children were running around the pool, making cardboard duct-taped boats in a competition to see whose would float the best.
“It was just a few moments of inattentiveness,” she said. “Honestly, when we got him out of the water I thought it would be fine. I did CPR [cardiopulmonary resuscitation], but it just didn’t work.”
Michael was in an unmedicated coma for weeks. It took him six months to slowly regain awareness. Today Michael is 11 and in a wheelchair, completely limited physically.
“I used to believe he had some purposeful movement, but now I think it is all spastic,” his mother said.
Two nurses help care for Michael during the week, giving him 24/7 management of his breathing issues and seizures. Locked-in children develop muscle contractures in areas where stretchy muscle is replaced by inelastic, fibrous muscle. Michael arches his neck backward, which tilts his head back, and because his lower jaws are contracted, he can’t close his mouth.
“It is a constant vigil readjusting his head and helping him close his mouth so he can breathe well,” Summerville said. “You can imagine it’s not comfortable to breathe.”
When Michael is calm, his muscles relax and he breathes better, she said. But then there are the seizures.
Michael may go two or three months without one and then have a spike in activity. After a scoliosis surgery in January 2017, he had seizures multiple times a day for several weeks.
The family was told he’d never be able to communicate. Yet this locked-in child does so—frequently.
“Cognitively, I believe he is a typical 11-year-old boy,” she said. “He understands literature and prefers watching documentaries. In fact, he would rather watch what the adults are watching. He likes being included in family life as much as possible.”
Michael makes quiet vocalizations, like a moan or a hum, and vowel sounds when feeling content. Every now and then—once or twice a week—he even smiles.
“His dad is the one who really gets him to smile,” Summerville said.
Michael enjoys listening to stories, particularly descriptions of the rugged Western environment in Louis L’Amour audiobooks. Documentaries about nature and heavy-duty machines used in construction are among his favorite subjects.
“He likes action and paints a picture in his mind of what he is hearing,” she said.

Photo: © Julysa Sosa / San Antonio Express-News via ZUMA Wire
Conrad’s story
Liz Tullis’ phone rang in January 2004, and it was the call no parent ever wants to receive. Her active 17-month-old toddler, Conrad, was visiting his grandparents in Temple, Texas, when he wandered into their swimming pool. He drowned and couldn’t be resuscitated until arriving at a nearby hospital.
She was out of the country at the time and only able to hear updates by phone.
“We never knew how long he was in the water,” Tullis said. “I was told he coded more than once at the hospital. They did everything they could to save him.”
Conrad was diagnosed with anoxic brain injury caused by lack of oxygen to the brain. At the time, not a lot was known about the post-drowning syndrome. What doctors did know is that Conrad would never walk or talk again.
“They told me Conrad was going to live, but they also said he would never get better, never express emotion,” she said. “They encouraged me to institutionalize him. Inside me there was a mixture of spiritual—hope—and intellectual—‘Do we really know he can’t recover?’”
She became acquainted with other parents and a common observation emerged, however. The children, seemingly locked in and unable to communicate, were surpassing doctors’ expectations.
“Verbally is just one way people communicate,” Tullis said. “We all have a repertoire of facial expressions, and Conrad is no different. Just looking at him, you can see what kind of mood he’s in. Definitely we like the smiles. If a conversation is going on, he reacts appropriately. If I say I’m going somewhere, he looks at me like, ‘Where are you going?’ It’s the same type of expressions that you would be able to understand from somebody who can talk and just isn’t. If he’s in pain, he makes a pained face. If he’s happy, he makes a happy face.
“We make him vocalize,” she said. “If we’re going somewhere, we say, ‘Do you want to go?’ and he has to make a small noise saying, ‘Yes, I want to go.’”
Now 15, Conrad attends Alamo Heights High School. School staff members send pictures and notes to tell his mother what’s going on so she can ask Conrad about it.
“He expresses whether something made him happy or sad or excited,” she said. “School staff also tell me Conrad knows when it’s going to be the next period and somebody is going to take him. They are definite about that.
“If I have him in a room and I have to go into another room, and if he feels I haven’t come back soon enough, he will let out this huge yell, like, ‘Get back in here.’ And whenever I have an audiobook of Moby-Dick playing, he sits there and listens every time and will not move. He’s been through the whole book. A friend of ours was talking about Moby-Dick, and Conrad turned his head straight over to the person and recognized the part of the book being discussed.”
Out of her experiences with Conrad and a desire to help other families, Tullis established the Conrad Smiles Fund. The fund has provided support to UT Health San Antonio research, such as networking with parents to seek their children’s participation in clinical studies.
“We were told Conrad would not be able to smile or show emotion,” she said. “But what the doctors learned in medical school was different from what we were experiencing. We’re with our kids all the time. We know. The facial cues and the sounds mean something.”
The research
Peter T. Fox, M.D., director of the Research Imaging Institute and professor in the Joe R. & Teresa Lozano Long School of Medicine, set out to find the science to prove their belief.
Drowning is the most frequent cause of unintentional injury and death in children less than 4 years of age, with more than 3,500 cases annually in the United States. Two-thirds of the time, the children survive thanks to successful CPR.
For the children who survive, but are “locked in,” the prognosis is grim.
“When someone inhales water, very quickly the heart stops beating,” Dr. Fox said. “The brain is the organ that’s greediest for oxygen. The lack of oxygen causes anoxic brain injury. By the time these resuscitated children arrive at emergency departments, they are either comatose or convulsing.”
Dr. Fox, who met the Tullis family in 2010, is trained in radiology, neurology and psychiatry, and uniquely suited to profile these children. With funding from the Kronkosky Charitable Foundation, he designed a series of studies to better understand post-drowning locked-in syndrome. The team, consisting of two doctoral students and two research staff, published its research over multiple years, including three papers in 2017. The work is changing the way these children are viewed by the medical establishment.
“This is a new syndrome,” Dr. Fox said. “It’s not taught in medical school. This is all new neuroscience.”
The researchers studied brain images of 10 children, including Michael and Conrad, and compared them to corresponding images taken in 10 healthy children. What they found confirmed their predictions and supported the experiences that parents were having with their locked-in children.
The studies showed the injury is much more restricted in scope than was previously believed. Rather than impacting the entire brain, the injury is confined to a single motor pathway. Paralysis results from injury to this pathway.
“Rather than finding damage everywhere, as everyone else expected, the injury turned out to be a small stroke,” Dr. Fox said. “Because the injury is adjacent to a blood vessel that can be accessed via catheter, it should be feasible to deliver medication to the site. This could, potentially, save children from being locked in.”
Administering clot-busting drugs used to treat an adult stroke will not work, he said, because the injury is far different, not caused by arterial plaque buildup. An agent that protects the brain would be ideal. Many ideas are being tossed about, including research at UT Health San Antonio that proposes to stimulate activity of caretaker cells called astrocytes in response to brain injury.
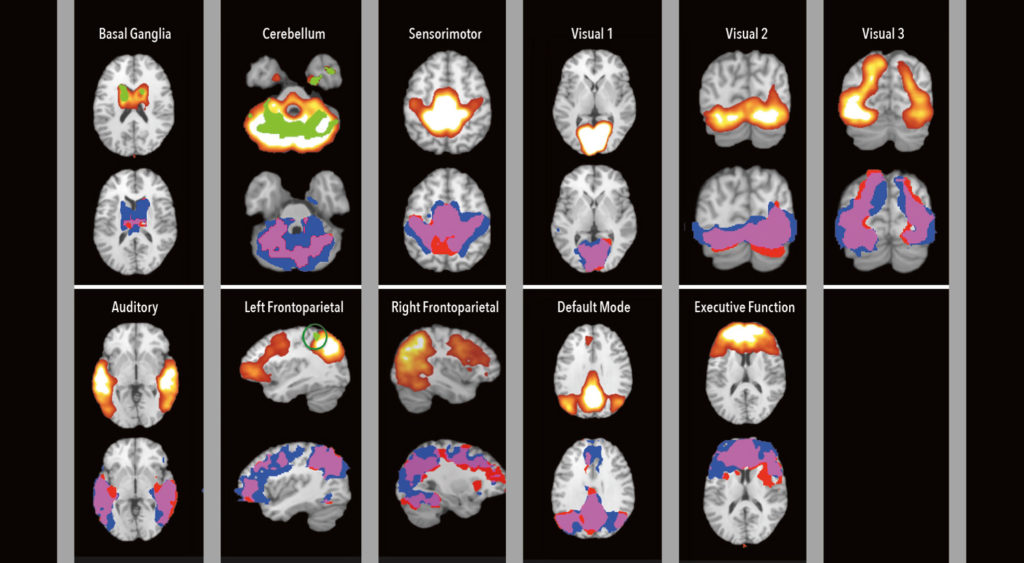
The studies also demonstrate that visual, auditory, tactile and cognitive networks are preserved in the children. This explains why the children track with their eyes, hear commands, respond to touch, and enjoy stories they hear or watch.
“Our observations suggest that the severe motor deficits observed in this population can mask relatively intact perceptual and cognitive capabilities,” Dr. Fox said.
The brain system that’s most associated with awareness is called the default-mode network. The team found a strong correlation between social behaviors and preservation of this network, he said.
“Even in the most severely affected of the children, we have evidence that at least the machinery for awareness of themselves and others remains functioning,” he said. “We can see that the machinery is still intact.”
That’s something that Tullis, who also serves as co-author on some of the studies, has suspected for years.
“These kids grow and are cognitively aware,” she said.
The new findings give hope and validation to these families, Dr. Fox said.
“What’s so important about this research is, now we have the science behind us,” Tullis said. “If this happened to us, and we are living it, we can help others around us. We want every child, like Conrad and like Michael, to reach his maximum potential—no limits.”

