UNIVERSITY IN MOTION: Kate Marmion School of Public Health announced
A transformational investment is made in the future of public health
The University of Texas at San Antonio received a transformational $30 million gift from the Kate Marmion Charitable Foundation to support the mission of the School of Public Health and improve the health of communities across South Texas.
This gift to the university and its academic health center, UT Health San Antonio, meaningfully advances the mission of this initiative and strengthens the university’s commitment to improving the health of South Texas. In recognition of the foundation’s generosity and partnership, the UT System Board of Regents approved the naming of the Kate Marmion School of Public Health in honor of Kate Marmion, the daughter of Janey Briscoe Marmion and granddaughter of former Gov. Dolph Briscoe Jr. and Janey Slaughter Briscoe.

The $30 million commitment will exponentially improve health outcomes for individuals and families across South Texas, especially in rural communities where access to quality healthcare remains limited. The gift also reflects the Kate Marmion Charitable Foundation’s focus on improving the health of rural Texans. By establishing far-reaching endowments to support the community outreach work of the school, along with new fellowships and scholarships to advance the development of a public health workforce, the gift will serve Texas in perpetuity.
“This profound investment from the Kate Marmion Charitable Foundation is a powerful testament to its enduring commitment to education, healthcare innovation and the well-being of Texans,” UT San Antonio President Taylor Eighmy, PhD, said.
South Texas faces significant health challenges, including higher rates of obesity, diabetes, heart disease and other chronic conditions that place a substantial burden on individuals and communities. These issues are compounded by limited access to healthcare and other community-level challenges that affect overall health and well-being.
“The Kate Marmion Charitable Foundation is privileged to make this gift to The University of Texas at San Antonio School of Public Health,” said Dolph Briscoe IV, president of the Kate Marmion Charitable Foundation. “A tremendous healthcare need exists in South Texas, and we are humbled by the opportunity to support the amazing faculty, staff and students at UT San Antonio in this critical effort.”
“This remarkable gift transcends far beyond a name. It honors Kate Marmion’s memory and love of South Texas, strengthens our mission and charts a path of hope and opportunity for generations,” said Francisco Cigarroa, MD, senior executive vice president for health affairs and health system at UT San Antonio.
Vasan Ramachandran, MD, FACC, FAHA, serves as the dean of the Marmion School of Public Health.
“We are profoundly grateful for this transformational gift, which allows us to confront the underlying factors that drive persistent health disparities in South Texas,” Ramachandran said.
This gift will position the school to continue providing state health improvement initiatives, including rural health, chronic disease prevention and child health. It will also augment workforce pipelines that prepare and deploy health professionals to serve underserved regions across Texas.
Health professional schools are a proven workforce pipeline
At the end of the 2025 academic year, more than 1,100 graduates from the university’s health professional schools joined the ranks of over 45,000 alumni advancing health and discovery across Texas and beyond its borders. Collectively, they represent the state’s largest producer of health professionals —physicians, nurses, dentists, biomedical scientists and allied health experts committed to meeting the growing demand for care.
On Sept. 1, The University of Texas Health Science Center at San Antonio and The University of Texas at San Antonio merged to become UT San Antonio. Both of the independently designated Research 1 institutions are now united in advancing a shared vision for discovery, education and care. The highlights that follow detail recent achievements of the university’s six health professional schools.
Building momentum
The first Master of Public Health student cohort of the Kate Marmion School of Public Health is progressing toward graduation in 2026 — a milestone for the region’s newest public health graduate school. In summer 2025, the school began co-administering the Doctor of Medicine/Master of Public Health dual degree with the Long School of Medicine. The school will also launch two new programs in fall 2026: a Graduate Public Health Certificate for non-degree-seeking working professionals, and an epidemiology concentration for master’s students.
Fostering excellence
The School of Nursing now ranks in the top 11% of Bachelor of Science in Nursing programs nationwide in U.S. News & World Report’s 2026 Best Colleges listing. The school was also named one of the National League for Nursing’s 2025 Centers of Excellence in Nursing Education, 2026 Best Colleges listing. The school was also named one of the National League for Nursing’s 2025 Centers of Excellence in Nursing Education, becoming San Antonio’s only nursing school with this distinction, which recognizes exceptional innovation and commitment to preparing skilled, compassionate nurses.
Filling critical gaps
The School of Health Professions celebrated two milestones in 2025: the graduation of its first Master of Science in Imaging Sciences class and the program’s initial accreditation by the Joint Review Committee on Education in Radiologic Technology. The program is the only entry-to-the-profession master’s in the nation offering eligibility for three American Registry of Radiologic Technologists certifications.
Addressing community needs
In Spring 2025, the Joe R. and Teresa Lozano Long School of Medicine’s Doctor of Medicine/Master of Public Health program officially came under one roof. The dual degree prepares physicians to connect patient care with population health sciences, blending training in epidemiology, policy and prevention. The school’s Addiction Medicine Fellowship likewise responds to community needs. Open to physicians from any specialty, the Accreditation Council for Graduate Medical Education-accredited program trains fellows at UT San Antonio’s Be Well Institute on Substance Use and Related Disorders and the South Texas Veterans Health Care System to diagnose and treat substance use disorders.
Expanding pathways
The Graduate School of Biomedical Sciences is broadening opportunities for students to pursue innovation and strengthen the region’s biomedical workforce. The new Master of Science in Drug Discovery and Development trains students across all stages of drug creation, preparing them for roles in biotechnology and pharmaceutical research. The Graduate Certificate in Medical Physics offers doctoral-level scientists and engineers a pathway into clinical practice and prepares graduates for accredited residencies and board certification.
Leading interdisciplinary discovery
Ranked No. 1 in Texas and 30th worldwide in dentistry and oral sciences by the Academic Ranking of World Universities’ 2024 Global Ranking of Academic Subjects, the School of Dentistry continues to strengthen its global reputation through innovative research and education. The school’s Center for Pain Therapeutics and Addiction Research recently secured its first National Institutes of Health grants to advance studies in nonopioid pain management, offering students new avenues for research and interdisciplinary training.
EXPANDING CARE: Where care and discovery come together
New Center for Brain Health pairs advanced research with clinical care of individuals facing neurological conditions
UT Health San Antonio’s Center for Brain Health, which opened Dec. 10, brings clinical care, innovative research and caregiver support together under one roof to revolutionize how diseases of the brain are understood and treated.
The $100 million, 103,000-square-foot center is designed to provide a comprehensive and hopeful experience for individuals facing neurological diseases while advancing the science behind diagnosis and treatment.

The idea for the new building began more than seven years ago, sparked by a vision to create a dedicated space for patient care and research. That vision resonated across the San Antonio community, prompting more than $40 million in philanthropic support to help make that dream a reality. And in November, Texas voters approved a state constitutional amendment establishing a $3 billion state fund to accelerate research, treatment and prevention of Alzheimer’s disease and related dementias.
“This center is the culmination of years of effort to build a space that not only meets the care needs of patients and families, but also expands our research capacity,” said Sudha Seshadri, MD, DM, neurology professor and founding director of the Glenn Biggs Institute for Alzheimer’s and Neurodegenerative Diseases at UT Health San Antonio.
“It’s deeply meaningful to me, both personally and professionally, to offer not just treatment, but respect for each person’s uniqueness. A diagnosis doesn’t define a person, and it certainly doesn’t stop their story.”
A new model for neurological care
The Center for Brain Health is set to redefine the treatment of conditions like Alzheimer’s, dementia, stroke, amyotrophic lateral sclerosis (ALS) and Parkinson’s. Multispecialty care teams include neurologists, therapists, counselors and support staff in one location, reducing the need for multiple appointments. The center features 75 exam rooms, 12 infusion chairs for newly approved and investigational treatments, and specialty spaces for therapy, diagnostics and wellness.
Other services include geriatric psychiatry, nutrition, neuropsychology, genetic counseling, physical therapy and mental health support for patients and caregivers.
Community spaces are available to host support groups and educational events, reinforcing the center’s role as a hub for families and anyone affected by neurological conditions.
“This is more than a building, it’s a new model for neurological care,” said Carlayne Jackson, MD, FAAN, chair of the Department of Neurology. “Our patients need comprehensive assessments, imaging, neuropsychology testing, family services and more. All of that is available here in a single, coordinated location.”
Jackson said what excites her most about the center is the integration of patient care and research.
“Being able to manage patients in the same space where research and clinical trials are happening is something we’ve never had before,” said Jackson.
The center includes a bridge to the institution’s Medical Arts and Research Center, is near the UT Health San Antonio Multispecialty and Research Hospital and is across the street from the Sam and Ann Barshop Institute for Longevity and Aging Studies, enhancing collaboration across research and clinical care teams.
“The Center for Brain Health represents hope — a place where care and discovery come together to preserve brain health, ensure early diagnosis and help people keep doing what they love for as long as possible,” Seshadri said.
Advanced imaging technology
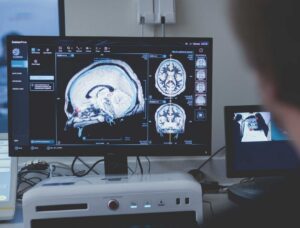 UT San Antonio’s 7-Tesla Terra.X magnetic resonance imaging (MRI) scanner — Texas’ first — housed within the Center for Brain Health, is one of the most powerful imaging technologies available. This system provides ultra-high-resolution brain scans to guide early diagnosis and novel research to aid the study of conditions like Alzheimer’s, Parkinson’s and other brain diseases.
UT San Antonio’s 7-Tesla Terra.X magnetic resonance imaging (MRI) scanner — Texas’ first — housed within the Center for Brain Health, is one of the most powerful imaging technologies available. This system provides ultra-high-resolution brain scans to guide early diagnosis and novel research to aid the study of conditions like Alzheimer’s, Parkinson’s and other brain diseases.
Compared to standard MRI, the 7T offers dramatically improved resolution, especially in deep or complex regions such as the brain stem and temporal lobes. In clinical use, this can help distinguish between minute differences that are not visible with lower-powered scans. For example, the 7T can more accurately distinguish between a benign blood vessel and an aneurysm, potentially sparing a patient from unnecessary surgery. The level of detail provided, even without contrast, can reveal deep structures like the brain stem, where many diseases begin, and veins where amyloid is cleared.
By offering this cutting-edge MRI locally, UT Health San Antonio can reduce the burden of travel for patients and expand access to high-resolution imaging that might change the course of their diagnosis or treatment.
EXPANDING CARE: An anchor for healthcare expertise
UT Health San Antonio’s first inpatient hospital expands mission to serve South Texas
In the year since the UT Health San Antonio Multispecialty and Research Hospital opened its doors in December 2024, expansion of the institution’s healthcare expertise and services and its delivery of quality patient care for the community have only gained momentum.
Among the hospital’s many milestone accomplishments:
- Earned The Joint Commission’s Gold Seal of Approval — a top national symbol of credibility and trust that reflects the hospital’s excellence in safety, rigorous performance standards and high-quality patient care.
- Opened a dedicated oncology unit, staffed by a specialized cancer care team providing inpatient chemotherapy and full-spectrum cancer care.
- Established a Stem Cell Transplant and Cellular Therapy program, a critical community need and region-defining service that will deliver advanced immunotherapies and specialized care for patients with blood cancers and blood disorders.
- Launched UT Health San Antonio’s first Blood Donor Center, ensuring life-saving blood availability for surgeries, blood disorders and cancer care.
- Expanded access to an Advanced Care Clinic for UT Health San Antonio primary care patients and patients with cancer who need immediate advanced evaluation or hospital-level care.
- Performed procedures spanning multiple specialties, including orthopaedic total joint replacement and complex spine surgery, as well as advanced oncologic procedures such as robotic lymph node dissection for testicular cancer.
- Became the first hospital in Texas to advance safer, multimodal pain management by deploying a new FDA-approved non-opioid pain medication following orthopaedic and podiatric surgeries.
- Opened recruitment for the hospital’s first inpatient phase 2 cancer clinical trial, expanding access to promising new therapies and advancing cancer research and treatment in South Texas.
The hospital is part of a comprehensive network of inpatient and outpatient care locations across the region that comprise UT Health San Antonio, the clinical care and clinical research health system of The University of Texas at San Antonio. Collectively, UT Health San Antonio medical, dental, nursing and allied health professionals conduct more than 2.5 million patient visits annually.
Modeling high-tech service
 The UT Health San Antonio Multispecialty and Research Hospital incorporates innovative pharmacy technologies, including robotic couriers, personalized automated dispensing cabinets and pneumatic tube systems for faster delivery of medications. Among other operational efficiency efforts, clinical lab services across all UT Health San Antonio patient care locations are now consolidated at the hospital’s 24/7 laboratory to support inpatient and high-volume outpatient care and provide faster diagnoses to improve patient outcomes.
The UT Health San Antonio Multispecialty and Research Hospital incorporates innovative pharmacy technologies, including robotic couriers, personalized automated dispensing cabinets and pneumatic tube systems for faster delivery of medications. Among other operational efficiency efforts, clinical lab services across all UT Health San Antonio patient care locations are now consolidated at the hospital’s 24/7 laboratory to support inpatient and high-volume outpatient care and provide faster diagnoses to improve patient outcomes.
Pioneering new treatments
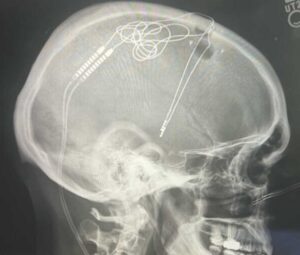 UT Health San Antonio neurologists are among the nation’s first to use technology enabling deep brain stimulation that adapts as symptoms change. Known as DBS, deep brain stimulation is the placement of electrodes in the brain connected to a battery-operated generator in the chest similar to a cardiac pacemaker. A small impulse of electricity moves from the generator to the electrodes to stimulate a specific area of the brain, relieving some symptoms and side effects for those with Parkinson’s disease, dystonia, epilepsy and essential tremor conditions.
UT Health San Antonio neurologists are among the nation’s first to use technology enabling deep brain stimulation that adapts as symptoms change. Known as DBS, deep brain stimulation is the placement of electrodes in the brain connected to a battery-operated generator in the chest similar to a cardiac pacemaker. A small impulse of electricity moves from the generator to the electrodes to stimulate a specific area of the brain, relieving some symptoms and side effects for those with Parkinson’s disease, dystonia, epilepsy and essential tremor conditions.
Until now, those electrical impulses had to be manually adjusted with doctor visits for those with implanted sensing DBS generators. The new adaptive DBS technology essentially is a software update that sets the generator battery to continually adjust stimulation based on the patient’s symptoms, using a tablet like an iPad that connects through Bluetooth.
Leading recovery support for opioid use disorder
Be Well Texas, an initiative of the Be Well Institute on Substance Use and Related Disorders at UT San Antonio, has been selected by the Texas Health and Human Services Commission to lead a major expansion of opioid use disorder recovery support services across the state. The initiative is part of a broader strategy aimed at reducing overdose deaths and building a lasting recovery infrastructure. The funding enables Be Well Texas and its partners across the state to expand treatment access, improve continuity of care and reach both rural and urban communities most in need with lifesaving services.
 As the lead agency, Be Well Texas will provide technical expertise, oversight and implementation support through a comprehensive network of treatment, recovery and provider engagement programs backed by the Be Well Institute’s clinical and public health experience. Since 2021, the Be Well Texas initiative has served as a trusted partner in the state’s overdose prevention efforts.
As the lead agency, Be Well Texas will provide technical expertise, oversight and implementation support through a comprehensive network of treatment, recovery and provider engagement programs backed by the Be Well Institute’s clinical and public health experience. Since 2021, the Be Well Texas initiative has served as a trusted partner in the state’s overdose prevention efforts.
Additionally, the Be Well Clinic, a flagship program of the Be Well Institute, delivers compassionate, evidence-based care for individuals starting or continuing their recovery journey through both in-person and statewide telehealth services. The clinic recently expanded to include comprehensive care for adolescents and young adults as young as 11, ensuring youth and families have early access to high-quality, integrated treatment.
Separately, the Be Well Institute has launched Nalaxone Texas, which distributes free, lifesaving opioid overdose medication and training to individuals and organizations throughout the state. Recently, Naloxone Texas has increased partnerships with colleges and universities to share resources and training with students, faculty and staff. Naloxone, known commercially as Narcan, is a fast-acting medication that reverses an opioid overdose and has saved countless lives.
These initiatives are supported with funding from the Texas Health and Human Services Commission, the Department of State Health Services and the state legislature.
Powering athletic performance
 UT Health San Antonio is the official sports medicine partner of the San Antonio Missions, marking the latest in a series of partnerships that support athletes at every level. The partnership with UT Health San Antonio’s nationally recognized sports medicine program builds on similar collaborations with the San Antonio Spurs and UTSA Athletics and gives Missions players access to the institution’s full network of specialists and services, including advanced diagnostics and imaging and rehabilitation services.
UT Health San Antonio is the official sports medicine partner of the San Antonio Missions, marking the latest in a series of partnerships that support athletes at every level. The partnership with UT Health San Antonio’s nationally recognized sports medicine program builds on similar collaborations with the San Antonio Spurs and UTSA Athletics and gives Missions players access to the institution’s full network of specialists and services, including advanced diagnostics and imaging and rehabilitation services.
Advancing life-saving cancer care
UT Health San Antonio’s Mays Cancer Center, the only National Cancer Institute-designated cancer center serving South Texas, is also the only provider in South Texas offering a novel targeted molecular therapy using a radioactive drug to fight metastatic prostate cancer. Whereas chemotherapy kills both cancer cells and good cells throughout the entire body, this new treatment binds to and kills only prostate cancer cells.
The new treatment is a game changer for men who have failed multiple other types of treatment including chemotherapy. In 2025, Mays Cancer Center was named among the nation’s leading hospitals and health systems for excellence in oncology programs by Becker’s Hospital Review. This list highlights cancer centers led by world-renowned experts who are driving innovation, ensuring patient safety and pushing the boundaries of what’s possible in cancer treatment and research.
BREAKTHROUGH RESEARCH: A top-ranked world leader in health research
Global rankings underscore the commitment of university investigators to improve health through discovery
The recent integration of The University of Texas Health Science Center at San Antonio and The University of Texas at San Antonio joined two Carnegie R1 universities — the highest designation for research activity reserved for the top 5% of research institutions in the United States. The new UT San Antonio merges deep expertise in biomedical and health professional education, research and clinical care with excellence in engineering, artificial intelligence, cybersecurity, business, education and the liberal arts.
The combined university also brings together more than $486 million in annual research expenditures, which helps to drive San Antonio’s $44.1 billion healthcare and biosciences industry. These research investments translate into new medications, treatments and therapies that directly benefit patients and families.
UT San Antonio’s Health Science Center, the region’s only academic health center, ranked in the top 2.4% of universities worldwide in the 2025 Center for World University Rankings, reaffirming its position as a global leader in biomedical discovery and innovation. It ranked 84th out of 5,868 healthcare institutions worldwide and 38th in the United States in the 2025 Nature Index of healthcare institutions for research output. This places the institution among the top 2% of healthcare institutions globally.
In the past five years, the university’s academic health center has conducted more than 600 clinical research projects leading to advancements in the treatment of cancer, aging-related diseases, Alzheimer’s and other neurodegenerative diseases, infectious diseases, mental health, substance use disorders, cardiovascular disease and metabolic diseases including diabetes.
The highlights that follow provide a glimpse of the broad and impactful work of investigators from across the institution to discover and test new therapies, prevent and treat disease and preserve and improve health across the lifespan.
Compound derived from chili peppers has anticancer effects
 Researchers from the School of Dentistry and UT Health San Antonio’s Center for Innovative Drug Discovery have discovered a promising compound called CIDD99 to treat human papillomavirus-negative oral squamous cell carcinoma, a form of oral cancer that is notoriously aggressive, painful and difficult to treat. The five-year survival rate hovers around 50%, and treatments have changed little in the past half-century. Derived from capsaicin, the spicy compound found in chili peppers selectively blocks calcium signaling in cancer cells by targeting a protein that is overexpressed in tumor cells but not in healthy tissue. Early tests in animal models showed that CIDD99 reduced tumor volumes fivefold, with no observable side effects. Early results also suggest this compound may have broad applicability in multiple cancer types, including lung, breast, prostate, brain and endometrial cancers.
Researchers from the School of Dentistry and UT Health San Antonio’s Center for Innovative Drug Discovery have discovered a promising compound called CIDD99 to treat human papillomavirus-negative oral squamous cell carcinoma, a form of oral cancer that is notoriously aggressive, painful and difficult to treat. The five-year survival rate hovers around 50%, and treatments have changed little in the past half-century. Derived from capsaicin, the spicy compound found in chili peppers selectively blocks calcium signaling in cancer cells by targeting a protein that is overexpressed in tumor cells but not in healthy tissue. Early tests in animal models showed that CIDD99 reduced tumor volumes fivefold, with no observable side effects. Early results also suggest this compound may have broad applicability in multiple cancer types, including lung, breast, prostate, brain and endometrial cancers.
Immune resilience may increase lifespan
A study from the Long School of Medicine identifies immune resilience — how the body counters disease drivers — as a measurable, adaptable trait that supports healthy aging. Analyzing data from more than 17,500 people, researchers found that individuals with high immune resilience at age 40 lived an average of 15.5 years longer than those with low resilience. This advantage disappeared by age 70, suggesting the trait may be modifiable until that point. The team pinpointed a key marker of resilience linked to better health, stronger vaccine responses and lower disease risk. The findings highlight a shift from treating disease to strengthening the body’s inherent capacity for health through lifestyle, medications or future immunotherapies.
Tai chi meets scientific rigor to transform health
 University researchers are using reflective markers to analyze how tai chi affects balance, coordination and joint load. For older adults or those with knee osteoarthritis, certain movements enhance mobility while others may increase joint stress. This work contributes to the growing field of integrative medicine, which combines conventional care with evidence-based complementary therapies to improve health and reduce reliance on medication. One promising focus explores tai chi’s potential to reduce fall risk in older adults with dementia by targeting both mobility and cognition. The team is also developing AI tools that use motion and health data to create personalized tai chi regimens, tailoring treatment for each patient’s needs.
University researchers are using reflective markers to analyze how tai chi affects balance, coordination and joint load. For older adults or those with knee osteoarthritis, certain movements enhance mobility while others may increase joint stress. This work contributes to the growing field of integrative medicine, which combines conventional care with evidence-based complementary therapies to improve health and reduce reliance on medication. One promising focus explores tai chi’s potential to reduce fall risk in older adults with dementia by targeting both mobility and cognition. The team is also developing AI tools that use motion and health data to create personalized tai chi regimens, tailoring treatment for each patient’s needs.
New criteria could provide early warning of Type 2 diabetes
A first-of-its-kind study challenges conventional thinking about the onset of Type 2 diabetes, identifying a risk category before prediabetes called “preprediabetes.” The study suggests that changes in the body that lead to Type 2 diabetes occur long before current diagnostic thresholds for prediabetes are met and found that one measurement — one-hour glucose levels during an oral glucose tolerance test — is far better at predicting future disease than the current two-hour glucose test. The researchers believe that, especially for high-risk patients and those with family histories of diabetes or cardiovascular disease, early screening and treatment could dramatically reduce rates of progression to prediabetes and Type 2 diabetes.
A psychedelic drug may help treat military members with PTSD
 UT San Antonio researchers, in collaboration with Emory University, received a $4.9 million grant to test whether combining MDMA, also known as ecstasy, with therapy can improve recovery rates for posttraumatic stress disorder. Clinical trial participants will receive either a single dose of MDMA or a placebo early in treatment alongside intensive Prolonged Exposure therapy, which helps patients safely process traumatic memories. Researchers hope the drug’s properties will enhance therapy effectiveness, leading to greater symptom relief, reduced depression and suicidal ideation and improved readiness and relationships. If successful, the approach could revolutionize PTSD treatment in military and veteran health systems, where Prolonged Exposure therapy is already a standard of care.
UT San Antonio researchers, in collaboration with Emory University, received a $4.9 million grant to test whether combining MDMA, also known as ecstasy, with therapy can improve recovery rates for posttraumatic stress disorder. Clinical trial participants will receive either a single dose of MDMA or a placebo early in treatment alongside intensive Prolonged Exposure therapy, which helps patients safely process traumatic memories. Researchers hope the drug’s properties will enhance therapy effectiveness, leading to greater symptom relief, reduced depression and suicidal ideation and improved readiness and relationships. If successful, the approach could revolutionize PTSD treatment in military and veteran health systems, where Prolonged Exposure therapy is already a standard of care.
Targeted drug offers hope for treatment of liver disease
San Antonio and South Texas have among the nation’s highest rates of obesity and diabetes, which is a major risk factor for metabolic dysfunction-associated steatotic liver disease, or MASLD, a chronic condition in which fat that builds up in the liver can lead to inflammation and damage. A study co-led by university researchers identifies a promising new drug candidate that could slow MASLD progression and prevent cirrhosis and liver cancer. The novel drug is a senolytic, a therapy that targets and eliminates senescent, or “zombie,” cells that drive inflammation and tissue damage. The drug works by degrading two proteins that help these harmful cells survive without the toxic side effects of previous senolytics. This discovery could represent a major step toward effective treatment for MASLD, addressing a critical unmet medical need in liver health.
Researchers identify novel drug target for AML
Despite advances in treatment, acute myeloid leukemia, or AML, still has a five-year survival rate of only about 30%. Researchers from the Long School of Medicine and Mays Cancer Center have identified a key driver of the disease, a protein called paraspeckle component 1 that is not needed for normal blood cell development but is essential for AML progression. When this protein was suppressed in human AML cells and mouse models, cancer cell growth decreased, and normal blood cell production was unaffected. Because this protein is overexpressed in AML and in 21 other cancer types, this finding could pave the way for new targeted therapies with broad applications across oncology.
For more stories and in-depth coverage of the life-saving and life-changing research being conducted at the UT San Antonio Health Science Center campus, visit Newsroom.
UNIVERSITY IN MOTION: UTSA to merge with UT Health San Antonio
The University of Texas System Board of Regents in August authorized the integration of The University of Texas Health Science Center at San Antonio and The University of Texas at San Antonio to create one unified institution by 2025. The regents also unanimously voted to name UTSA President Taylor Eighmy as its president once the combined institution is approved by accrediting entities.
“Great cities and great universities make each other better. It is time to marshal the talent, size and scale of UTSA and UT Health San Antonio to multiply their roles as global leaders in education, health care and innovation,” said Board of Regents Chairman Kevin P. Eltife. “By bringing together all of their complementary and unique strengths, we will give Texans access to the best education, discoveries and health care imaginable, while accelerating the university’s trajectory as a top U.S. and global university.”
Key to the plan was the decision to fully leverage the individual contributions of UT Health San Antonio and UTSA. UT Health San Antonio, the largest academic health research institution in South Texas, ranks in the top 3% globally for National Institutes of Health funding. UTSA, a top-tier (Carnegie R1) research institution, educates 35,000 students across seven colleges and interdisciplinary schools.
According to the U.S. Census Bureau’s most recent data, San Antonio, the nation’s seventh-largest city and the second largest in Texas, added nearly 22,000 new residents between July 2022 and July 2023 — more than any other city in the U.S. As a critical gateway to South Texas, which is home to 5.5 million people and projected to grow to 6.1 million by 2040, San Antonio’s global influence continues to expand.
James C. “Rad” Weaver of San Antonio, vice chairman of the Board of Regents, said the decision was one of the most important transformational steps the two UT institutions will take together for the long-term benefit of the city and state.
“This merger is the catalyst that will supercharge our region as a national leader in learning, innovation, health and economic vigor,” Weaver said.
To ensure a smooth transition, Eighmy and Robert Hromas, MD, FACP, acting president of UT Health San Antonio, will tap the expertise of faculty, researchers and administrators who will serve on transition teams and working groups to ensure accreditation and other approvals, as well as streamlined, timely, strategic processes to operationalize the university.
“The impact of a unified presence is undeniable, and Texas will benefit immensely from this integration, which among many benefits, will enable greater public impact and enhanced global competitiveness,” said UT System Chancellor James B. Milliken. “This initiative is about expanding and growing to align with the needs of the region and state, and to maximize the potential of two UT institutions that exist only miles apart.”
The combined institution would become the third-largest research university in Texas, with annual research expenditures nearing $470 million, encompassing six federally funded research and development centers.
UT System officials said it will be poised to achieve new heights in securing research funding, forging industry and government partnerships, attracting philanthropic investments and pioneering groundbreaking innovations. It will also draw top-tier faculty, staff, students, researchers and health care professionals from around the world.
Among other recent academic developments: the first graduates of a dual degree program in medicine and artificial intelligence, construction of a 95,500-square-foot research lab, the opening of a lab for spinal cord injury rehabilitation research, a new program for Certified Registered Nurse Anesthetists and launch of the School of Dentistry’s Center for Global and Community Oral Health.
First graduates of dual degree in medicine and AI
At the university’s May 2024 commencement, fourth-year medical students Aaron Fanous and Eri Osta became the first graduates of the nation’s first dual degree program in medicine and artificial intelligence. The MD/MSAI dual degree program, which officially launched in fall 2023, combines a Doctor of Medicine degree from The University of Texas Health Science Center at San Antonio’s Joe R. and Teresa Lozano Long School of Medicine and a Master of Science in Artificial Intelligence from The University of Texas at San Antonio.
AI’s presence is already evident in customized patient treatment plans, robotic surgeries and drug dosage. The aim of the five-year program is to enable physicians to lead in the practical use of artificial intelligence to improve diagnostic and treatment outcomes and to prepare students for next-generation AI and its impacts on the future of health care research, education, industry and administration.
Science One bolsters research profile
Plans to commence construction of a new lab facility this fall will significantly expand the university’s footprint, bolster its already robust research profile and provide new learning opportunities for students within the Graduate School of Biomedical Sciences and beyond.
Graduate School of Biomedical Sciences and beyond.
The $100 million Science One building is part of a massive expansion of the university’s research and patient care missions. The five-story, 95,500-square-foot building will house laboratory space dedicated to researching the diseases that impact the community most.
“UT Health San Antonio is renowned for world-class research in cancer, dementia, aging and diabetes, and we will put experts from each of these diseases in our Science One building,” said Robert Hromas, MD, FACP, acting president of UT Health San Antonio.
“This new facility will allow our experts to share techniques, fostering new ideas that will lead to innovative breakthroughs that will not only provide economic development for San Antonio and South Texas, but also better health care for patients suffering from these diseases.”
Construction is projected to complete in August 2026.
NeuroRecovery Research Lab opens
 This past June, the School of Health Professions celebrated the official opening of its NeuroRecovery Research Lab dedicated to spinal cord injury rehabilitation research. The lab is housed in the school’s rehabilitation services clinical space at the Mays Cancer Center, home to UT Health San Antonio MD Anderson Cancer Center.
This past June, the School of Health Professions celebrated the official opening of its NeuroRecovery Research Lab dedicated to spinal cord injury rehabilitation research. The lab is housed in the school’s rehabilitation services clinical space at the Mays Cancer Center, home to UT Health San Antonio MD Anderson Cancer Center.
The lab’s centerpiece, the PowerStep, is a computerized body weight-supporting treadmill system that enables hands-on, activity-based therapy interventions. Data collected during therapy sessions on the system are shared with other researchers of the NeuroRecovery Network, an international group of rehabilitation centers that develop and provide therapies to improve functional recovery and health among people living with paralysis.
Therapies on the PowerStep include step retraining, step adaptability, segmental trunk control drills, coordination activities and anticipatory balance activities. Patients receive a full ensemble of sensory facilitation, which enables motor recovery in an environment in which they feel safe. The treadmill’s harness removes patients’ fear of falling, enabling them to participate in interventions to regain motor control.
Nurse anesthetist program welcomes first students
To help fill critical demands for anesthesia services, the university’s School of Nursing welcomed its inaugural cohort of 18 students this fall into its newly launched Bachelor of Science in Nursing to Doctor of Nursing Practice-Nurse Anesthesia program.
The three-year, full-time, first-of- its-kind program for South Texas will provide students with the skills and knowledge to offer safe and individualized anesthesia care across all age groups. At the conclusion of the program and after passage of the nurse anesthesia certification exam, these Certified Registered Nurse Anesthetists (CRNA) can work with various medical practitioners providing all types of anesthesia services, including sedation, general and regional anesthesia and pain management.
Currently, there are only four CRNA programs in Texas, with the next-closest programs located in Dallas-Fort Worth and in Houston.
School of Dentistry adds to academic, research impact
Since its launch in 2023, the UT Health San Antonio School of Dentistry’s Dental Hygiene program at UT Education and Research Center at Laredo (UT Center at Laredo) has kept pace with its goal to admit eight more students this past July at the start of its second year of offering the degree program.
(UT Center at Laredo) has kept pace with its goal to admit eight more students this past July at the start of its second year of offering the degree program.
The Bachelor of Science in Dental Hygiene degree program is the first of its kind in Laredo, aimed at addressing significant gaps in oral health care needs within the community while boosting local job opportunities in a high-demand field. The dental hygiene courses at the center are taught live and through distance learning by UT Health San Antonio School of Dentistry faculty, and in-person dental hygiene faculty teach at the new simulation and radiology labs there and at community clinics where students also get practical experience.
In addition to broadening its academic reach, the School of Dentistry continues to expand its research focus with the launch of its Center for Global and Community Oral Health in September 2023. The center brings together various outreach and research programs under one umbrella to study and develop solutions to the most pressing dental challenges facing global populations today.
This fall, the school launched its Center for Regenerative Sciences, a new research initiative to position the university at the forefront of regenerative dentistry and medicine, with a focus on the development of advanced tissue regeneration strategies.
EXPANDING CARE: Building health care transformation
With $1 billion in infrastructure expansions underway, UT Health San Antonio is on a historic growth trajectory, shaping the future of health care for the region and positioning the institution as an essential force for improving human health for generations to come
UT Health San Antonio is in the midst of significant transformation, evolving from a premier provider of outpatient care to an integrated health care delivery system that will soon include inpatient services at the UT Health San Antonio Multispecialty and Research Hospital, opening this December.
The new hospital will enhance the institution’s continuum of care, allowing for better integration and alignment with established outpatient programs, such as Mays Cancer Center, home to UT Health San Antonio MD Anderson Cancer Center. This evolution of care is driven in large part by the rapid growth in health care demands within the surrounding community.
Part of the $1 billion in capital investments in support of UT Health San Antonio patient care expansion over the next several years is construction of a $100 million Center for Brain Health. The new facility, which will connect by an enclosed corridor to the UT Health Medical Arts and Research Center, will advance comprehensive brain health research and provide innovative expert care for patients with a wide variety of neurodegenerative diseases, movement disorders and complex neurologic conditions.
With a projected opening of December 2025, the facility will also provide a home to the institution’s many brain health experts and initiatives that serve the growing need for neurological care in the region. Among them: the Glenn Biggs Institute for Alzheimer’s and Neurodegenerative Diseases.
According to Sudha Seshadri, MD, professor of neurology and founding director of the Biggs Institute, the center’s research efforts will benefit from significant recruitment of Hispanics into clinical trials, expanding the nation’s understanding of how brain-related diseases specifically affect what is already the predominant population demographic across South Texas.
The center will also serve as a training venue for medical residents and postgraduate trainees, ensuring the future of sustained neurological care for the community.
The Center for Brain Health will include:
- 75 exam rooms
- 50 faculty offices
- 12-chair non-oncology infusion center
- Outpatient pharmacy
- Dedicated space for research
Among other new patient care developments: an institute on substance use and related disorders, state-of-the-art patient care technology, a specialty care clinic to provide comprehensive dental care for adults and children with complex medical conditions and the opening of a new outpatient and surgery center.
A commitment to substance use treatment
In April 2023, UT Health San Antonio celebrated the grand opening of the 20,000-square-foot Be Well Texas facility, a hub for providing substance use treatment services across the state, where one in 10 people have a substance use disorder but not everyone has the same access to care.
 Be Well Texas offers comprehensive treatment and recovery support for substance use and Mental health services, regardless of ability to pay. In addition to its in-person and statewide telehealth clinical operation, the program coordinates a network of providers treating for opioid and other substance use and providing recovery support services. It brings together addiction medicine specialists, behavioral health experts, researchers and staff members with lived experience in addiction recovery to collaborate and expand access to care statewide.
Be Well Texas offers comprehensive treatment and recovery support for substance use and Mental health services, regardless of ability to pay. In addition to its in-person and statewide telehealth clinical operation, the program coordinates a network of providers treating for opioid and other substance use and providing recovery support services. It brings together addiction medicine specialists, behavioral health experts, researchers and staff members with lived experience in addiction recovery to collaborate and expand access to care statewide.
“We started these programs to provide equitable access to compassionate, evidence-based programs for substance use disorder and people who are using substances,” said Jennifer Sharpe Potter, PhD, MPH, executive director of Be Well Texas.
Potter is also UT Health San Antonio’s vice president for research and founding director of its Be Well Institute on Substance Use and Related Disorders, a pioneering initiative established earlier this year as a center of excellence with national scope for research, clinical and public health programs, and education and community engagement to advance the field addressing addiction and related conditions. It is home to Be Well Texas.
The institute marks a significant milestone in UT Health San Antonio’s commitment to addressing the complex challenges posed by substance use. With more than $50 million in National Institutes of Health, state and other federal funding annually, the Be Well Institute works as a highly integrated and collaborative center across the university and represents a comprehensive framework and programming for advancing the understanding and treatment of substance use disorders.
With support from the National Institute on Drug Abuse Clinical Trials Network and other Federal funding, the work of the institute encompasses research, medical interventions and evidence-based treatments, psychological therapies, social and peer support, counseling on lifestyle changes, follow-up care, and provider training and education as well as many community outreach and educational initiatives.
UT Health San Antonio faculty are likewise at the forefront of addressing substance use issues statewide, including establishing treatment networks, workforce development initiatives and distribution of life-saving naloxone to traditional and nontraditional first responders.
Collectively, what is available at UT Health San Antonio is unique in Texas and ready to be expanded nationally, said Potter.
“The launch of the Be Well Institute heralds a new era of collaboration and innovation in the field of substance use research and care,” she said. “Stakeholders from across the academic, health care and public sectors are encouraged to join us in this vital endeavor as we strive to improve the lives of individuals and communities affected by substance use disorders.”
Better care through technology
Preparation for opening the new UT Health San Antonio Multispecialty and Research Hospital this December has included equipping the facility with technologies to enhance patient comfort and make care more efficient.
Among the advanced features found within will be beds that can reposition a patient without the assistance of a nurse and alert staff if a patient is at risk for falling or attempts to leave their bed.
Virtual nursing is another key feature of patient rooms, where each large-screen monitor serves not only as a television, but also has a microphone and camera so the patient can interact with care providers.
Robots will also roam the hospital’s halls, delivering bottled water, specimens to labs or medications from the pharmacy to nursing units.
Technology is even embedded within the Tom C. Frost Skybridge, completed earlier this year, allowing for lab samples to be delivered quickly and securely between the hospital and the Mays Cancer Center, home to UT Health San Antonio MD Anderson Cancer Center. The skybridge likewise provides a seamless and vital pathway for patients, providers and caregivers to move easily between facilities.
Serving dental patients with special needs
In February, UT Health San Antonio’s School of Dentistry opened its Phil and Karen Hunke Special Care Clinic to provide comprehensive dental care for adults and children with intellectual, developmental, cognitive or physical disabilities, and those with complex medical conditions.
The clinic was purposely designed for individuals with mobility challenges. From arrival to departure, patients and their caregivers find wide corridors outfitted with hand railings and wheelchair bumpers. Each treatment room features adjustable lighting, sound-dampening walls, large screens and sliding barn doors. A multi-sensory room known as the “Zen Den” offers patients a tranquil space to alleviate anxiety and take a break during treatment if needed.
room features adjustable lighting, sound-dampening walls, large screens and sliding barn doors. A multi-sensory room known as the “Zen Den” offers patients a tranquil space to alleviate anxiety and take a break during treatment if needed.
In addition to the specific focus on patient comfort, the clinic provides opportunities for dental and dental hygiene students and residents to gain invaluable experience by rotating through the special care clinic. Under the guidance of experienced faculty members, students can learn firsthand how to tailor dental care to meet the unique needs of each patient.
Specialized continuing education programs are also being developed by the school for practicing dentists. The sessions will provide dentists with advanced techniques, best practices and strategies for addressing the unique needs of those with disabilities and medically complex conditions, enhancing their ability to deliver high-quality oral health care for all patients.
Newest outpatient location opens
In March, UT Health San Antonio opened its UT Health Outpatient and Surgery Center at Kyle Seale Parkway. The five-story, 108,000-squarefoot community medical facility includes primary care and a range of specialty practices. Patients also have access to the latest in diagnostic laboratory testing and convenient imaging services. The location includes an ambulatory surgery center with state-of-the-art operating suites and spacious pre-op and recovery rooms. Learn more at UTHealthCare.org/KSP.
Banking on the brain: Researchers rely on brain donation to find new treatments
The thin man with a fat grin strolled into the conference room with a mischievous confidence. “Is this the brain bank?” he bellowed, almost laughing. “I’d like to make a withdrawal. How much brains can I withdraw?” Transaction-wise, the man, who was attending an informational session on brain donation, will much more likely make a deposit. And that suits Kevin F. Bieniek, PhD, just fine.
Donating a brain is viewed differently than, say, donating a kidney or even body donation. The brain is the seat of the soul, as (philosopher René) Descartes said. Your brain is a special organ. It encompasses the entire sense of person and being.
–Kevin F. Bieniek
With a careful flick of his thumb, Bieniek, assistant professor of pathology and laboratory medicine in the Long School of Medicine, pops the blue lid off a plastic container. Inside are over a dozen pink, carefully freeze-packed slices of a human brain. White clouds of cold air escape from the door of the freezer, where other containers are neatly stacked and stored.
“This is what we need,” said Bieniek, the inaugural director of the brain bank at the university’s Glenn Biggs Institute for Alzheimer’s and Neurodegenerative Diseases. It’s his job to acquire a robust repository of brains for scientific research.
When the Biggs Institute was established in 2017, it was intended to be a comprehensive center that offers patient care, treatment and family support as well as advanced research in dementia and other brain disorders. Without brains, research is limited.
Sudha Seshadri, MD, founding director of the Biggs Institute, points to the central role of the brain bank in battling brain disorders.
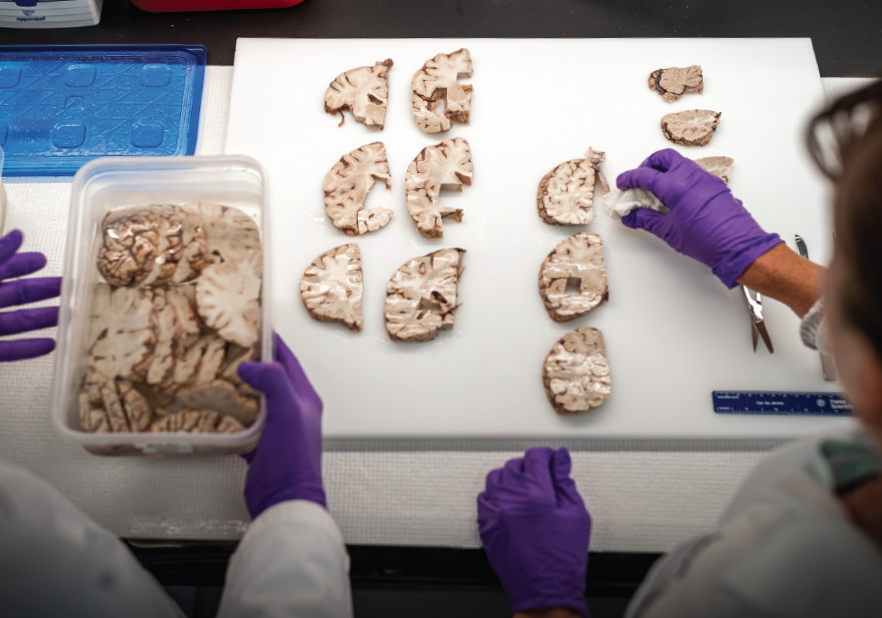
“We believe a deeper understanding of the many biological pathways leading to dementia is essential to finding new drug targets and effective interventions that work,” she said. “Currently, the best method for understanding the molecular and pathological changes in the brain that cause the symptoms of dementia is examination of the brain at autopsy. We study the brain in detail using molecular methods.”
While large brain banks affiliated with medical centers are located predominantly along the coasts, there is a large swath of the country that is highly underrepresented, said Bieniek.
But in 2021, the National Institute on Aging, part of the National Institutes of Health, named the Biggs Institute a designated Alzheimer’s Disease Research Center — the only one in Texas. The designation helps promote research collaboration, encourages data sharing and open science and offers information and clinical trials for patients and families affected by Alzheimer’s and related dementias.
Texas is the second most populous state in the country, has the second highest number of deaths related to Alzheimer’s disease and is home to a Hispanic population that is among the fastest growing demographic segments in the U.S.
“We’re looking to be a resource for the greater San Antonio and South Texas region, regardless of socioeconomic status, race or ethnicity,” Bieniek said. “But ultimately, where we’re unique, is there’s this very large population that really hasn’t gotten the care from Alzheimer’s disease centers that it needs.”
Seshadri echoed that sentiment.
“We know very little about the unique mixtures of brain pathology in Hispanic persons,” she said. “The brain bank will help us make a precise diagnosis in families with the illness in multiple members and help future generations.”
While the decision to donate one’s brain is intensely personal, Bieniek said the reasons often involve care and concern for tomorrow’s patients.
Brain donors and their families want to contribute to research and help future patients, he said.

“It’s this concept called ‘altruism,’ people who recognize that brain donation is a very selfless gift,” he said. “Even in a time of incredible suffering, incredible tragedy, they want their experience and their family’s experience to help benefit society — people they don’t even know — to move that needle, to be the catalyst to that research discovery that will help heal this disorder.”
The need for closure is another motivation for donors, he said.
After the autopsy, “the neuropathology report goes to the next of kin,” Bieniek said. “We’ll say what we did, what regions of the brain we sampled, what we found and where we found it. Then we’ll give a neuropathological diagnosis or diagnoses if there are multiple things going on. And we try to put it all together — ‘What does this all mean?’”
A donor’s family may want to know how the brain disorder might impact other members of the family, he said. Neurodegenerative diseases have different levels of heritability.
“A family might ask, how are we going to approach this disease, how proactive will we be knowing that a specific diagnosis is imminent,” he said. “There may be family planning implications or lifestyle changes.”
While diseased brains are essential, researchers can’t fully understand brain disorders without comparing them to normal, healthy brains.
In his quest for all kinds of brains, Bieniek plans to reach out to memory care centers, nursing homes, hospitals and clinics. But he acknowledged a certain stigma surrounding brain donation.
“Donating a brain is viewed differently than, say, donating a kidney or even body donation,” Bieniek said. “The brain is the seat of the soul, as [philosopher Rene] Descartes said. Your brain is a special organ. It [encompasses] the entire sense of person and being.”
There also may be cultural or religious barriers and misconceptions regarding brain donation to overcome, Bieniek said. For example, donating will not delay or interfere with a traditional funeral or open casket. Also, “most religions view organ donations as valuable to society and an act of charity and love.”
With 222 donations as of March 2023, Bieniek is confident the brain bank will be pivotal in understanding brain disorders.
“The more cases we get, the more powerful studies we can conduct,” he said. “Everything we sample, everything we collect, we save, we archive and we share with our group, with people across campus, across Texas and the U.S. If they have a good idea, if they’re at a qualified institution and we think they have an interesting proposal, then we can provide them with tissue, and that tissue might be the critical step to discovery.”
I’m giving my brain to science. It’s the smart thing to do.

Eleven years have passed since I was diagnosed with an exceptional neurodegenerative disease, a variety of leukodystrophy that researchers tell me is rare among the rare. In fact, what I live with should have claimed my life long before any ultimate diagnosis was made.
before any ultimate diagnosis was made.
Today, I live with a yet-to-be-named form of Vanishing White Matter that has significantly limited my physical abilities, claimed my sight — and immensely expanded my intellect and vision.
When the initial identification of the disease was made and my original neurologist told me, “I don’t know how you have lived this long,” I felt a calling to become a research subject. Then, I realized if I were going to make a genuine difference, I needed to find a postmortem home for my brain and spinal cord.
One morning during what had become a two-year search for a place to donate my brain, a friend called and told me about the Glenn Biggs Institute for Alzheimer’s and Neurodegenerative Diseases at UT Health San Antonio. I contacted them and was grateful to find a welcoming home for my central nervous system.
The reasons for my decision are difficult for some to understand. I am more than my disease. Why did I decide to donate my brain? What do I hope to achieve? Simply this: I want to be the brains behind healing for others.
As far as my wife, Darnice, and I are concerned, it is simply the right thing to do. We felt God was telling us, “Make all of what can be used.” Our adult son advised, “Make it work for you.”
So, in addition to donating key tissue of my central nervous system, I have advocated for rare brain disease research, used my background as a news reporter to lobby state legislators, written and called members of Congress and created support networks among families battling conditions often overlooked in the larger field of health care concerns. As I often tell people, “There is more than cancer and heart disease in the world of medical science.” In all fairness, I truly believe my deep faith in God, along with a wry sense of humor, keeps me going.
A new acquaintance has suggested to me that the difference between donating one’s brain and donating a kidney or a portion of one’s liver, is that in those cases the donor is more likely to see or at least hear about any results for the beneficiary.
When you donate your brain or central nervous system to science, you will never know — at least in this life — how much good will come of it. I suppose the brain donor is really offering hopes, dreams and the potential of promise.
What would I recommend to others in my situation? Have the brains to deliver healing.
Providing novel approaches to trauma
The University of Texas System Board of Regents approved $2.5 million to establish the Trauma Research and Combat Casualty Care Collaborative at UT Health San Antonio in partnership with the Department of Defense and University Health’s Level 1 Trauma Center at University Hospital.
The collaborative leverages longstanding partnerships with University Health and the Southwest Texas Regional Advisory Council, known as STRAC. It will be the first and only one of its kind in the United States, according to UT System.
Trauma is the leading cause of death and permanent disability in children and adults under 44 years of age. The collaborative, which is being called TRC4, will serve to address the critical need for improved trauma care in the United States — both on the battlefield and in the civilian sector — to dramatically improve the care, health outcomes and survival rate for trauma injuries.
“This trauma care research center will save lives and support our dedicated service members,” said UT System Chancellor James B. Milliken. “TRC4 will also create new commercialization and device development opportunities right here in Texas.”
The UT System Board of Regents’ $2.5 million investment in the new trauma care research center matches an initial in-kind commitment toward the project made by the U.S. Army Institute of Surgical Research. The UT System’s investment will cover early start-up costs for the collaborative, which includes hiring executive leadership and administrators, developing the TRC4 strategic plan, establishing the peer review process and providing initial research funding.
The establishment of TRC4 is the latest advancement to come from a partnership launched in 2021 between the UT System and the U.S. Army Futures Command/U.S. Army Institute of Surgical Research. Subsequently, all UT institutions and Institute of Surgical Research leadership approved a legal framework that enables further expansion of their collaborative efforts. This framework was signed by Chancellor Milliken and the Army Futures Command in April 2022.
New therapy reduces headache disability after brain injury
The first therapy developed for post-traumatic headache significantly reduced related disability in veterans following a traumatic brain injury and decreased co-occurring symptoms of post-traumatic stress disorder.
The treatment, called Cognitive Behavioral Therapy for Headache, was appealing to patients, showing low drop-out rates. In addition, it is easy for therapists to learn and deliver. The findings were reported in JAMA Neurology.
“We are excited by this development in the treatment of post-traumatic headache, which along with TBI is poorly understood and for which treatment options are so limited,” said Don McGeary, PhD, associate professor of psychiatry and behavioral sciences in the Joe R. and Teresa Lozano Long School of Medicine. “To find the first major treatment success for post-traumatic headache, which is arguably the most debilitating symptom of TBI, and that the treatment also significantly reduces other PTSD symptoms, is a major breakthrough.”
Both TBI and PTSD are signature wounds of post-9/11 military conflicts, and the two conditions commonly occur together. Post-traumatic headaches, or headaches that develop or worsen following a head or neck injury, become chronic and debilitating in a large percentage of those who experience a TBI, such as a concussion, inhibiting their ability to engage in the activities of daily life. When PTSD occurs with other symptoms, it can worsen the headaches and make them more difficult to treat.
Although effective treatments exist for PTSD, they do not for post-traumatic headache. Migraine medications alleviate the headache pain but do not relieve related disability. They also often have unwanted side effects, and their overuse can worsen headaches.
McGeary and his colleagues developed Cognitive Behavioral Therapy for Headache by modifying a psychotherapy for migraine headaches. It includes key components such as relaxation, setting goals for activities patients want to resume, and planning for those situations.
Cognitive Behavioral Therapy for Headache requires eight sessions of 30-45 minutes each. This is shorter than Cognitive Processing Theory, a leading psychotherapy for PTSD that typically requires 12 sessions lasting 60-90 minutes each. The new therapy teaches patients how to evaluate and change upsetting and maladaptive thoughts related to their trauma.
Those receiving Cognitive Behavioral Therapy for Headache reported significant reductions in disability and in negative impact on function and quality of daily life. They also showed improvement in PTSD symptoms. All of these treatment gains were maintained six months after treatment completion. However, the therapy did not reduce headache intensity or frequency compared to usual care, which can include injections, physical and occupational therapies, pain medications, acupuncture and massage, and long-term medical care.
McGeary said the therapy’s reductions on negative life impact are likely due to its building patients’ confidence that they could control or manage their headaches, a concept known as “self-efficacy.” That sense of control was key to helping patients “get their lives back,” he said.
“If you can improve a person’s belief that they can control their headache, they function better,” McGeary said. “That’s because, when dealing with a long-term, disabling pain condition, people make decisions about whether they’re going to actively engage in any kind of activity, especially if the activity exacerbates the pain condition. They make those decisions based on their perceptions of their ability to handle their pain.”
McGeary believes the planning component of the therapy is key to improving those perceptions.Another benefit of the therapy is that it requires only two hours to train clinicians to provide the care. That would make it relatively easy to increase the number of therapists available to treat veterans with post-traumatic headache and ease caseloads at clinics.