Craniomaxillofacial Surgeon, Multidisciplinary Team Provide Best Care
By Catherine Duncan
Amanda Gonzalez was thrilled when she and her husband, Pablo Gonzalez, became pregnant with their daughter, Anina. When their daughter was born with a cleft palate, they struggled with the exhaustion that comes from having a newborn but also the added stress of an infant who had difficulty feeding.
However, when Anina was only 4 months old, Amanda received the shocking news that she was pregnant again—not something someone who had waited four years to become pregnant expected to receive.
“When we found we were pregnant with our second daughter, we didn’t expect anything to be wrong. We had already gone through that,” Amanda Gonzalez recalls. “We had planned to have a home birth, but she wouldn’t come. I had to go to the hospital and have an emergency c-section.

“When Alessia was born, I remember the room became quiet and heavy. I will never forget that moment,” she said. “They then took her to the NICU where she was put on a CPAP [continuous positive airway pressure] machine because her breathing was so difficult.”
Doctors at the hospital immediately diagnosed Alessia with Apert syndrome, a rare genetic disorder that causes premature fusion of the bones of the skull, hands and feet. It also can cause facial abnormalities and nasal, breathing and speech problems. Within days of her birth, tests confirmed the initial diagnosis.
Although Gonzalez had undergone sonograms while pregnant, none revealed Alessia’s condition. “The Apert community is close-knit around the world. I have learned it is hit or miss if a mother finds out because of a sonogram. Many of us have no idea until after our child is born. We were referred to UT Health San Antonio’s Craniofacial Clinic. We soon became very familiar with the many specialists who are caring for our child.”
One of those specialists is Mark A. Miller, DMD, MD, FACS, pediatric cleft and craniomaxillofacial surgeon and clinical director of oral and maxillofacial surgery for the School of Dentistry at UT Health San Antonio. Dr. Miller, an assistant professor of oral and maxillofacial surgery, neurosurgery and pediatrics, has worked with a multidisciplinary team from across the university to care for Alessia.
Dr. Miller said he was recruited by Edward Ellis, DDS, MS, chair of oral and maxillofacial surgery, so the team would have a craniofacial surgeon in the School of Dentistry. Dr. Ellis had worked with the Department of Neurosurgery in the Long School of Medicine on campus to coordinate Dr. Miller’s arrival so he could work with the pediatric neurosurgeon, Izabela Tarasiewicz, MD, FRCSC, who operates on children at University Hospital, the medical school’s main teaching hospital.
Dr. Tarasiewicz is an associate professor of neurosurgery who is cross appointed in pediatrics and oral and maxillofacial surgery. She specializes in pediatric neurosurgery with a focus on the management of spinal dysraphism and congenital malformations of the central nervous system. “Dr. Miller and I share a mission to redefine the standard of care in South Texas for simple and complex craniosynostosis with the most cutting-edge techniques,” Dr. Tarasiewicz said.
Dr. Miller said he first saw Alessia when she was 6 months old, which was shortly after he moved to San Antonio. “I had just started at the School of Dentistry and was still completing my fellowship” in pediatric craniomaxillofacial surgery from the Arnold Palmer Hospital for Children in Orlando, Florida, he recalled. “She was one of the very first patients I saw after joining the faculty. At that time, Dr. Tarasiewicz had already performed a minimally invasive procedure to relieve the pressure on her brain because of the fused cranial bones,” he said.
Dr. Tarasiewicz said she met the Gonzalez family shortly after Alessia was born. “She was born with craniosynostosis, a congenital defect in which the bones in a baby’s skull join together too early. This creates a restriction of her head growth,” she said. “I performed a minimally invasive endoscopic release to open up the sutures. I did this for Alessia when she was 4 months old because her sutures were closed. I opened them to allow her brain the room it needed to grow.”
Alessia then went to UT Health San Antonio’s Cranial Remolding Program to be fitted for a helmet that she wore while her head healed. Clinical Director Darren J. Poidevin, CLPO, is a licensed orthotic/prosthetic practitioner who cared for Alessia at this time.
As follow up to the initial procedure, Alessia was seen regularly at UT Health’s Craniofacial Clinic at University Hospital. Gonzalez said Alessia has had multiple other procedures, including ones on her nasal passage and fingers.
“As a patient, she is one of those babies who bounces back. The nurses would say they love how sassy she is. She really has a stubborn will; that serves her well with what she has to deal with in life,” Gonzalez said.
By age 2, Alessia was starting to have issues, including one of her eyes not being able to close properly because of pressure inside her skull.
Dr. Miller and Dr. Tarasiewicz, who together had continued monitoring Alessia as she was developing and growing, conferred with Martha Schatz, MD, pediatric ophthalmologist and clinical professor of ophthalmology, and Marisa Earley, MD, pediatric otolaryngologist and associate professor of otolaryngology-head and neck surgery, about scheduling an invasive surgery called a frontal orbital advancement in April 2019 when Alessia was 26 months old.
The team follows the parameters of care as designated by the American Cleft-Palate Craniofacial Association for which Dr. Miller sits on the national membership committee. “There comes a point where the initial minimally invasive technique bridges the maximum of its benefit. Then Alessia needed the next surgery. We know with Apert syndrome there are multiple surgeries that are needed as a child develops. The next one is a frontal orbital procedure. Because of the positions of her eyes and the health of her eyes, it was necessary to move forward,” he said.
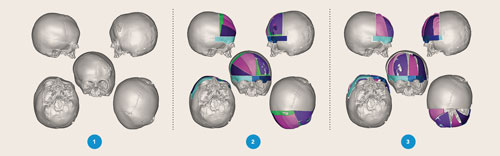
Dr. Miller said the process begins with a CT scan of her head that is then put through a 3-D system so a model of her head can be created. “We look at the bones of her skull. Next, we meet with a biomedical engineer, and we superimpose her skull on a normalized skull. We look at how we can get Alessia from where she is now to a more uniformed head shape.”
“We start planning our craniotomies, which are the surgical cuts in the skull, and figure out how we are going to bring her skull into a more normal shape. I use the model of the skull to design how I am going to rearrange the pieces of skull to create a more acceptable configuration. Each piece is then precisely removed and adapted so we can follow the exact plan.”
Dr. Miller said once he knows where he wants to move the pieces, he fabricates guides that will show him how to replicate the cuts that he has done virtually. This patient specific planning allows Dr. Miller to create a simulated surgical plan virtually. “Intraoperative time is so much lower because I can achieve exactly what I plan using these patient specific planning tools for cranial cases,” he said.
After the incision from the top of each ear to the other ear, the guide was placed on to her skull. “The plating guide was preprinted to match her anatomy perfectly. I can look at vascular structure—markings show me where the vascular areas to be avoided are located—to know where we need to modify our reconstruction in the safest manner possible.”

“The guide shows Dr. Tarasiewicz exactly where I want her to make these craniotomies. Then Dr. Tarasiewicz removes these bony pieces. I then reconstruct cranial grafts into their planned configuration. I modified her frontal orbital bando to meet the more normalized anatomy. We use screws and plates that will reabsorb over time,” he said.
Dr. Miller, who said few centers in the country are using this technology, said that after surgery, Alessia’s skull is virtually identical to the plan he had created prior to the surgery. “Immediately post op you can see the drastic difference,” he said.
According to Dr. Miller, there are several benefits to using the patient specific planning and 3-D model guide: The entire surgery can be stimulated before anyone walks in the operating room; the surgeons can identify issues that they may have not seen until the operation was underway, including vascular issues and anatomical interferences; surgeons are very precise during the procedure because the patient’s skull has been superimposed on a more normalized skull which helps them try to match that anatomy; and less time in the operating room means less blood loss for the patient.
“For these procedures, nearly 100 percent of these patients need blood transfusions. Our transfusion amounts are much lower because the virtual planning speeds up our surgery by a couple of hours,” he said.
Dr. Miller said that University Hospital is on board 100 percent with the virtual plan. “This is not an inexpensive planning technique but with what we save the patient in morbidity, being on the table longer, and anesthesia time, the cost is not different. This may cost a few thousand dollars to plan and create the guides, but it costs more to be in the OR for that many more hours,” he added.
Gonzalez said she was amazed at how well her daughter did after the invasive procedure. “Shortly afterward, she was eating apple sauce. Then she was crawling on the floor and smiling at everyone. This kid is made of steel.”
Dr. Miller said the team has had really great results with Alessia. “She has gotten the most value from the surgeries because of how we staged them. By giving her minimally invasive releases, which most centers do not offer, at 4 months of age, we delayed Alessia’s actual frontal orbital advancement until she was 2½ years ago. That is unheard of.
“Normally this big surgery would have been done when she was 9 to 11 months. Then the likelihood of needing to redo that surgery is much higher because so much cranial growth occurs during the first two years of life. Kids’ skulls are 90 percent grown by 6 years of life. We are getting her through these early years with one minimally invasive procedure and one open procedure,” Dr. Miller said.
The team is monitoring her to determine when to do more procedures in her future. “We repositioned the top part of her orbits, but we will need to reposition the bottom parts of her obits. Mid-face growth is also affected. When she is older, we will probably have to do a subcranial Le Fort III osteotomy. She may also need another jaw surgery when she is done growing.”
Gonzalez said as a mother, it is scary knowing Alessia, who turns 5 in January, has more surgical procedures ahead of her. “Dr. Miller has explained the mid-face advancement to us. Alessia has a high-arch palate. This procedure will help with jaw alignment so it will be easier for her to be able to eat.”
The entire UT Health San Antonio team has already made such a difference in Alessia’s life, she said. “From the School of Dentistry to all of the medical team members, they all told us they would take great care of her. I always feel good when she is with Dr. Miller and the other specialists.”
As an active member of the global Apert community, Gonzalez said she sees Apert children who have had surgery at other hospitals around the world. “I don’t think everyone gets the kind of care that we are fortunate to have here. I’m so glad we are at UT Health where all these specialists work together. And, not one of these doctors has ever told us, ‘She’ll never be able to do this or that.’ They always tell me she will thrive. UT Health has given us hope for Alessia’s future. Every day I am thankful.”
Gonzalez said she must mention that all of her children have benefited from UT Health San Antonio. Her 19-year-old son, who is now in the U.S. Air Force, came to the orthodontic clinic for his braces.
The couple’s older daughter, Anina, underwent surgery to repair her cleft palate at age 1. The surgery was performed by Christian Stallworth, MD, facial plastic surgeon with UT Health Physicians. At the same time, Dr. Earley performed an ear tube procedure on Anina. Coincidentally, Dr. Earley, a pediatric otolaryngologist, has also operated on sister Alessia.
Dr. Miller stressed that the team is able to achieve these results because of working in a multidisciplinary, collaborative environment that only an academic medical center can provide.
“This collaboration allows us to treat these patients the way we do. We’ve got pediatric otolaryngology, pediatric ophthalmology, pediatric craniofacial surgery, pediatric dentistry, orthodontics and pediatric neurosurgery all taking care of this one child to give her the best and brightest future she can possibly have. We are super excited about where she is now and where Alessia is headed,” Dr. Miller added.





